Advertisement - Members don't see this ad
You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
The March Continues for Prostate Hypofractionation
Started by Chartreuse Wombat
D
deleted941485
Where have you been? Hypofrac and Sbrt are the future. There’s no turning back from this stuff. Gonna work its way into literally every disease site they can get enough data for. Only hope is APMs that way we can hypofrac the living daylights out of everything we can get away with. Until then You just need to hope your employer doesn’t fire you when your Dept’s revenue drops off a cliff. But hey we’re in such high demand these days...right? We’ll land on our collective feet...
Just a thought experiment. Twelve years ago, what percent of fractions delivered in the average department were for localized prostate cancer? Breast cancer? Metastatic disease?
Now imagine prostate treatment numbers drops by ~80%.
And fractions for breast cancer drop by ~50%
And if we’re “choosing wisely”, metastatic treatment fraction volume decreases by 75%.
Let me be transparent: this is great news for patients! We should celebrate these advances. But as we cheer these developments, we should also be able to sincerely ask ourselves (and our “leadership”), do we need 50% more docs to each year to deliver an ever decreasing number is fractions?
The medical students of the Class of 2019 were smart enough to do the arithmetic. Will our illustrious chairs follow?
I doubt it.
Now imagine prostate treatment numbers drops by ~80%.
And fractions for breast cancer drop by ~50%
And if we’re “choosing wisely”, metastatic treatment fraction volume decreases by 75%.
Let me be transparent: this is great news for patients! We should celebrate these advances. But as we cheer these developments, we should also be able to sincerely ask ourselves (and our “leadership”), do we need 50% more docs to each year to deliver an ever decreasing number is fractions?
The medical students of the Class of 2019 were smart enough to do the arithmetic. Will our illustrious chairs follow?
I doubt it.
Advertisement - Members don't see this ad
Maybe a naive question, but might SBRT result in higher proportion of patients selecting radiation therapy over RP, with this at least partially offsetting the decrease in # of fractions?
A smaller pool of patients compared to a decade ago or longer, given the higher number of pts choosing active surveillance, coupled with PCPs performing less PSA screening after the USPTF recs against it several years ago (although this did change very recently).Maybe a naive question, but might SBRT result in higher proportion of patients selecting radiation therapy over RP, with this at least partially offsetting the decrease in # of fractions?
This is good for patients, not for increasing RO demand though. Urology has been undersupplied in the market for years, so it really doesn't impact them as much
in my experience, if you're comfortable offering SBRT, it's the easiest sell of all for patients debating surgery vs RT. it's a slam dunk.
In my practice, over 50% of my patients are hypofractionationed in some way, either SRS, 1-5 fraction SBRT/FSRT, or 1-5 fraction palliative cases. I never have more than 15 on beam, and my RVUs are solid for academics. This is the future.
I have been here all along. My default regimen brachy for appropriate patients; otherwise 60/20 or for selected patients SBRT.Where have you been? Hypofrac and Sbrt are the future. There’s no turning back from this stuff. Gonna work its way into literally every disease site they can get enough data for. Only hope is APMs that way we can hypofrac the living daylights out of everything we can get away with. Until then You just need to hope your employer doesn’t fire you when your Dept’s revenue drops off a cliff. But hey we’re in such high demand these days...right? We’ll land on our collective feet...
Agree with what has been said above. SBRT makes for a good selling point among patients who are comparing surgery and radiation. I hope that the evidence continues to mature and support it's use, especially as an alternative to HDR. The knowledge and technical barrier to offering good SBRT is much lower than for good implants. I think this is a great advancement for our field, while recognizing that it won't necessarily help the bottom line.
Maybe a naive question, but might SBRT result in higher proportion of patients selecting radiation therapy over RP, with this at least partially offsetting the decrease in # of fractions?
It can. As GFunk has said numerous times before, there are those who fight change, and those who learn to use it. In my part of the country we did very little definitive radiation for prostate. Now we do.
At the same time, in places without aggressive urologists, conventional prostate RT may be a significant proportion of some practices volume. It’s hard to judge someone for having a hard time seeing this as a good thing.
In my practice, over 50% of my patients are hypofractionationed in some way, either SRS, 1-5 fraction SBRT/FSRT, or 1-5 fraction palliative cases. I never have more than 15 on beam, and my RVUs are solid for academics. This is the future.
Ditto. I’m 50% clinical and ride around 15-20 under treatment. About half are some kind of SBRT (mostly liver) or hypofractionation. If the community docs in my state embraced new practices, my numbers would not be so high.
Advertisement - Members don't see this ad
Maybe a naive question, but might SBRT result in higher proportion of patients selecting radiation therapy over RP, with this at least partially offsetting the decrease in # of fractions?
I doubt that SBRT will suddenly lead to a lot more men choosing radiation over RALP. In many parts of the country, men with prostate cancer never even have a consultation with a RO. Urologists own the patients and they can be quite effective at scaring patients away from the "harms" of radiation.
