You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
Seminoma RT
Personally it’s been about 8 years. Treating seminoma is a lost art and dying subfield. Look for my letter to the editor in the Red Journal next month - I’m starting a local initiative (Bay Area League to restore the Lost art of Seminoma radiation).
I am going to propose that seninomas be immediately referred to our local academic centers for same day treatment. Furthermore, given how few seminomas are seen by residents in training nowadays, I suggest we create a fellowship and a separate ABR specialization.
I am going to propose that seninomas be immediately referred to our local academic centers for same day treatment. Furthermore, given how few seminomas are seen by residents in training nowadays, I suggest we create a fellowship and a separate ABR specialization.
Last edited:
Under treatment now:
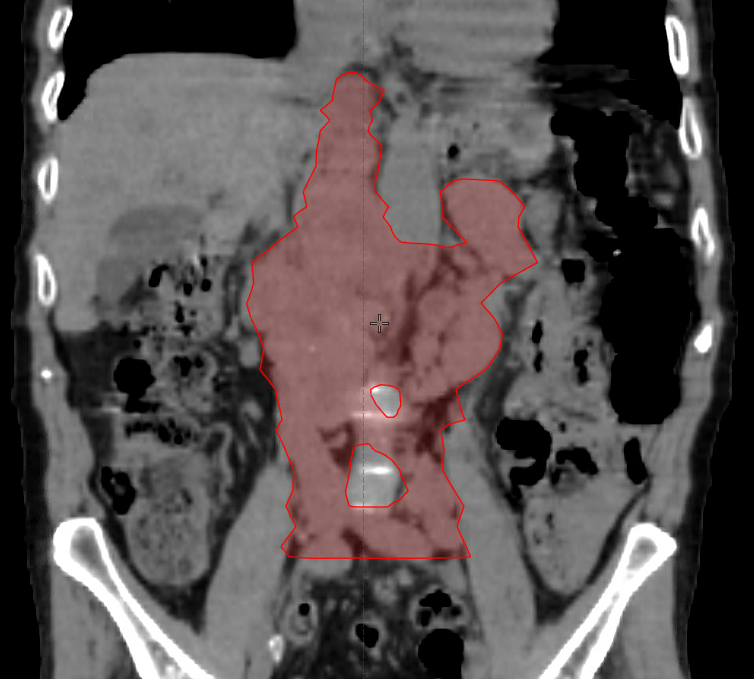
Not exactly adjuvant, but it is after other stuff.
Not exactly adjuvant, but it is after other stuff.
Advertisement - Members don't see this ad
Tough to tell what's adenopathy/bowel/vessel from one slice, but it looks like what I presume is a right common iliac node is getting short changed.
It's vessel. There's upstream venous congestion. Adenopathy is 7 cm AP/PA direction. There are some smaller nodes further south along the let iliac, but I had to stop somewhere. Resimming tomorrow after 12 Gy given shrinkage.Tough to tell what's adenopathy/bowel/vessel from one slice, but it looks like what I presume is a right common iliac node is getting short changed.
Last edited:
About three years ago.
Patient had a T1N0 tumor. On observation had early para aortic failure. Elected for XRT instead of chemo for what was then IIA disease. NED since.
Patient had a T1N0 tumor. On observation had early para aortic failure. Elected for XRT instead of chemo for what was then IIA disease. NED since.
Thanks, Obama!To get an adjuvant, you'll have to more than likely have interested referrers for such on the urology and med onc side. Those interested referrers have not referred to me since the Obama administration.
I'm on track to have never seen it in residency.
I'll tell you what though, I certainly have sat through about 7 lectures and answered dozens of boards-related practice questions on the topic. I feel like I've seen one, does that count?
I'll tell you what though, I certainly have sat through about 7 lectures and answered dozens of boards-related practice questions on the topic. I feel like I've seen one, does that count?
Advertisement - Members don't see this ad
Active Surveillance is the treatment of choice for a stage I seminoma patient. The last time I did radiotherapy for stage I was 10 years ago. I treat stage IIA/B once every year approximately. Ten years ago, AS was not the preferred option for stage I according to national guidelines.
