You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
acidosis and contractility
- Thread starter marktwain
- Start date
- Joined
- May 24, 2009
- Messages
- 4,673
- Reaction score
- 10,736
- Points
- 7,901
- Attending Physician
If you are acidotic then H+ is going to be coming into the cell from the extracellular space which will cause K+ to efflux out. In heart tissue this means that K+ will be leaving the cell causing the resting membrane potential to become more negative and thus less excitable.
- Joined
- Jul 18, 2006
- Messages
- 416
- Reaction score
- 2
- Points
- 4,601
- Fellow [Any Field]
I think (in addition to the HyperK+) the H+ ions also protonate and inactivate Na Channels.
- Joined
- Feb 28, 2011
- Messages
- 43
- Reaction score
- 6
- Points
- 4,651
- Medical Student
The idea that acidosis (i.e. incr [H+]) leads to efflux of K+ from cardiac myocytes --> hyperpolarization and thus decreased contractility makes sense, but is there such thing as a H+/K+ exchanger on such cell types? I've looked in BRS Physiology, but can't find one. There is a Na+/H+ exchanger, but that's different.
Plus, this article states that "the dominant mechanism for the reduction of contractility in whole tissue is competitive inhibition of the slow calcium current by hydrogen ions."
I know this is an old thread, but would anyone care to shed some light on this issue? Thanks!
There are some other conjectures which can be found here.
Plus, this article states that "the dominant mechanism for the reduction of contractility in whole tissue is competitive inhibition of the slow calcium current by hydrogen ions."
I know this is an old thread, but would anyone care to shed some light on this issue? Thanks!
There are some other conjectures which can be found here.
- Joined
- Dec 23, 2013
- Messages
- 11
- Reaction score
- 5
- Points
- 4,531
- Medical Student
I always thought that the effects of acidosis and alkalosis on muscle (tetany / low contractility) were via Ca++.
I was told that: H+ and Ca++ ions compete for binding sites on albumin, so in acidotis the Ca++ will be displaced by additional H+ --> More free Ca++ in circulation --> inhibition of muscle Na+ channels by Ca++ (this is the paradoxical step, as you'd expect more Ca++ to increase contractility. I'm not sure what the mechanism of inhibition is here.)
The reverse being true of alkalosis causing tetany - less H+ allows Ca++ to bind to albumin, releasing the inhibition of Na+ channels causing tetany and paraesthesia (due to a similar effect on sensory neurons).
I was told that: H+ and Ca++ ions compete for binding sites on albumin, so in acidotis the Ca++ will be displaced by additional H+ --> More free Ca++ in circulation --> inhibition of muscle Na+ channels by Ca++ (this is the paradoxical step, as you'd expect more Ca++ to increase contractility. I'm not sure what the mechanism of inhibition is here.)
The reverse being true of alkalosis causing tetany - less H+ allows Ca++ to bind to albumin, releasing the inhibition of Na+ channels causing tetany and paraesthesia (due to a similar effect on sensory neurons).
- Joined
- Mar 5, 2014
- Messages
- 1,098
- Reaction score
- 102
- Points
- 4,651
- Medical Student
sooo which one is it?
- Joined
- Dec 16, 2013
- Messages
- 275
- Reaction score
- 152
- Points
- 5,151
The first explanations don't really address contractility. I always equated contractility with how much Ca2+ is in the cell..not how depolarized a cell is. Hyperkalemia will definitely affect the SA node though. The explanation by coninmedia or w/e his name sounds most correct and the article provided backs it up pretty well.
- Joined
- Jan 30, 2013
- Messages
- 1,933
- Reaction score
- 2,439
- Points
- 5,751
- Location
- North of the Wall
- Attending Physician
The only case where I've heard this explanation being used is to explain the physiologic symptoms of hypocalcemia with respiratory alkalosis (decreased H+ leads to increased Ca binding of albumin which decreases free serum Ca). I do not think that this mechanism applies to all acid/base disturbances.I always thought that the effects of acidosis and alkalosis on muscle (tetany / low contractility) were via Ca++.
I was told that: H+ and Ca++ ions compete for binding sites on albumin, so in acidotis the Ca++ will be displaced by additional H+ --> More free Ca++ in circulation --> inhibition of muscle Na+ channels by Ca++ (this is the paradoxical step, as you'd expect more Ca++ to increase contractility. I'm not sure what the mechanism of inhibition is here.)
The reverse being true of alkalosis causing tetany - less H+ allows Ca++ to bind to albumin, releasing the inhibition of Na+ channels causing tetany and paraesthesia (due to a similar effect on sensory neurons).