I doubt that SBRT will suddenly lead to a lot more men choosing radiation over RALP. In many parts of the country, men with prostate cancer never even have a consultation with a RO. Urologists own the patients and they can be quite effective at scaring patients away from the "harms" of radiation.
I agree that this is an issue for many practices, no doubt. But as sbrt becomes more widely adopted and becomes commonly known, it’s going to be harder for urologists to downsell it. Kind of a long game win.
Also you’re still seeing some patients wirh intact prostate I’m sure - are these JUST patients that aren’t medically operable?
Last edited:
Many of the aggressive/unscrupulous urologists are going to jump on HIFU, whole gland or focal, to avoid sending nonsurgical pts for XRT, just like many have and, in some cases, continue to do cryosurgery inappropriately for upfront therapyI agree that this is an issue for many practices, no doubt. But as sbrt becomes more widely adopted and becomes commonly known, it’s going to be harder for urologists to downsell it. Kind of a long game win.
Also you’re still seeing some patients wirh intact prostate I’m sure - are these JUST patients that aren’t medically operable?
Last edited:
Let's review the current trends in prostate cancer:
-Only about ~60% of patients with PCa consult with a RO; link
-Use of AS is on the rise with concomitant decline in XRT; link
-PSA screening is decreasing among PCPs; link
-SBRT reimbursement is about half of IMRT; link
-We are moving from 45 fractions to 5; see OP
So if you think SBRT will be a big windfall for the specialty, then you are wrong.
-Only about ~60% of patients with PCa consult with a RO; link
-Use of AS is on the rise with concomitant decline in XRT; link
-PSA screening is decreasing among PCPs; link
-SBRT reimbursement is about half of IMRT; link
-We are moving from 45 fractions to 5; see OP
So if you think SBRT will be a big windfall for the specialty, then you are wrong.
Don't think anyone is saying it's a 'windfall', but not necessarily the end of the world either, if that's what you think.
we're just in the middle of a transition period from the 'old guard thought' based on rudimentary understanding of rad bio that dictated that everything needed to be done at 1.8 or 2 Gy/fx. Also technocolgy has changed so we CAN do more.
Things change, thankfully.
I think everyone is in agreement (before you mention it) that we should put the brakes on resident training expansion for a while.
we're just in the middle of a transition period from the 'old guard thought' based on rudimentary understanding of rad bio that dictated that everything needed to be done at 1.8 or 2 Gy/fx. Also technocolgy has changed so we CAN do more.
Things change, thankfully.
I think everyone is in agreement (before you mention it) that we should put the brakes on resident training expansion for a while.
Must be a real long game kid. As I was eating caviar last night I noticed this ad was in my "The New Yorker." I have seen roadside billboards in Florida advertising the same "breakthroughs" for twenty years. Know what that's got us? Bupkis! Once I figure out how to diagnose prostate cancer all on my wonderful own, I can control the patient. That's why I'm advocating that we become interventional radiologists AND rad oncs, you see...I agree that this is an issue for many practices, no doubt. But as sbrt becomes more widely adopted and becomes commonly known, it’s going to be harder for urologists to downsell it. Kind of a long game win.
Also you’re still seeing some patients wirh intact prostate I’m sure - are these JUST patients that aren’t medically operable?

Goo goo g'joob
I would humbly submit that the problem is the *****ic way institutions/people are reimbursed per fraction instead of per course. Once this is taken into proper perspective, there will be no impediment to hypofractionate everything and suddenly people will have an "awakening."
Can anyone honestly tell me why a 41 fraction prostate cancer VMAT course should reimburse more than a 10-20 fraction lymphoma VMAT case? The stakes are way higher with the latter, not to mention the risk of secondary malignancy which is germane in 30-40 year old patients and not in 70-80 year old low-risk prostate patients.
Can anyone honestly tell me why a 41 fraction prostate cancer VMAT course should reimburse more than a 10-20 fraction lymphoma VMAT case? The stakes are way higher with the latter, not to mention the risk of secondary malignancy which is germane in 30-40 year old patients and not in 70-80 year old low-risk prostate patients.
ASTRO, at one point a few years ago, looked into trying to have CMS split imrt into simple (prostate) and (complex). It's crazy to me that a prostate only ebrt plan reimburses the same planning charge as a head and neck or pelvic imrt planI would humbly submit that the problem is the *****ic way institutions/people are reimbursed per fraction instead of per course. Once this is taken into proper perspective, there will be no impediment to hypofractionate everything and suddenly people will have an "awakening."
Can anyone honestly tell me why a 41 fraction prostate cancer VMAT course should reimburse more than a 10-20 fraction lymphoma VMAT case? The stakes are way higher with the latter, not to mention the risk of secondary malignancy which is germane in 30-40 year old patients and not in 70-80 year old low-risk prostate patients.
