- Joined
- Mar 31, 2008
- Messages
- 1,899
- Reaction score
- 2,762
Thoughts?
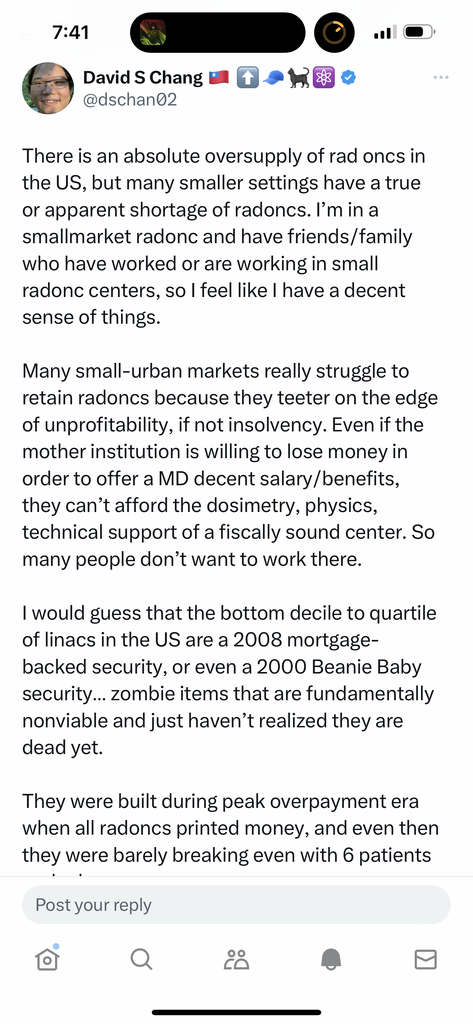
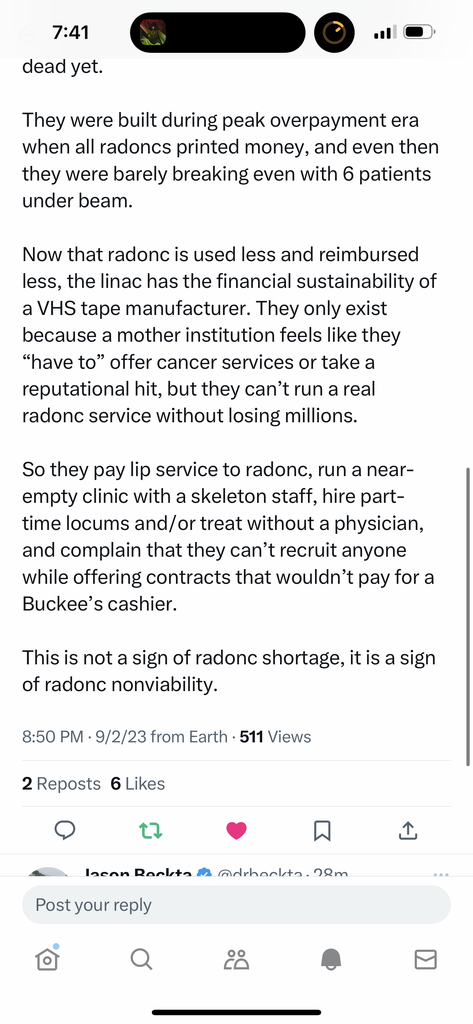
This doesn't ring true to me. I work in a relatively small town area, distant suburb from large metros but small enough to be considered rural. My practice is very viable and profitable for the hospital. Many of my friends/acquaintances from residency are in similar situations and also gainfully employed running profitable departments. Perhaps what he is describing is accurate in the true BFE rural settings, but I just don't see this level of dysfunction (yet), at least from my vantage point in the midwest.
How sustainable is that with the reimbursement landscape and hypofx?Agree. I'm a WASP male that hates living in a city. I don't mind the suburbs but would rather be in the country. I still want to be within 2 hours of a large airport though.
There are definitely rural practice settings in need that will make very good offers... it just might not be in your preference of the 4 geographical regions of the US. (NW, SW, NE, SE) And if its hospital owned; that offer might change the moment the hospital administration changes.
Not saying med students shouldn't apply... just be ready to be flexible.
At least you won't have to round though.
I am not American, but the way I read the argument, it obviously has to do with 2 factors:This doesn't ring true to me. I work in a relatively small town area, distant suburb from large metros but small enough to be considered rural. My practice is very viable and profitable for the hospital. Many of my friends/acquaintances from residency are in similar situations and also gainfully employed running profitable departments. Perhaps what he is describing is accurate in the true BFE rural settings, but I just don't see this level of dysfunction (yet), at least from my vantage point in the midwest.