- Joined
- Mar 5, 2014
- Messages
- 1,098
- Reaction score
- 102
- Points
- 4,651
- Medical Student
so anyone? Dfib slim perhaps care to explain this?
- Joined
- Aug 20, 2012
- Messages
- 1,277
- Reaction score
- 1,046
- Points
- 5,321
- Attending Physician
I remember something from class about a decrease in sensitivity of adrenergic receptors to catecholamines during acidosis. Less beta 1 response, less contractility.
http://ccforum.com/content/16/4/r153
Other articles online talk about decreased calcium influx and/or decreased binding of troponin C to calcium.
http://ajpcell.physiology.org/content/258/6/C967
http://www.ncbi.nlm.nih.gov/pubmed/6804193
http://ccforum.com/content/16/4/r153
Other articles online talk about decreased calcium influx and/or decreased binding of troponin C to calcium.
http://ajpcell.physiology.org/content/258/6/C967
http://www.ncbi.nlm.nih.gov/pubmed/6804193
- Joined
- Jan 10, 2016
- Messages
- 1
- Reaction score
- 4
- Points
- 4,551
- Medical Student
Here is how I choose to think of it:
1. If we are acidotic, the alpha intercalated cells in the kidney are going to be spitting Hydrogen into the filtrate, which it can only do by reabsorbing K in to the blood. Thus, you get to a hyperkalemic state in the blood.
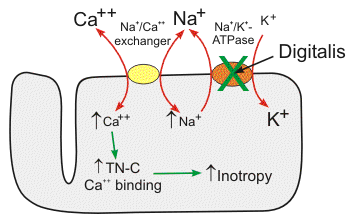
2. In the heart, the increased serum K will be exchanged for Na, increasing the the extracellular concentration of sodium.
3. The increased extracellular concentration of sodium will drive the Na/Ca exchanger, thus driving more calcium out of the cell, decreasing intracellular concentrations of Calcium
4. Decreased intracellular Ca = decreased contractility
It basically works the exact opposite of digoxin. I don't know if this is close to how it actually works, it's just they way I could make sense of it.
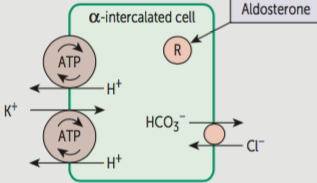
1. If we are acidotic, the alpha intercalated cells in the kidney are going to be spitting Hydrogen into the filtrate, which it can only do by reabsorbing K in to the blood. Thus, you get to a hyperkalemic state in the blood.
2. In the heart, the increased serum K will be exchanged for Na, increasing the the extracellular concentration of sodium.
3. The increased extracellular concentration of sodium will drive the Na/Ca exchanger, thus driving more calcium out of the cell, decreasing intracellular concentrations of Calcium
4. Decreased intracellular Ca = decreased contractility
It basically works the exact opposite of digoxin. I don't know if this is close to how it actually works, it's just they way I could make sense of it.
Attachments
- Joined
- Sep 1, 2016
- Messages
- 14
- Reaction score
- 3
- Points
- 4,621
- Medical Student
" ....It has been previously suggested that H+ may interfere directly with Ca2+ entry into the myocardial cells. This may occur because of competition between H+ and Ca2+ for superficial binding sites on the sarcolemma. Voltage clamp experiments on frog atrial fibers have shown that artificial buffer acidosis decreases the slow inward calcium current that occurs during the plateau phase of the action potential....."
Steenbergen, C., Deleeuw, G., Rich, T. E. R. R. E. L. L., & Williamson, J. R. (1977). Effects of acidosis and ischemia on contractility and intracellular pH of rat heart. Circulation research, 41(6), 849-858.
Steenbergen, C., Deleeuw, G., Rich, T. E. R. R. E. L. L., & Williamson, J. R. (1977). Effects of acidosis and ischemia on contractility and intracellular pH of rat heart. Circulation research, 41(6), 849-858.
Although not directly related to the original question, as someone with extensive electrophys background, I just want to correct a common misunderstanding involving hyperkalemia and RMP, i.e. the thinking that hyperkalemia causes the resting membrane potential (RMP) to be more negative and therefore the heart less excitable.
This explanation, although seemingly very intuitive, is actually false, and can cause problems down the line when trying to explain other arrhythmias that occur with electrolyte abnormalities. Therefore, I think it's important to clarify this point: hyperkalemia causes the RMP to actually be more positive (in fact, it's HYPOkalemia that causes the RMP to be more negative; see attached image). Weird, I know, but bear with me.