I would humbly submit that the problem is the *****ic way institutions/people are reimbursed per fraction instead of per course. Once this is taken into proper perspective, there will be no impediment to hypofractionate everything and suddenly people will have an "awakening."
Can anyone honestly tell me why a 41 fraction prostate cancer VMAT course should reimburse more than a 10-20 fraction lymphoma VMAT case? The stakes are way higher with the latter, not to mention the risk of secondary malignancy which is germane in 30-40 year old patients and not in 70-80 year old low-risk prostate patients.
Although the argument of "reimbursing per course and not per fraction" makes sense, I do not think it's the ultimate way to go.
The problem with reimbursing per course is that it may lead to overutilization of expensive techniques where there is little to gain.
What does this mean?
Reimbursing per course and not per fraction will for example lead to radical cuts to those who still opt for 35/2.5 or 40/2 for bone mets nowadays.
Standard bone metastasis treatment will cost significantly less, probably in the range of what is now being paid for 20/4?
These guys will have to rethink their practice and may opt to SBRT every bone met so that they can still make some money. Don't get me wrong, SBRT may be great for many cases of bone mets but it probably isn't the solution for every patient with a bone or let me formulate it better: "Not every patient will benefit from it."
Thus, in my view, one needs to find a middle way out of this.
Perhaps in the case of bone mets:
Reimburse a flat fee for planning and the first 5 fractions. Every additional fraction will also be reimbursed but with a significantly lower amount per fraction as of what is being reimbursed today. That way you are discouraging physicians from "overfractionating".
Reimburse VMAT or SBRT only if certain parameters are met (good PS, favorable prognosis, pretreatment).
We do this in Europe to some extent too.
Where I practice: When utilizing stereotactic fractionated radiotherapy, we get paid significantly more for the planning process and for the first 6 fractions. Every further stereotactic fraction beyond those 6 is reimbursed like a "normal" 3D-fraction.
Perhaps in the case of bone mets:
Reimburse a flat fee for planning and the first 5 fractions. Every additional fraction will also be reimbursed but with a significantly lower amount per fraction as of what is being reimbursed today. That way you are discouraging physicians from "overfractionating".
Reimburse VMAT or SBRT only if certain parameters are met (good PS, favorable prognosis, pretreatment).
This is what we do already in the USA.
There are guidelines for IMRT or SBRT put out by CMS (Medicare) and private insurers that use such parameters.
I'm not entirely clear how much of the payment is per fraction vs. the upfront costs (planning, simulation, etc) for treatment of a 3D bone met case. Does anyone know the cost difference for a 5 or 10 fraction course vs. a 20 fraction course? The difference between 10 and 20 fractions is certainly not double.
Advertisement - Members don't see this ad
RANDO_Phantom
Full Member
I doubt that SBRT will suddenly lead to a lot more men choosing radiation over RALP. In many parts of the country, men with prostate cancer never even have a consultation with a RO. Urologists own the patients and they can be quite effective at scaring patients away from the "harms" of radiation.
Aggressive group of urologists in my area -- all young, <10 years out from training, and operate on everyone. No qualms about saying "patient refused radiation" in Tumor Board discussions. THEY'RE the ones talking to patients about radiation, and in vast majority of cases, deter them from it. I'll never get used to it, this idea that no patients are truly "our" patients, that we just get to borrow them a few weeks. Uros get away with it all the time, at least where I am. It devalues our expertise and training, and gyps the patient of an opportunity to hear expert opinion about all of their options, and then making an informed decision that's best for them. I'm trying to get the PCPs to refer every patient with prostate cancer to both urologist and radonc, but it's in one ear/out the other.
At least the younger ones operate. The old timers will cryoablate whole gland or "focal", while some of them would even fly cash patients out to the islands or Mexico for HIFUAggressive group of urologists in my area -- all young, <10 years out from training, and operate on everyone. No qualms about saying "patient refused radiation" in Tumor Board discussions. THEY'RE the ones talking to patients about radiation, and in vast majority of cases, deter them from it. I'll never get used to it, this idea that no patients are truly "our" patients, that we just get to borrow them a few weeks. Uros get away with it all the time, at least where I am. It devalues our expertise and training, and gyps the patient of an opportunity to hear expert opinion about all of their options, and then making an informed decision that's best for them. I'm trying to get the PCPs to refer every patient with prostate cancer to both urologist and radonc, but it's in one ear/out the other.
Speaking of prostate hypofractionation... I was reading the "ASTRO, ASCO, and AUA Evidence-Based Guideline"
https://ascopubs.org/doi/full/10.1200/JCO.18.01097
Can someone tell me how this works?