Europe is safer due to the centralization of care ie every hospital doesn’t have a linac.I am not American, but the way I read the argument, it obviously has to do with 2 factors:
- compensation models
- patient load
In the golden era of radonc, a practice could sustain itself even with a small amount of patients on beam, because:
- Overall costs for personell (other than doctors) were lower than today and there were people willing to take those jobs even with not a high salary
- Fractionation was different. Having 8 prostate patients on beam, meant that with 40 fractions, you only need to start one new prostate patient per week, in order to keep 8 prostate patients on beam at any time. This meant an overall low burden for consults, contouring, planning and QA.
- compensation was different
This apparently led to a many practices being funded that are now finding themselves competing for the same patients.
Add to that
- overall decline in utilization of RT for the two main indications (breast & prostate)
- patients willing to travel more for treatment (including protons)
and you likely now have an oversupply.
It is bound to happen in Europe too at some point, the US is simply one (or more) steps ahead, as usual.
Agree with some others above, this doesn't ring true for me.
When it comes time to replace a linac, the sh hits the fan and true costs become apparent. It is easier to make this assessment when you are running a very old linac w/crap software and not accounting for up front investments.Agree with some others above, this doesn't ring true for me.
The technical side of Rad Onc still pays very well and you need very few patients on treatment to remain a profit center for the hospital.
The key here is how much the hospital feels obligated to be pay the physician and what salary it takes to convince someone to take the job. That's what's changing with oversupply.
for the same salary, I would rather have a job like that than 10 pts on treatment.I think the most important thing to consider when we discuss anything of this nature:
Do not approach American Healthcare Economics with objectivity or rationality.
While "America" is a country, the highly regulated market of Medicine can vary widely from state to state. We can't even have a single national medical license, which is like, the base unit of the Healthcare Enterprise.
In a vacuum: RadOnc remains viable, even with low "on beam" numbers, if you break it down into component parts.
But...that doesn't reflect reality. As a thought experiment: what would it take to even out the maldistribution of care? There are 35 states with Certificate of Need laws (and a few more that have the functional equivalent) - could we even get a new linac location off the ground? Not without significant effort and expense.
Ok, let's say we get approval. How much capital do we need? Obviously the cost is extremely variable, but I've been involved in this for the past year, and I can say that a new linac (with installation) will cost about $2.7-$3.0 million dollars.
That's if you already have the vault and the department around the vault. We're talking another $1-$2 million easy if we have to build from nothing.
Alright, so $5 million dollars upfront. Let's say we secure funding and actually get this thing built, which would take at least 1-2 years.
Has anyone tried to hire...any staff lately? It's nuts. And especially if you're not in a "desirable" area.
You're going to be very hard-pressed to find anyone willing to dump that kind of cash and effort into a project if the end result is 5-10 "on beam" afterwards, the ROI on that is...never? Who knows.
But ok, let's say it's not a new build.
Now we're up against our good friend, consolidation. Yes, the technical side of radiotherapy still gets a decent amount of reimbursement - but who's in control of it? Administrators who are able to see the bigger picture, and allocate resources effectively? Hahahaha...no.
I work in a very "resource poor" hospital. I'm the only Radiation Oncologist. I don't have permanent physics - we contract a private group. I have a single 0.9 FTE Dosimetrist. I have a total of 3 therapists: two full time, one part time. I have a Medical Assistant and a single RN.
And I have crazy volume. I break 30 on beam, and usually stay in the 20's.
For those in practice trying to do the math: no, the numbers don't add up. We don't have anywhere close to the necessary resources. It's bad.
Through sustained and obnoxious effort on my part, the hospital is starting to invest more to at least bring us up to a minimally safe level. Except...we have no applicants. We've had a therapist job open for 6 months. We've had two people apply. Both ghosted us. We spent months entertaining a physicist who expressed interest in coming here. Also to be told...nope.
I think it's obvious, based on my SDN track record, that I have an intense, borderline obsessive interest in Radiation Oncology. The only reason I can stick this out is a combination of my uncommon skillset (not too many early career generalists who understand billing and can plan their own VMAT cases) and family ties in the greater region. This would absolutely be "churn-and-burn" otherwise.
