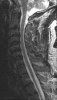
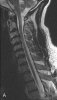
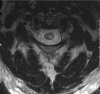
Actually, I wasn't thinking about the technical aspects of the procedure...as with my discussion with Dr. Gilula...there are a multitude of ways to get into the foramen....
I was thinking about an alternate differential...imagine that you were at the patients bedside
1. subdural injection (delayed onset of neuro sxs)
2. subarachnoid injection (relatively quick onset of neuro sxs)
the above are unlikely, because the patient was still breathing and apparently conscious and I am assuming that they did not become hypotensive
1. intravascular...
unlikely because the patient did not seize or become obtunded
in any event, I do not know why they would use 0.75% bupivacaine...at least if you are going to use such a high concentration use levo-bupivacaine or ropivacaine or use a lower concentration of bupivacaine
as far as the technical aspects of the procedure:
nothing in the cervical foramen is safe..it is a busy area...I emailed Huntoon and apparently, even the dorsal inferior cervical foramen is vulnerable....(see the abstract below) and I would encourage you to read an article in Spine 1996 by Oga regarding the tortuosity of the vertebral artery.
although efforts to CTFESIs safer, such as optimal views and DSA, seem logical....we will never be able to see every image/technical approach that every practitioner in the USA...one must assume that not all these practitioners are experts and not all their patients are ideal...thus, the fact that complications are not approaching a 10-20% rate, but probably are in the .001% range, suggests that our bodies are very forgiving to foreign insults. Grey Water is correct that there is no evidence...but there never will be evidence that optimal views/DSA are the way to go...you are asking to perform a study wherein we want to reduce the rate of complications from 0.001% to 0.00001%.
additonally, the recognition of vascular uptake ultimately depends on the resolution of the human eye...DSA is not a microscope looking at blood vessels....it depends on the mag capabilities of the fluoroscope...hence, really small vessels, smaller than the caliber of a 25 or 27 gauge needle may be responsible for complications..and these could be missed...criticising a practioner for not using DSA is like being a monday morning quaterback
think about all the other things one can use to criticise a practitioner who has a complication:
If you have a heavy smoker, multilevel cervical spinal stenosis without myelopathy but vague non discrete radicular signs, and a short thick neck or a patient with a multilevel anterior fusion....odds are the vascular anatomy will be abnormal and that there will be some vascular disease....now if you do a cervical transforaminal....you will need someone to pull down the shoulders and you will probably need a swimmer's view....also if you use a small caliber needle (25 gauge), it will be deflected from dense fibrous (in these patients) tissue and will be more difficult to steer the deeper you go...common sense suggests that we should not perform CTEFSIs in this population..but we do, don't we? Now, if a complication occurs, can the practitioner be faulted or are we being speculative and trying to create a story for the events that led to the complication.
should we demand the use of needles with calibers in the 18-22 gauge range
should we demand the use of blunt needles
should we demand a posterior approach
should we also demand the use of a stimulating needle with impedance checks...high impedance fluctations suggest intravascular injection? low voltage stimulation may suggest intraneural injections?
should we demand a test dose with epinephrine?
should we use the auscultatory test, such as described by Leighton to detect intravascular injections in OB patients...auscultate the heart to listen for air bubbles...I can't remember if she used portable dopplers
even then, complications may not occur even when all these safety stops are removed...the ISB approach ala Winnie with paresthesia elicitation (sharp needle in the brachial plexus) rarely results in disastrous complications...imagine an intraneural injection of high doses of local anesthetic
also, is imaging needed?...Boezaart's new approach to the brachial plexus...in volves advancing a sharp stimulating needle in an upright patient, blindly, till the needle hits the distal C6 transverse process and then injecting high dose local
common sense to one individual may be different to another...and common sense should not be codified into standards
so, should we be dogmatic about our common sense and then show up as an expert witness and slam the practitioner's incompetence (didn't use optimal views, didn't use DSA), when we know that the vast majority of practitioners are probably practicing in the same way as the defendent..or should we fess up as a community of pain doctors at large and say.....
cervical transforaminal procedures are potentially dangerous, but we advocate them anyway...in fact the irony is that even 'monkeys' can do it, but dangers can occur, independent of whether you are a monkey or an expert monkey.