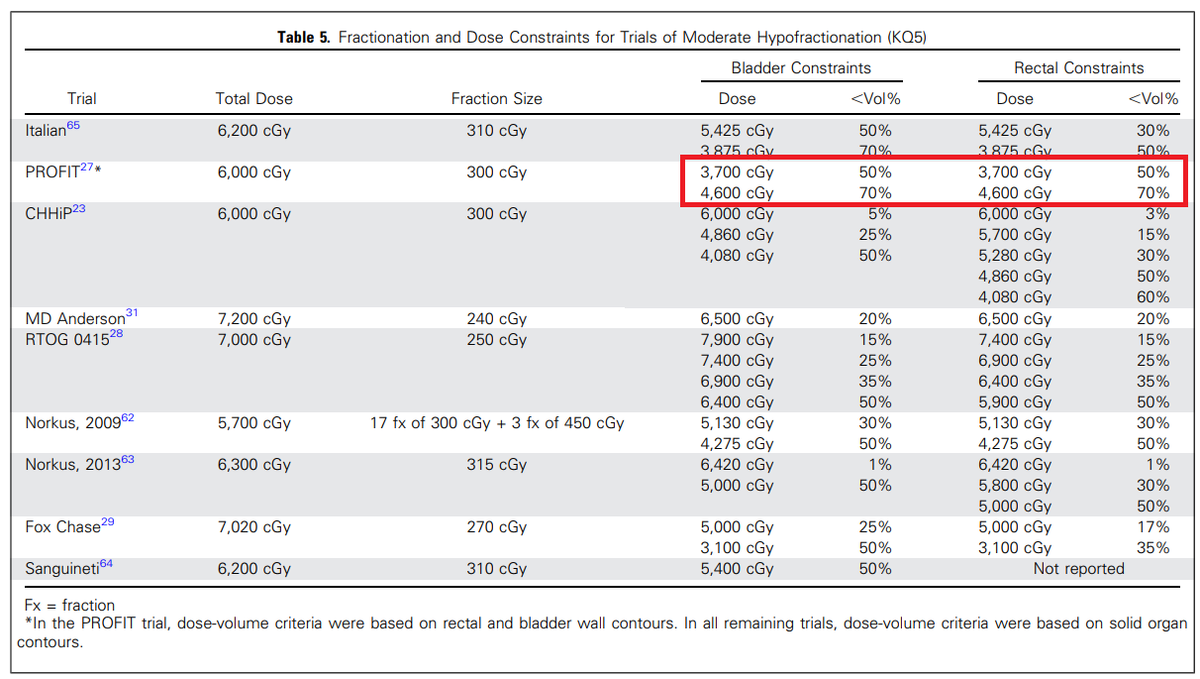
I was under the impression that with rising dose less % of the OAR should receive that dose...
🙂
First I thought it was a typo in the JCO paper. But it seems the trial protocol was actually written that way...
https://ascopubs.org/doi/suppl/10.1200/JCO.2016.71.7397/suppl_file/protocol_2016.717397.pdf
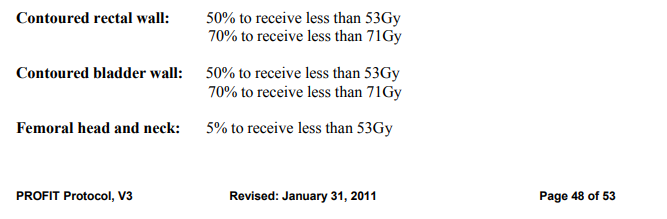
https://ascopubs.org/doi/full/10.1200/JCO.18.01097
Can someone tell me how this works?
I was under the impression that with rising dose less % of the OAR should receive that dose...
🙂
First I thought it was a typo in the JCO paper. But it seems the trial protocol was actually written that way...
https://ascopubs.org/doi/suppl/10.1200/JCO.2016.71.7397/suppl_file/protocol_2016.717397.pdf
Last edited:
Is that not 77385 and 77386.ASTRO, at one point a few years ago, looked into trying to have CMS split imrt into simple (prostate) and (complex).
A 3D course of tx at 35 fractions is about $14,000. So let's assume a complex tx (custom blocking, tangents, wedges, etc., ie 3D). If each "3D fraction" goes for about $275, then ROUGHLY....Does anyone know the cost difference for a 5 or 10 fraction course vs. a 20 fraction course? The difference between 10 and 20 fractions is certainly not double.
5 fractions: $5750
10 fractions: $7125 (~25% more than 5 fx)
20 fractions: $9875 (~40% more than 10 fx)
That's global reimbursement. Out of $14K for 35fx sans IGRT, about $2500 is professional. Past about 10 fractions, reimbursement more or less does double on the professional side especially once you add in IGRT.
One would assume keep 70% or more of rectum ("<Vol%") to 46Gy or less e.g. One would assume. What's dumb about constraints is that both of these DVHs below meet the rectal constraints. (They did add in a 50% 37 Gy constraint, even so...) But which curve would you want???Speaking of prostate hypofractionation... I was reading the "ASTRO, ASCO, and AUA Evidence-Based Guideline"
https://ascopubs.org/doi/full/10.1200/JCO.18.01097
Can someone tell me how this works?