For those of you who don't know what I'm talking about, who have stability and sufficient resources in a "slow" practice: I'm genuinely happy for you. Please hold on to your jobs and stability for the sake of your patients.
But I promise you - jobs like mine are more common than you think, and the "insolvency" of RadOnc is not getting any better, even if the math "works out" on paper.
Yeah...I’m
for the same salary, I would rather have a job like that than 10 pts on treatment.
But do you know how to clear a jammed Glock when shooting soda cans in the woods with cheap, steel jacket Russian ammo?Hmm
I like syrup and ice skiing
No, but I’ll eat Ben and Jerry’s, listen to Phish and Noah Kahan and get some Cabot cheddarBut do you know how to clear a jammed Glock when shooting soda cans in the woods with cheap, steel jacket Russian ammo?
Do you have an opinion on the curing process for hardwood vs softwood?
These are anti-biryani jokes.Are these biryani jokes that I don’t understand?
Very well said, but I think the problems you describe are more "rural hospital problems" than rad Onc problems.I think the most important thing to consider when we discuss anything of this nature:
Do not approach American Healthcare Economics with objectivity or rationality.
While "America" is a country, the highly regulated market of Medicine can vary widely from state to state. We can't even have a single national medical license, which is like, the base unit of the Healthcare Enterprise.
In a vacuum: RadOnc remains viable, even with low "on beam" numbers, if you break it down into component parts.
But...that doesn't reflect reality. As a thought experiment: what would it take to even out the maldistribution of care? There are 35 states with Certificate of Need laws (and a few more that have the functional equivalent) - could we even get a new linac location off the ground? Not without significant effort and expense.
Ok, let's say we get approval. How much capital do we need? Obviously the cost is extremely variable, but I've been involved in this for the past year, and I can say that a new linac (with installation) will cost about $2.7-$3.0 million dollars.
That's if you already have the vault and the department around the vault. We're talking another $1-$2 million easy if we have to build from nothing.
Alright, so $5 million dollars upfront. Let's say we secure funding and actually get this thing built, which would take at least 1-2 years.
Has anyone tried to hire...any staff lately? It's nuts. And especially if you're not in a "desirable" area.
You're going to be very hard-pressed to find anyone willing to dump that kind of cash and effort into a project if the end result is 5-10 "on beam" afterwards, the ROI on that is...never? Who knows.
But ok, let's say it's not a new build.
Now we're up against our good friend, consolidation. Yes, the technical side of radiotherapy still gets a decent amount of reimbursement - but who's in control of it? Administrators who are able to see the bigger picture, and allocate resources effectively? Hahahaha...no.
I work in a very "resource poor" hospital. I'm the only Radiation Oncologist. I don't have permanent physics - we contract a private group. I have a single 0.9 FTE Dosimetrist. I have a total of 3 therapists: two full time, one part time. I have a Medical Assistant and a single RN.
And I have crazy volume. I break 30 on beam, and usually stay in the 20's.
For those in practice trying to do the math: no, the numbers don't add up. We don't have anywhere close to the necessary resources. It's bad.
Through sustained and obnoxious effort on my part, the hospital is starting to invest more to at least bring us up to a minimally safe level. Except...we have no applicants. We've had a therapist job open for 6 months. We've had two people apply. Both ghosted us. We spent months entertaining a physicist who expressed interest in coming here. Also to be told...nope.
I think it's obvious, based on my SDN track record, that I have an intense, borderline obsessive interest in Radiation Oncology. The only reason I can stick this out is a combination of my uncommon skillset (not too many early career generalists who understand billing and can plan their own VMAT cases) and family ties in the greater region. This would absolutely be "churn-and-burn" otherwise.
For those of you who don't know what I'm talking about, who have stability and sufficient resources in a "slow" practice: I'm genuinely happy for you. Please hold on to your jobs and stability for the sake of your patients.
But I promise you - jobs like mine are more common than you think, and the "insolvency" of RadOnc is not getting any better, even if the math "works out" on paper.
Absolutely!!!Very well said, but I think the problems you describe are more "rural hospital problems" than rad Onc problems.
I bet they have to pay surgeons boatloads of "premium" to keep them in the area similarly, and I'm sure the surgical services are complaining just as much about trying to keep nursing staff on board. As you said staffing across the system is tough because of location. I bet that as far as revenue goes rad Onc still looks relatively favorable, especially since you're quite busy (and understaffed). They've probably kept it that way because they 1) didn't know better and 2) didn't have the right kind of advocate
This is the point. Non-viability as described in the original post really just means non-viability of smaller scale, locally controlled radonc. It does not refer to large centers doing radonc.Europe is safer due to the centralization of care ie every hospital doesn’t have a linac.
