I am neither old enough, nor an anesthesiologist
but, I have heard that when fluoroscopy was first coming onto the pain scene, the older anesthesiologists criticized the younger ones that wanted to use XR to perform pain procedures. they said, "what, you can't feel it? didn't we train you to use your hands? this is the ART of medicine" yada yada yada
then real studies were performed and we found that the "blind" injections were in the wrong place up to 40% of the time.
Any imaging modality is more accurate than palpation approach. this has been demonstrated dozens of times. US > palpation. fluoro > palpation. US = fluoro for joints. US infinitely better than fluoroscopy and palpation for soft tissue injections when your target is nerve, a tendon sheath, etc and avoiding structures you don't want to hit - viscous, lung, etc. When nerve stimulators were first used to perform peripheral nerve blocks, and injectate volumes dropped from 10-20 ml to 5-10 ml to perform the same block, I would argue that using US provides ability to perform these procedures in much safer ways.
As good as we all want to believe we are, and as good we all think we are in being 99.999% accurate, the studies show a much different reality. global satisfaction, VAS do not pan out 1:1 with accuracy in many studies as Steve is alluding to, but to not strive for the highest accuracy with our injections goes against one of the basic principles of our profession.
As physicians I am sure we all take pride in Accuracy and Precision. This is also why we do specific nerve root lesion injections vs caudal esi or oral steroids. and I would remind you, this is the basic tenet many of you ascribe to, to isolate the painful lesion down to the single medial branch...
Ultrasound does not pay very much. and if you spent the time to learn how to use it, you will find that it is an INCREDIBLY USEFUL tool. it is not only used for guidance for injections. as a brief example, I was teaching a course 2 weekends ago to a group of 3 anesthesiologists, ACGME trained pain physicians with over 60 years of combined experience. one of them brought in his family member with posterior knee pain. This person had already been evaluated by multiple specialists, MRI x2, was then seen at the big state university where orthopedics did not find anything wrong with his knee. People always bring these folks to me and ask me to, "just take a look and tell us what you see" it is not easy, nor do I welcome it. I am not trained as a radiologist, and if these specialists could not find the root of the problem with MRI, i doubt I can either.
one beauty about US is something people call, "soon-auscultation." meaning, you put the probe directly over where it hurts. this is a HUGE advantage over MRI. you can also move the painful part of the body around in real-time, vs static imaging.
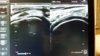
i placed the probe over where it hurt, and after a brief survey of the area was able to find a hypo echoic area within a tendon. i traced this tendon caudally until it turned into a muscle: his medial gastrocnemius. i saved some nice images, and made sure that I could easily reproduce that hypo echoic area in the tendon so that I was not fooling myself. then i looked at the same area on his contralateral and unaffected limb. i found the same area of the leg. the insertion of the medial gastroc tendon on the distal posterior femur. it looked beautifully normal. (see attached image)
Again, you can do a lot of things with ultrasound. the economics of it are negligible. $30 for the code is actually a waste of my time and a drop in the bucket compared to the $12 tylenol in the hospital. I don't expect everyone who uses US to want to learn how to use it to it's full potential. nor do I expect everyone to do cervical/lumbar RF with the parallel approach even if I think it's the best way to do it.
in that same group of 3 physicians i taught recently, i was able to demonstrate to them how within their small sample size of 3 how you have completely variable anatomy. one person had a bifid median nerve, one had a median nerve much more ulnar than typical. when evaluating their necks, one had dozens of thyroid nodules that were identified which needed to be further evaluated, another had esophagus on the left, while the others had them on the right, etc
to go back to my argument on the superiority of US over fluoroscopy for soft tissue injections, i will mention a example of a procedure commonly performed with both US and fluoroscopy. for stellate ganglion block, i teach 3 approaches depending on the anatomy that is found. Trans-thyroidal, trans-jugular, and an in-plane lateral to medial approach. for most practitioners, they have 1 approach to this injection with fluoroscopy. there is no way to evaluate the anatomy for inferior-thyroidal arteries, ascending cervical arteries, visualization of the cervcal nerve roots, esophagus, etc. these are some of the structures that have been violated and published as complications in performing stellate ganglion blocks (retropharyngeal hematoma compromising airway, abscess from esophagus etc). Mind you, I am ACGME Pain trained and can do these with fluoroscopy as well but choose not to as I find US to be a much safer approach. and Yes, I can do them with both modalities to evaluate for contrast flow.
If you take the time to want to develop US as a skill, it is a fantastic tool.