View attachment 257294
I was under the impression that with rising dose less % of the OAR should receive that dose...
🙂

Last edited:
I was referring to 77301. Tx planning, not delivery. I think ASTRO was trying to target urorads with that oneIs that not 77385 and 77386.
I once heard Nancy Lee say it took her a few hours to do an NPC case. Whew! Maybe we should do like lawyers and charge patients for billable hours spent contouring/planning. That'd be the most honest way... if everyone was honest. The way human nature is, we would probably see a study on improved clinical outcomes with time spent contouring. Still, some rad oncs are fast and some slow in various clinical scenarios; it can take me longer on a prostate than a H&N sometimes. Regardless, I like to be speedy. I like to approach planning and contouring like the surgeons of old, "Time me, gentlemen."I was referring to 77301. Tx planning, not delivery. I think ASTRO was trying to target urorads with that one
I would humbly submit that the problem is the *****ic way institutions/people are reimbursed per fraction instead of per course. Once this is taken into proper perspective, there will be no impediment to hypofractionate everything and suddenly people will have an "awakening."
Can anyone honestly tell me why a 41 fraction prostate cancer VMAT course should reimburse more than a 10-20 fraction lymphoma VMAT case? The stakes are way higher with the latter, not to mention the risk of secondary malignancy which is germane in 30-40 year old patients and not in 70-80 year old low-risk prostate patients.
I am totally onboard with hypofractionation. In fact, despite being in private practice, we hypofractionate fairly aggressively (to the point that our numbers are probably 25% less than they could be).
This is high value care. If you believe that the control rates and toxicity are similar, this is objectively what is best for our patients. The problem with hypofractionation is that private practice radiation oncologists are penalized for doing what is best for their patients. In fact, I would go so far as to say that a practice that hypofractionates is LESS competitive than one that doesn't, for the simple fact that you are making less money and thus are less able to compete. Like it or not though, hypofractionation is here to stay. As I have said before, the hypofractionation vs. standard fractionation non-inferiority study has become the bread and butter of academic radiation oncology and does more to advance careers than it does to advance our field.
Since we anonymous misanthropes of SDN love to complain about ASTRO leadership, my main criticism of the push to embrace hypofractionation is as follows. Radiation oncologists are being shamed into making what is probably an equivalent treatment the new standard of care. This is what is probably best for patients, but it is definitely not best for us as physicians (selfish, I know). However, rather than being proactive about things and pushing a model that rewards physicians for providing value prior to making the recommendation that everyone takes a pay cut, our leadership has once again let the cart come before the horse and created a situation where the interests of its constituents are simply ignored or it is assumed that they will work themselves out (market correction, canaries in coal mines, etc).
The massive irony of all this is that the people pushing for all of this "high value care" are the same people investing millions of dollars in protons with absolutely no randomized clinical data to back this up, the very definition of low value care. Not to spout conspiracy theories, but one has to wonder what the spin will be on the COMPPARE study. Unfortunately, the people that control these studies also control the flow of information and have a vested interest in the outcome.
"Hypofractionation is non-inferior to standard fractionation and thus should be the new standard of care"
"Proton therapy is non-inferior to photon therapy and thus should be the new standard of care"
Protons were supposed to be better, given the significant cost differential, while hypofx costs the system less."Hypofractionation is non-inferior to standard fractionation and thus should be the new standard of care"
"Proton therapy is non-inferior to photon therapy and thus should be the new standard of care"
I cant imagine they are shameless enough to say that about protons and was pleasantly surprised to see the oped in JCO trashing protons for lung ca (and rightfully so)
I cant imagine they are shameless enough to say that about protons and was pleasantly surprised to see the oped in JCO trashing protons for lung ca (and rightfully so)
This was admittedly overly facetious and conspiracy theorist on my part.
Advertisement - Members don't see this ad
So you agree with me that their constraints make no sense whatsoever?One would assume keep 70% or more of rectum ("<Vol%") to 46Gy or less e.g. One would assume. What's dumb about constraints is that both of these DVHs below meet the rectal constraints. (They did add in a 50% 37 Gy constraint, even so...) But which curve would you want???

It's interesting to see that they were not changed in this huge trial over the years and various protocol versions...
Would the following sound better?Speaking of prostate hypofractionation... I was reading the "ASTRO, ASCO, and AUA Evidence-Based Guideline"
https://ascopubs.org/doi/full/10.1200/JCO.18.01097
Can someone tell me how this works?
View attachment 257294
I was under the impression that with rising dose less % of the OAR should receive that dose...