FWIW, RBE is less important for SBRT/hypofx than for standard fractionation. Higher LET cell kill has a greater alpha component (and therefor a lower a/b ratio) thus RBE gets closer to 1.Meanwhile, proposing proton carveouts and promoting ultra-hypofractionation (again not applicable to protons as they don't know how RBE scales with dose per fraction) are strictly consolidate care in large or medium sized metro type initiatives.
I was under the impression that RBE with protons is not an issue outside of the immediate area just at the end of the Bragg peak and generally considered to be around 1.1.FWIW, RBE is less important for SBRT/hypofx than for standard fractionation. Higher LET cell kill has a greater alpha component (and therefor a lower a/b ratio) thus RBE gets closer to 1.
I was under the impression that RBE with protons is not an issue outside of the immediate area just at the end of the Bragg peak and generally considered to be around 1.1.
RBE is the main issue with heavy ions and totally unpredictable depending on tissue.
I also do not agree with the statement that RBE is less important in the setting of hypofractionation.
Those mini spots of very high RBE in protons are not in the same region every day. Interplay effect comes here into action.
So if you are treating a prostate with 40 x 2 Gy with protons, a 140% hotspot of 2 Gy (-->2.8 Gy) at the end of Bragg peak will not be on the same spot every day. Which is probably ok.
Now, try an ultrahypofractionation schedule with protons and use 8 Gy per day. That 140% hotspot just became a 11.2 Gy hotspot...

I would hope so, but I'm skeptical (as you know). One of the features (and bugs) of proton therapy is the differential LET as you follow a beam through tissue. That far side of the Bragg peak becomes a cluster, and I suspect very biologically sensitive. Your prescription dose may look like you're in a regime where RBE is getting towards one (largely because you are just giving so much dose that discrete biological mechanisms of repair are overwhelmed), but there is always a low dose portion of the plan with lots of uncertainty. (again the fact that getting numbers in cell culture experiments is difficult is evidence of highly variable RBE).Would say that this effect would offset the impact of LET/interplay to some extent.
Bias being that SBRT protons bills for SBRT (same as photon plan).I would hope so, but I'm skeptical (as you know). One of the features (and bugs) of proton therapy is the differential LET as you follow a beam through tissue. That far side of the Bragg peak becomes a cluster, and I suspect very biologically sensitive. Your prescription dose may look like you're in a regime where RBE is getting towards one (largely because you are just giving so much dose that discrete biological mechanisms of repair are overwhelmed), but there is always a low dose portion of the plan with lots of uncertainty. (again the fact that getting numbers in cell culture experiments is difficult is evidence of highly variable RBE).
Are there proton protocols out there pushing for 1-5 fractions? Even in the liver (my favorite spot for protons) protocols that I have seen, not seeing protocols below about 10 fractions?
LU008 may allow it... would have to double checkI would hope so, but I'm skeptical (as you know). One of the features (and bugs) of proton therapy is the differential LET as you follow a beam through tissue. That far side of the Bragg peak becomes a cluster, and I suspect very biologically sensitive. Your prescription dose may look like you're in a regime where RBE is getting towards one (largely because you are just giving so much dose that discrete biological mechanisms of repair are overwhelmed), but there is always a low dose portion of the plan with lots of uncertainty. (again the fact that getting numbers in cell culture experiments is difficult is evidence of highly variable RBE).
Are there proton protocols out there pushing for 1-5 fractions? Even in the liver (my favorite spot for protons) protocols that I have seen, not seeing protocols below about 10 fractions?
Bias being that SBRT protons bills for SBRT (same as photon plan).
Similarly, fewer proton fractions doesnt compare as well financially to more fractions, and 10vs 15 treatments really isnt that much different for the patient (and data/individual experience is more robust for 15 fraction treatments). There really isnt a scenario I would prefer 10 over 15 regardless of modality except perhaps central lung that wouldnt be a proton case anyways
SBRT protons gets SBRT code, that’s correct advice. Should not get the proton code. On paper they bill about the same per fraction, but of course you have that pesky cap at 5 fractions when it’s SBRT. Another titbit (real word) of info eg, if you did proton SBRT on breast you couldn’t bill any IGRT per fraction. But if you did five fraction high dose proton and billed proton codes AND IGRT, one could argue that’s unbundling.Very hard to make protons "worth it" with 5 fractions. That is why the proton zealots should be most worried about SBRT.