The reason for this is because electrical charge across membranes is determined by the flow (or more accurately, the INCENTIVE to flow) of ions across membranes, not the concentrations of ions themselves. For example, K+ is a mostly intracellular ion (140 mM inside vs. 5 mM outside) that carries a positive charge. Therefore, based on the default RMP of -90 mV in the heart, the direction that K+ naturally likes to flow is out of the cell. Since K+ is a positive ion, the more it wants to flow out of the cell, the more negative the intracellular space will become. Therefore, if you look at how RMP is affected by K+ based on how much INCENTIVE it has to flow out of the cell, how hyper- and hypokalemia respectively affect the RMP becomes clear.
So let's look at hyperkalemia. In hyperkalemia, the extracellular K+ concentration increases to >5 mM. Assuming the intracellular K+ stays largely unchanged at 140 mM due to how strictly cells regulate their potassium, the concentration gradient of intracellular vs. extracellular K+ will decrease. This decreased gradient in turn reduces the incentive for K+ to flow out of the cell (i.e. more K+ wants to stay inside the cell now). And since K+ is a positive ion, the decreased incentive to flow out makes the inside of the cell more positive compared to the outside, hence raising the RMP. The reverse is true for hypokalemia.
Does these minute details matter? Yes, because knowing that hyperkalemia makes the RMP more positive can help explain why a lot of patients with hyperkalemia (particularly mild hyperkalemia) experience cardiac hyperexcitability and palpitations (because the RMP is now closer to the cardiac action potential threshold). Interestingly however, more severe hyperkalemia will have the paradoxical effect of decreasing cardiac excitability due to the progressive inactivation of sodium channels at RMPs higher than -70, which counteracts the effect of the RMP being close to the action potential threshold. In summary, hyperkalemia has an fascinating biphasic effect on the heart depending on how severe it is: mild hyperkalemia causes the heart to go into overdrive, while more severe hyperkalemia will cause QRS prolongation (because of sodium channel inactivation) and dampen overall heart function.
This explanation, although seemingly very intuitive, is actually false, and can cause problems down the line when trying to explain other arrhythmias that occur with electrolyte abnormalities. Therefore, I think it's important to clarify this point: hyperkalemia causes the RMP to actually be more positive (in fact, it's HYPOkalemia that causes the RMP to be more negative; see attached image). Weird, I know, but bear with me.
The reason for this is because electrical charge across membranes is determined by the flow (or more accurately, the INCENTIVE to flow) of ions across membranes, not the concentrations of ions themselves. For example, K+ is a mostly intracellular ion (140 mM inside vs. 5 mM outside) that carries a positive charge. Therefore, based on the default RMP of -90 mV in the heart, the direction that K+ naturally likes to flow is out of the cell. Since K+ is a positive ion, the more it wants to flow out of the cell, the more negative the intracellular space will become. Therefore, if you look at how RMP is affected by K+ based on how much INCENTIVE it has to flow out of the cell, how hyper- and hypokalemia respectively affect the RMP becomes clear.
So let's look at hyperkalemia. In hyperkalemia, the extracellular K+ concentration increases to >5 mM. Assuming the intracellular K+ stays largely unchanged at 140 mM due to how strictly cells regulate their potassium, the concentration gradient of intracellular vs. extracellular K+ will decrease. This decreased gradient in turn reduces the incentive for K+ to flow out of the cell (i.e. more K+ wants to stay inside the cell now). And since K+ is a positive ion, the decreased incentive to flow out makes the inside of the cell more positive compared to the outside, hence raising the RMP. The reverse is true for hypokalemia.
Does these minute details matter? Yes, because knowing that hyperkalemia makes the RMP more positive can help explain why a lot of patients with hyperkalemia (particularly mild hyperkalemia) experience cardiac hyperexcitability and palpitations (because the RMP is now closer to the cardiac action potential threshold). Interestingly however, more severe hyperkalemia will have the paradoxical effect of decreasing cardiac excitability due to the progressive inactivation of sodium channels at RMPs higher than -70, which counteracts the effect of the RMP being close to the action potential threshold. In summary, hyperkalemia has an fascinating biphasic effect on the heart depending on how severe it is: mild hyperkalemia causes the heart to go into overdrive, while more severe hyperkalemia will cause QRS prolongation (because of sodium channel inactivation) and dampen overall heart function.
Attachments
Similar threads
- Replies
- 0
- Views
- 248
- Replies
- 0
- Views
- 3K