🙂
First I thought it was a typo in the JCO paper. But it seems the trial protocol was actually written that way...
https://ascopubs.org/doi/suppl/10.1200/JCO.2016.71.7397/suppl_file/protocol_2016.717397.pdf
View attachment 257295
71 Gy to no more than 30%
53 Gy to no more than 50%
Both are saying the same thing. (I think; but I am sure that the misanthropes and deplorable of SDN will correct me)
The popular constraint of 70 Gy <25% of rectum is the same as 75% of rectum to receive less than 70 Gy; right?
Last edited:
Would the following sound better?
71 Gy to no more than 30%
53 Gy to no more than 50%
Both are saying the same thing. (I think; but I sure that the misanthropes and deplorable of SDN will correct me)
The popular constraint of 70 Gy <25% of rectum is the same as 75% of rectum to receive less than 71 Gy; right?
I see how you're reading it. The original way that Chip and Profit did it seems like a ****ty way to report constraints, and flies in the face of how DVH constraints are normally reported for percentage based values. But I do see how it ends up being the same.
This horrible rectal DVH curve meets those reasonable sounding criteria.Would the following sound better?
71 Gy to no more than 30%
53 Gy to no more than 50%

Yes, but you know that a competent radiation oncologist would not sign that plan because while meeting the constraints a competent radiation oncologist would know that it is possible to derive a better solution.
Yes, but you know that a competent radiation oncologist would not sign that plan because while meeting the constraints a competent radiation oncologist would know that it is possible to derive a better solution.
exactly.
what a ridiculous hypothetical proposed by scarbrtj. By that metric, tons and tons of Bad DVHs could be written out for almost any constraint.
I have seen many situations where people "met literature constraints" yet generated DVHs which could have been easily improved. While we don't write out DVHs per se, we birth DVHs with constraints as starting points. Looking at the prostate literature and the table Palex80 posted above, I have made better DVHs in 100% of cases than what the literature constraints allow. 100%. Which means the literature constraints allow for DVHs (and clinical outcomes probably) which are worse than achievable. That ain't good. The (prostate rectal) constraints are superfluous paper tigers. There have been attempts to create different ways of conveying constraints versus one or two thou-shall-not-pass points on a DVH; they've not gained traction. Although it matters how close a DVH constraint point is to the Rx dose. Again in the table above where all doses are prescribed at about 60-70 Gy, I don't see a point constraint at ~33% of the Rx dose, ie at 20 Gy. In stage III lung planning where have Rx doses to 60+ Gy, we care a lot about a DVH point at 20 Gy to a particular OAR. That makes optimization harder, which is good. If DVH point constraints are set closer to the Rx dose for an OAR, it makes optimization easier, which is bad. All the rectal constraints above, save Fox Chase's (who have constraint points farthest from the Rx dose... they have a point at ~42% of Rx dose), allow for rectal doses which I never have/never will countenance and set up for IMRT optimizations with little-to-no cost, mathematically speaking.By that metric, tons and tons of Bad DVHs could be written out for almost any constraint.
This horrible rectal DVH curve meets those reasonable sounding criteria.

But Chartreuse's point was that the SAME DVH would be deemed 'acceptable' if you said V71 < 30% or V53 < 50%, which are normal sounding constraints for prostate treatment. It's just a difference in terminology.
That DVH is bad regardless of how you frame the constraint.
I agree with you that for clinical trials the constraints are overtly generous. However, for national or international trials they have to make it something people can do regardless of technology, hence why they are so lax. I imagine most of us are not allowing V71 of rectum to routinely be 30% when treating with standard fractionation, but in places without ability to do daily CBCT or fiducials + daily KV pairs, PTV margins may be large (remember that some of these trials even allowed 3D prostate treatment) enough where forcing stricter constraints makes centers unable to enroll patients on the trial (which is bad for the trial).
Also, sometimes people do things differently in clinical practice than they do for the trial. For example, NSABP-B51 mandates PTV margins (I believe 5mm) for all the lymph node basins and evaluation of coverage based on that. How many of us are routinely putting PTV margins on all of our contoured lymph node regions (EDIT - in breast cancer patients) and evaluating plans/DVHs based on that? Maybe I'm an outlier but I don't do that in routine clinical practice.
Last edited:
The point I was trying to make is that those DVH constraints make no sense... Irrelevant if you look at the JCO paper or the protocol, they make no sense.
If you demand that less than 50% of the rectal wall should receive 37 Gy, what's the point in saying that less than 70% of the rectal wall should receive 46 Gy?