This thread is probably off topic and may deserve a thread on Protons/RBE/fractionation
Agree, thread has gotten sidetracked....but in a very pertinent way.Very hard to make protons "worth it" with 5 fractions. That is why the proton zealots should be most worried about SBRT.
This thread is probably off topic and may deserve a thread on Protons/RBE/fractionation
I think he's conflating high standards with embracing being overworked. If Kobe had hit 60% of his shots he'd be the greatest basketball player ever. If I bricked on 40% of my patients I'd be in a different profession. When I look at my schedule in aria, there is no planning time built in. Kinda like a surgeon having no OR time. It's weird it's like that, and there's a limit to my capacity to think critically. That limit is lower in training.Then, after emphasizing value-based-care for non-hospital based practices, but pocketing sky-high reimbursements yourself, you get to turn around and declare they're in the 'minors' and can't afford all the wonderful new shiny things you can. Regulatory capture everyone!

I could make it happen, but it would be a different clinic. I was just venting a little, I suppose.The importance of having planning time built in the schedule is crucial - but I'm guessing at some places that is a non-starter
Everyone be bashing rural radonc like its a bad thing.
You want a half-time # paying job? Welcome I say, welcome to rural america.


His circles are better then yours.I admit, I'm a tad bored today with my single digit on treatment. But hey, my bank account isn't complaining so I need to remember that I could be instead doing 14 consults and bragging on twitter about how pumped I'm getting lol.
His circles are better then yours.
My circles are perfect… nobody has ever seen a more gorgeous creation!If you zoom in far enough, all of our circles are squares
Building in contouring/dosimetry time was one of the smartest things I've ever seen in scheduling. 30 minutes of protected time in dosimetry in the AM and PM will ensure all contours are done within 24 hours and potentially shave a week off of planning. It shortens the iterative loop from once every couple days to twice a day. Also prevents your dosimetrists from getting bored waiting for contours then having to work feverishly later once you drop them in a big batch. Expecting people to do contours and check all their portal images at home or afterhours is unrealistic unless they own the practice.I think he's conflating high standards with embracing being overworked. If Kobe had hit 60% of his shots he'd be the greatest basketball player ever. If I bricked on 40% of my patients I'd be in a different profession. When I look at my schedule in aria, there is no planning time built in. Kinda like a surgeon having no OR time. It's weird it's like that, and there's a limit to my capacity to think critically. That limit is lower in trainin
Radiation oncology, folks, let me tell you, it's a real head-scratcher. You've got these doctors, very smart people, they say it's the way to go for treating cancer. But, folks, I've got my doubts, and I'm not one to shy away from sharing my thoughts."Write a short speech about drawing perfect circles in the style of Donald (Shytbag) Trump"
ChatGPT: Hold my beer
ChatGPT been reading(!)Radiation oncology, folks, let me tell you, it's a real head-scratcher. You've got these doctors, very smart people, they say it's the way to go for treating cancer. But, folks, I've got my doubts, and I'm not one to shy away from sharing my thoughts.
First off, radiation, you know what that means, right? It's like something out of a sci-fi movie, and I've been in a few of those, let me tell you. But this isn't a movie, this is real life, and we're talking about blasting people with radiation. Sounds a bit extreme, doesn't it?
Now, they say it's effective, they say it can shrink tumors and all that. But let me tell you something, there are side effects, big side effects. It can damage healthy cells too, not just the bad ones. So, you're trying to cure cancer, and in the process, you might be causing more problems. That doesn't sound like a good deal to me.
And let's not forget the cost, folks. It's astronomical, it really is. I've always been a businessman, I know the value of a dollar, and we can't afford to be throwing money at treatments that might not even work. We should be looking for cost-effective solutions, not breaking the bank.
But here's the thing, folks, there are alternatives out there. We've got cutting-edge research, promising new therapies, and we should be putting our money into those areas. We've got to be smart about this, and radiation oncology, well, it's just not the smartest choice, believe me.
In conclusion, radiation oncology, it's got its proponents, but I'm not convinced. It's expensive, it's risky, and there are better options on the table. We need to prioritize effective and affordable treatments for cancer, and radiation therapy might not be the golden ticket everyone thinks it is. We can do better, folks, we can do better.
