- Joined
- Mar 22, 2008
- Messages
- 4,130
- Reaction score
- 2,742
- Points
- 6,851
- Location
- Phoenix, Arizona
- Attending Physician
Is the Vscan a live demo or online? I did the Butterfly demo and was impressed with the images, but am leaning toward the Vscan due to very positive reviews, no cable, and no ongoing fees.Just did the online demo of butterfly IQ- for the price it kicks the butt out of what I have been borrowing (old mindray) and a very old sonosite. The msk pictures they were showing me live were much better than on their website library.
I would love the edge II, but can't justify the price in my current situation
I have demo of vscan next week and am excited to see what it has to offer.
They mail you one for 3 days and while you have it they schedule a 30min zoom meeting. I am excited to give it a try.Is the Vscan a live demo or online? I did the Butterfly demo and was impressed with the images, but am leaning toward the Vscan due to very positive reviews, no cable, and no ongoing fees.
You mean BCBS denied the ultrasound portion of the injection?I just got us code denial for lateral epicondylitis from bcbs. Biller fought it and we lost appeal.
outside of a heavy regen Med practice I would be hard pressed to justifying paying for more than the butterfly us these days.
I am demo'ing vscan right now. Picture quality is better than I expected. Have not tried injection with yet, so have not visualized needle.Any updates on Butterfly vs Vscan? Very interested in purchasing one of the two
My GE Vscan Air is arriving next Wednesday. I’ll let you know.Bump
Considering getting this. Really like that it has a 2-in-1 probe. Any updated thoughts?
Besides cost, were there any reasons you considered this over the Lumify?My GE Vscan Air is arriving next Wednesday. I’ll let you know.
Just cost. Vs the butterfly, I just liked the wireless. I worry about the probe connection to the device. Also kinda like the curvilinear probe option so maybe I can do ultrasound hip injections.Besides cost, were there any reasons you considered this over the Lumify?
I was ready to pull the trigger but I’m worried about probe longevity




Those seem to be mostly central line associated. Still, do any of you have a good recommendation for sterile probe covers? Hard to sort through what they have on Henry Schein because the filtering on their search sucks, and all the sterile ones seem absurdly expensive.ugh.... dont use a big bottle of US gel...

Ultrasound gel as a source of hospital outbreaks: Indian experience and literature review - PubMed
This report highlights the importance of early identification of an outbreak, prompt response of the ICU and infection control teams, sound environmental and epidemiological surveillance methods to identify the source and stringent infection control measures to control the outbreak. Contaminated...pubmed.ncbi.nlm.nih.gov

Outbreak of Acinetobacter baumannii associated with extrinsic contamination of ultrasound gel in a tertiary centre burn unit - PubMed
Based on data from our epidemiologic, microbiologic, and observational studies, we believe that inadvertent extrinsic contamination of the gel dispenser occurred in the Ultrasound Department. Contaminated gel was then dispensed into multiuse vials of gel stored on the mobile carts. The outbreak...pubmed.ncbi.nlm.nih.gov

Ultrasound echocardiographic gel contamination by Burkholderia cepacia in an Italian hospital - PubMed
Ultrasound echocardiographic gel contamination by Burkholderia cepacia in an Italian hospitalpubmed.ncbi.nlm.nih.gov