In other words the constraints say:
V37 < 50% and V46 < 70%
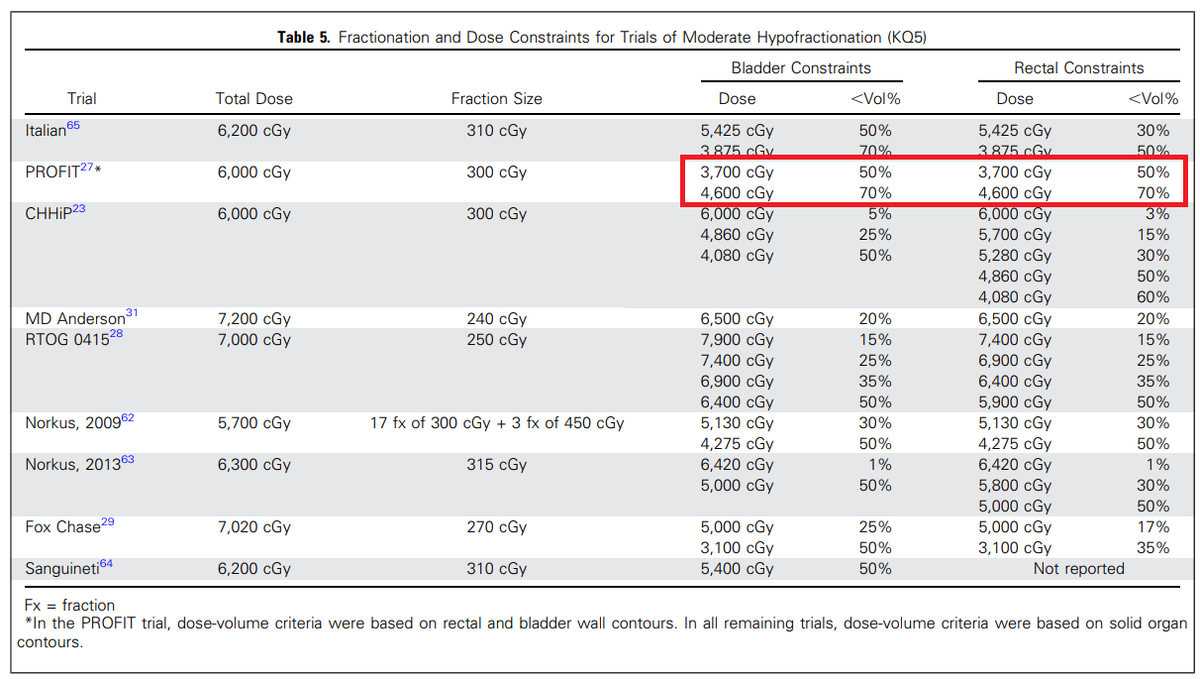
That makes no sense.
The DVH would have to climb rather than fall to meet that constraint.
If you demand that less than 50% of the rectal wall should receive 37 Gy, what's the point in saying that less than 70% of the rectal wall should receive 46 Gy?
In other words the constraints say:
V37 < 50% and V46 < 70%
That makes no sense.
The DVH would have to climb rather than fall to meet that constraint.
The point I was trying to make is that those DVH constraints make no sense... Irrelevant if you look at the JCO paper or the protocol, they make no sense.
If you demand that less than 50% of the rectal wall should receive 37 Gy, what's the point in saying that less than 70% of the rectal wall should receive 46 Gy?
In other words the constraints say:
V37 < 50% and V46 < 70%
View attachment 257454
That makes no sense.
The DVH would have to climb rather than fall to meet that constraint.
Chartreuse's point is that it's actually NOT saying V37 < 50% and V46 < 70%.
That is how I initially read it as well, but it's likely a misquoting of the PROFIT protocol (based on the picture you had earlier of how they phrase their constraints).
The proper way I would phrase that constraint would essentially be V37 < (100-50%) = V37 < 50% and V46 < (100-70%) = V46 < 30%, which is more in line with what CHHiP has.
And don't even get me started on the RTOG 0415 constraints, which I've tried to use previously when treating with 70/28. Prescription dose is 70Gy and your Rectal constraint is V74 < 15%? Such lazy trial and constraint writing to literally just copy and paste from the standard fractionation arm without thought on what an appropriate constraint would be.
Is anyone aware of any published, reasonable constraints for 70/28 (as my institutions most common prostate hypofrac regimens) ? Ideally ones that have some actual dose-respondent toxicity outcomes correlated to them?
Advertisement - Members don't see this ad
I do on all my pelvic and h&n imrt pts.... 0.5-0.7 cm. How many of us are routinely putting PTV margins on all of our contoured lymph node regions and evaluating plans/DVHs based on that? Maybe I'm an outlier but I don't do that in routine clinical practice.
I do on all my pelvic and h&n imrt pts.... 0.5-0.7 cm
I meant for breast cancer patients, as NSABP B-51 forces you to to create PTVs for all of your lymph node volumes for plan evaluation. I see this was unclear above and edited that post.
Obviously for any IMRT plan I am creating PTVs (I do IMRT for 100% of H&N and near 100% of non-rectal pelvic).