There is one scenario where one could think of adjuvant treatment with radiotherapy for stage I seminoma: patients who will not tolerate chemotherapy well in case of relapse. If you have for instance a patient with considerable heart or lung disease or perhaps a weird hematologic condition which makes them not (well) eligible for chemotherapy, you may opt for adjuvant radiotherapy to eliminate the "risk" of having to give 3x BEP or 4x EP down the road.
I would certainly weigh in risk factors for recurrence of course when making that call.
There is one scenario where one could think of adjuvant treatment with radiotherapy for stage I seminoma: patients who will not tolerate chemotherapy well in case of relapse. If you have for instance a patient with considerable heart or lung disease or perhaps a weird hematologic condition which makes them not (well) eligible for chemotherapy, you may opt for adjuvant radiotherapy to eliminate the "risk" of having to give 3x BEP or 4x EP down the road.
I would certainly weigh in risk factors for recurrence of course when making that call.
"He who studies medicine without books sails an uncharted sea, but he who studies medicine without patients does not go to sea at all."I'm on track to have never seen it in residency.
I'll tell you what though, I certainly have sat through about 7 lectures and answered dozens of boards-related practice questions on the topic. I feel like I've seen one, does that count?
- William Osler
Lots of landlocked rad onc residents these days #sadfaceemoji
"Halstead! For the love of God, step away from the cocaine!""He who studies medicine without books sails an uncharted sea, but he who studies medicine without patients does not go to sea at all."
- William Osler
Lots of landlocked rad onc residents these days #sadfaceemoji
- also Osler
Been at least 5 years since treated seminoma and 3 for Hodgkin.
About a decade for Stage I but I have treated 3 early PA recurrences with RT alone in the last five years. I am thinking of offering a seminoma fellowship.
Let's not get crazy. Fellowships here would be silly and offensive. Practices and centers should simply credential rad oncs for seminoma treatment (AP/PA techniques and volumes are complex) via a thorough vetting process and that should suffice.About a decade for Stage I but I have treated 3 early PA recurrences with RT alone in the last five years. I am thinking of offering a seminoma fellowship.
Sounds like a high volume center of excellence.About a decade for Stage I but I have treated 3 early PA recurrences with RT alone in the last five years. I am thinking of offering a seminoma fellowship.
About a year ago. I try to avoid it when I can and the last couple I have done were all for the same reason: recent diagnosis preparing to deploy for active duty and unable to keep up with surveillance opting to treat before leaving. I also treated someone getting ready to serve an extended prison sentence who didn’t trust the government to take care of him. Otherwise I only treat for salvage and honestly that’s how it should be. These are super salvageable.When was the last time you treated a seminoma in the adjuvant setting?
That was my whole point. I am preparing for my clinical exam and learning the ‘dead art’ from the books and questions.I'm on track to have never seen it in residency.
I'll tell you what though, I certainly have sat through about 7 lectures and answered dozens of boards-related practice questions on the topic. I feel like I've seen one, does that count?
Advertisement - Members don't see this ad
That was my whole point. I am preparing for my clinical exam and learning the ‘dead art’ from the books and questions.
Not entirely. Adjuvant for stage 1 may be dead but it’s conceivable you could treat a stage 2 patient. The only difference is you boost the involved node to 30 Gy. These are a chip shot if you get them on your boards. It will go something like this: they have you stage it as stage 1. They ask you options expecting you to recommend surveillance. Then they tell you the patient is anxious and wants treatment. You tell them the can do carbo or RT and the patient will take RT. Then you have to tell them the dose (20 Gy) and describe the field (AP/PA). Use a clamshell. Boom, you passed.
NCCN mentions 36 Gy for larger lymph node...Not entirely. Adjuvant for stage 1 may be dead but it’s conceivable you could treat a stage 2 patient. The only difference is you boost the involved node to 30 Gy. These are a chip shot if you get them on your boards. It will go something like this: they have you stage it as stage 1. They ask you options expecting you to recommend surveillance. Then they tell you the patient is anxious and wants treatment. You tell them the can do carbo or RT and the patient will take RT. Then you have to tell them the dose (20 Gy) and describe the field (AP/PA). Use a clamshell. Boom, you passed.
Adjuvantly? Haven't done a single one. Did one salvage during residency.
Similar threads
- Replies
- 20
- Views
- 3K