Prolonged postprocedural outbreak of Mycobacterium massiliense infections associated with ultrasound transmission gel - PubMed
Postprocedural infections by Mycobacterium abscessus complex are increasing worldwide, and the source and route of transmission are infrequently identified. Here the extension of a previous clustering of paediatric patients with surgical site infections due to a single strain of the subspecies...pubmed.ncbi.nlm.nih.gov
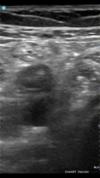
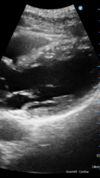
when i was last in ER, ER residents were taught how to do this study.One of my partner’s PAs grabbed me as I was coming in this morning and asked if I would take a look at a patient she was worried had a DVT. I told her about the ultrasound yesterday and she was very interested in potential uses for it. Told the patient I’m not a sonographer and he would need to have a real study performed regardless, but apparently his PCP had ordered it a few days before and he hadn’t been contacted to schedule yet. Started with the popliteal fossa, and sure enough, he had a DVT! Sent him to the ER and they did a formal study that confirmed it.
View attachment 345091
Also, here’s a parasternal long axis view of my heart.
View attachment 345093
Ultrasound has become only really worth it for regen now. As part of an ortho group, I do a ton of ultrasound guided procedures and realize I’m not getting paid for use of the ultrasound. Have gotten to the point where I have my assistant book out baker’s cyst aspirations and glut med tenon injections and proximal hamstring tendons, unless they are my own patients. It’s a great diagnostic tool, but unfortunately have to balance finances with offering the service to patientsFor BILLING -- It is my understanding that a pre and post injection image needs to be saved. Is that the case?
And WHERE are you storing images?
Why are you not getting paid for the ultrasound? There is a small difference between the 20610 and 20611, but with high volume it certainly makes sense. Of course, you have to own the ultrasound machine to collect the technical competent that helps with that payment.Ultrasound has become only really worth it for regen now. As part of an ortho group, I do a ton of ultrasound guided procedures and realize I’m not getting paid for use of the ultrasound. Have gotten to the point where I have my assistant book out baker’s cyst aspirations and glut med tenon injections and proximal hamstring tendons, unless they are my own patients. It’s a great diagnostic tool, but unfortunately have to balance finances with offering the service to patients
How has the Vscan air treated you now that you're 6 months in? How is the needle visualization? Is it suitable for PNS? I'm highly considering ordering one.Got the Vscan Air today. The iPad still hasn’t shipped yet but I’ve tried it with my phone.
Haven’t used it on a patient but scanned my heart, lungs, and a few nerves. Impressed by the quality for such a small unit. Not sure if it’s any better than the Butterfly, which is half the price, but there’s no yearly membership fee, and no wire to break. Got myself a Pelican case to hold it all. Will upload some images when I get some clinical ones and keep you posted.
How was the needle visualization?I am demo'ing vscan right now. Picture quality is better than I expected. Have not tried injection with yet, so have not visualized needle.
I plan on buying butterfly and "trialing" it for 2 weeks. Will let you know.
I would appeal and bill for a diagnostic scan which should be reimbursed. You will get denied for the guidance by most commercial carriers as they will only pay for specific conditions-for example Aetna requires a failed blind injection for most joints first before they pay for guidance. At least you can get something for your efforts.I just got us code denial for lateral epicondylitis from bcbs. Biller fought it and we lost appeal.
outside of a heavy regen Med practice I would be hard pressed to justifying paying for more than the butterfly us these days.

You can bill a diagnostic scan first. (Document the depth of injection target/site of maximal tenderness with sonopalpation) and get reimbursed for the dx scan. I use a limted scan code. I still document a guided injection as well but I don’t bill the guidance code (since it does not pay with most carriers and if you do a diagnostic scan first ncci edits don’t allow for guidance billing)Ultrasound has become only really worth it for regen now. As part of an ortho group, I do a ton of ultrasound guided procedures and realize I’m not getting paid for use of the ultrasound. Have gotten to the point where I have my assistant book out baker’s cyst aspirations and glut med tenon injections and proximal hamstring tendons, unless they are my own patients. It’s a great diagnostic tool, but unfortunately have to balance finances with offering the service to patients
Billing a diagnostic code in this situation is not recommended. This is bundled into the injection code and you are not diagnosing anything.You can bill a diagnostic scan first. (Document the depth of injection target/site of maximal tenderness with sonopalpation) and get reimbursed for the dx scan. I use a limted scan code. I still document a guided injection as well but I don’t bill the guidance code (since it does not pay with most carriers and if you do a diagnostic scan first ncci edits don’t allow for guidance billing)
Not recommended by who?Billing a diagnostic code in this situation is not recommended. This is bundled into the injection code and you are not diagnosing anything.
Maybe you could clarify what you are billing or give some examples. I work with a large ortho group and for example:Not recommended by who?
Ultrasound can be used for diagnostic purposes as well as interventional planning. When you order an xray-is there always pathology?
ligament tears, calcific tendons, normal scan, etc,,
I am not sure, if you fully read the post
For clarityMaybe you could clarify what you are billing or give some examples. I work with a large ortho group and for example:
When I get a referral for an
1. IA hip injection (20611)
2. Subacromial injection (20611)
3. Greater troch injection (20611)
4. Glenohumeral injection (20611)
5. AC injection (20606)
6. CMC injection (20604)
I am able to bill the appropriate US code listed.
If its a biceps tendon, Iliopsoas tendon, or deQuervains injxn I would use 76942 and 20550.
Not appropriate to bill 76881 or 76882 (diagnostic codes) for any of these. Im not diagnosing anything and I can't just add it because insurance will "cover" it. If fact, Medicare won't pay even if you bill for them together.
For example, If they send me a case of "eval rotator cuff" and inject if appropriate. I could code both, but both won't get paid.
If they send a patient like that its best to just send patient back and let them resend for SAC or IA injection.
Hope that helps
Unfortunately, fluoro is not always covered.Bummer the codes don’t reliably pay ultrasound any longer.
I would just do all of those joint injection procedures you listed under x ray , quicker, and you get paid for the fluoro code.
Only really need US for tendon/nerve injections.
Maybe not Aetna but joint fluoro is covered by Medicare, BCBS, WC, etc so more than 75% of most patients you treat in private practice.Unfortunately, fluoro is not always covered.
Aetna considers fluoroscopic guidance for viscosupplementation experimental and investigational. There is a tendency for carriers to follow each other when it comes to these matters.
I hate to be the harbinger of bad news.
3/4 full or 1/4 empty 🤷♂️Maybe not Aetna but fluoro is covered by Medicare, BCBS, WC, so more than 75% of most peoples practices.