The constraints on this table don't say anything clinically helpful and are vague and there is no standardized lingo AMAZINGLY (obviously!) in radiation oncology for constraint conveyance without getting wordy and/or using mathematical inequality operators everywhere (e.g. ≤ or ≥). Highly recommend the latter versus the former. All these constraints say is "37 Gy, <Vol% 50%... 46Gy, <Vol% 70." What the heck is "less than volume percent"??? Is one percent "<Vol% 70"? Sure. So 49% of the rectum ("<Vol% 50") could get 37Gy or more, and 1% of the rectum ("<Vol% 70") could get 46Gy or more. Constraint met, DVH falling not rising, nice DVH curve. (69% is also "<Vol% 70," and if you went there, yeah, the DVH would rise not fall.)If you demand that less than 50% of the rectal wall should receive 37 Gy, what's the point in saying that less than 70% of the rectal wall should receive 46 Gy?
In other words the constraints say:
V37 < 50% and V46 < 70%
That makes no sense.
The DVH would have to climb rather than fall to meet that constraint.
On the table, PROFIT is the only case of increasing <Vol% with increasing dose. Others list increasing <Vol% with decreasing dose. You have to get into verbal gymnastics to explain this; for TL;DR purposes I won't. But depending how you read these, you can read it any way you want and you're not easily falsifiable.
Which is, in fact, my ultimate point for "almost any poorly specified constraint."what a ridiculous hypothetical proposed by scarbrtj. By that metric, tons and tons of Bad DVHs could be written out for almost any constraint.
RANDO_Phantom
Full Member
Chartreuse's point is that it's actually NOT saying V37 < 50% and V46 < 70%.
That is how I initially read it as well, but it's likely a misquoting of the PROFIT protocol (based on the picture you had earlier of how they phrase their constraints).
The proper way I would phrase that constraint would essentially be V37 < (100-50%) = V37 < 50% and V46 < (100-70%) = V46 < 30%, which is more in line with what CHHiP has.
And don't even get me started on the RTOG 0415 constraints, which I've tried to use previously when treating with 70/28. Prescription dose is 70Gy and your Rectal constraint is V74 < 15%? Such lazy trial and constraint writing to literally just copy and paste from the standard fractionation arm without thought on what an appropriate constraint would be.
Is anyone aware of any published, reasonable constraints for 70/28 (as my institutions most common prostate hypofrac regimens) ? Ideally ones that have some actual dose-respondent toxicity outcomes correlated to them?
Thanks. Link to article this is from (if possible)? Would like to have a paper to give to attendings/dosimetrists rather than just saying some guy on the internet sent me this.
RANDO_Phantom
Full Member
Thanks. Link to article this is from (if possible)? Would like to have a paper to give to attendings/dosimetrists rather than just saying some guy on the internet sent me this.
Tell 'em Dr. Lee uses these constraints.
This recent red journal article goes over Duke's constraints for their 70/28 regimen. (edit - RANDO beat me to it as above).
Where I trained we also did most patients hypfrac or SBRT and used very similar constraints to the Duke ones. I now do 95% of all my prostate either 70/28 or on NRG GU-05 (SBRT vs. hypofrac). I'm in private practice.
There is some clinical data that suggests V70>10 cc for rectum does correlate best with toxicity, so I try to keep that closer to 5 cc's in most cases.
Where I trained we also did most patients hypfrac or SBRT and used very similar constraints to the Duke ones. I now do 95% of all my prostate either 70/28 or on NRG GU-05 (SBRT vs. hypofrac). I'm in private practice.
There is some clinical data that suggests V70>10 cc for rectum does correlate best with toxicity, so I try to keep that closer to 5 cc's in most cases.
I do. We had that argument before. 🙂Also, sometimes people do things differently in clinical practice than they do for the trial. For example, NSABP-B51 mandates PTV margins (I believe 5mm) for all the lymph node basins and evaluation of coverage based on that. How many of us are routinely putting PTV margins on all of our contoured lymph node regions (EDIT - in breast cancer patients) and evaluating plans/DVHs based on that? Maybe I'm an outlier but I don't do that in routine clinical practice.
Anyone is welcome to try and translate this into practical treatment planning.
https://www.thegreenjournal.com/article/S0167-8140(19)30085-4/fulltext
https://www.thegreenjournal.com/article/S0167-8140(19)30085-4/fulltext
Sorry to hijack this thread somewhat, but does anyone here regularly use one of the moderately hypofx prostate regimens (e.g. 70Gy/20fx)? If so, what dosing do you use for the pelvis or SV. For example, we often take the pelvis to 45Gy or SV to 50.4Gy before boosting the prostate?
Also, what dose constraints do you use for moderate hypofx? RTOG 0415? I know Kaiser will use 10% lower than RTOG 0415 constraints.
Any thoughts?
Also, what dose constraints do you use for moderate hypofx? RTOG 0415? I know Kaiser will use 10% lower than RTOG 0415 constraints.
Any thoughts?
Advertisement - Members don't see this ad
Similar threads
- Replies
- 28
- Views
- 2K
- Replies
- 8
- Views
- 2K
- Replies
- 54
- Views
- 6K
D