it is hypocritical to endorse a technique that can be taught at a weekend course and then state that this procedure should only be performed by 'experts' and in only specific ways..also it is irresponsible to demand that practitioners rigorously understand anatomy...knowing the anatomy in a cadaver cannot prepare you with every possible anatomic variation...even then, fluoroscopy cannot provide all the information needed to make CTFESIs safe all the time...
at some point, we have to have faith in fellow physicians that they are trying their best...and assuming there wasn't gross or malicious incompetence, we have to assume they did the best they could in order to avoid complications and we should exercise an open mind that there are a number of ways to do the procedure safely.
t
<snip>
A-1140
October 26, 2004
3:30:00 PM - 5:00:00 PM
Room Hall C2-4
The Ascending and Deep Cervical Arteries Are Vulnerable to Injury during Cervical Transforaminal Epidural Injections: An Anatomic Study
Marc A. Huntoon, M.D.
Anesthesiology, Mayo Clinic College of Medicine, Rochester, Minnesota, United States.
Background: Corticosteroids are commonly injected in the cervical epidural space as a treatment for radiculitis. Traditionally, epidural corticosteroid has been injected via an interlaminar approach, but the transforaminal approach has become prevalent. Recent case reports (1,2) of anterior spinal cord infarct and death have elicited safety concerns for the transforaminal approach.
Methods: In this prospective anatomic study of 10 embalmed cadavers, the relationships of the spinal roots, blood supply from the vertebral, ascending cervical and deep cervical arteries supplying radicular or segmental medullary anastamoses were examined. Specific areas of vulnerability to needle trauma in the posterior (dorsal ) foramen were examined. Arterial origin , outer diameter, location and foraminal distribution were documented.
Results: In 5 dissected cadavers of 10 planned, 3 of the 5 have arteries that are vulnerable to needle injury during a standard dorsal middle transforaminal injection. In a female cadaver a large branch of the deep cervical artery arising directly from the subclavian arch on the right passes ventral to the C7 nerve root before diving under the C6 root in the dorsal aspect of the intervertebral foramen. This vessel is vulnerable to needle injury from transforaminal placement. The vessel measures 1.6 mm, compared to the 3.0 mm vertebral artery . The deep cervical supplies segmental medullary blood to the anterior spinal artery. In a second (male) cadaver, an ascending cervical branch from the right thyrocervical trunk passes ventral to the C7 root then passes through the dorsal aspect of the C6 foramen, continues ascending to the dorsal aspect of the C5 foramen then trifurcates into a segmental medullary vessel as well as ascending branches. The artery is 1.0 mm compared to the 3.5 mm vertebral artery , and appears to be very vulnerable at C5 and C6. In a third male cadaver, a radicular branch of the deep cervical artery is vulnerable at the dorsal aspect of the C7 root.
Discussion: A recent case described a near -miss during a C7 transforaminal injection in which a segmental medullary pattern of contrast spread caused the authors to abort the procedure.These authors are aware of 6 more cases of spinal cord injury that are sub judice and not yet reported. (3) Previously, Brouwers et.al. had described a fatal transforaminal injection at C6.(1) More recently, Ludwig et. al. reported an anterior cord ischemic event associated with a C6 root injection (2). A prospective study of 504 transforaminal cervical injections documents a 19.4% incidence of contrast confirmed intravascular injection. (4) It is known that the inferior cervical segmental medullary blood supply may come from branches of the ascending and deep cervical arteries, and that some variability exists.(5) Our study demonstrates that the C5, C6 and C7 areas may be most vulnerable to needle injury, with ascending and deep cervical arteries in the presumed safe area of injection, dorsal to the nerve root and vertebral artery. As blood supply is variable, transforaminal injections in these cervical foramina may be innevitably high risk.
References:
1. Brouwers, et.al. Pain 2001; 91:397
2. Ludwig, et.al. Arch Phys Med Rehab 2003; 84:E37
3.Baker, et.al. Pain 2003;103:211
4.Furman et.al. Spine 2003;28:21
5. Gillilan. J Comp Neurol 1958;110:75
Anesthesiology 2004; 101: A1140