You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
- Joined
- Aug 24, 2011
- Messages
- 846
- Reaction score
- 2,068
- Points
- 5,496
- Attending Physician
Spinal (~7.5-10 mg hyperbaric bupivacaine) with 0.1 mg PF morphine plus single shot adductor canal. Will modify based on patient and surgeon (will consider more morphine/bupivacaine in spinal)
D
deleted87051
Spinal (~7.5-10 mg hyperbaric bupivacaine) with 0.1 mg PF morphine plus single shot adductor canal. Will modify based on patient and surgeon (will consider more morphine/bupivacaine in spinal)
Same
- Joined
- Mar 13, 2003
- Messages
- 2,205
- Reaction score
- 1,254
- Points
- 5,226
- Attending Physician
What they said, but with isobaric bupiv
D
deleted162650
SS ACB w/ 10mg isobaric Bupi spinal w/ 20mcg fent. I find the fent lasts jut long enough to ease the transition in PACU as the spinal is wearing off w/ many pts having return of motor function and still zero to minimal pain. Surgeons are also doing exparel local infltation. IT morphine out of favor at my institution outside of OB.
- Joined
- Jan 21, 2005
- Messages
- 1,324
- Reaction score
- 2,317
- Points
- 5,451
- Location
- CA
- Attending Physician
Protocol for most of our surgeons:
Spinal with duramorph, continuous adductor canal catheter
Spinal with duramorph, continuous adductor canal catheter
- Joined
- May 28, 2008
- Messages
- 2,524
- Reaction score
- 3,135
- Points
- 5,281
- Location
- Neither here nor there
- Attending Physician
Protocol for most of our surgeons:
Spinal with duramorph, continuous adductor canal catheter
We did these for awhile but the paperwork/maintenance was too much of a headache. Single shot ACB with Exparel.
- Joined
- Jul 16, 2003
- Messages
- 6,484
- Reaction score
- 4,872
- Points
- 6,481
- Attending Physician
If you are gathering metrics on patient satisfaction scores, time to pacu D/C and time to ambulation, then you can't beat IT + ACB. Small dose of IT duramorph can help over 24 hrs.
- Joined
- Apr 22, 2007
- Messages
- 22,997
- Reaction score
- 10,020
- Points
- 9,821
- Location
- Southeast
- Attending Physician
1. SAB
2. Single shot ACB or Femoral (surgeon preference)
3. If Painful in PACU then rescue popliteal/sciatic block (single shot)
2. Single shot ACB or Femoral (surgeon preference)
3. If Painful in PACU then rescue popliteal/sciatic block (single shot)
Advertisement - Members don't see this ad
- Joined
- Apr 22, 2007
- Messages
- 22,997
- Reaction score
- 10,020
- Points
- 9,821
- Location
- Southeast
- Attending Physician
1. SAB
2. Single shot ACB or Femoral (surgeon preference)
3. If Painful in PACU then rescue popliteal/sciatic block (single shot)
I'd like to add #4 which is LIA of Exparel by all the surgeons.
- Joined
- May 21, 2010
- Messages
- 475
- Reaction score
- 315
- Points
- 5,241
- Attending Physician
Those of you using intrathecal morphine, are you also having the patient on a continuous pulse ox for 24 hours? Thats the main reason i avoid using it.
- Joined
- Apr 22, 2007
- Messages
- 22,997
- Reaction score
- 10,020
- Points
- 9,821
- Location
- Southeast
- Attending Physician
Those of you using intrathecal morphine, are you also having the patient on a continuous pulse ox for 24 hours? Thats the main reason i avoid using it.
Many of my patients are over 75 with a significant number over 80. While I believe IT MSO4 0.1 mg is perfectly safe I do not want any increased liability. Hence, I would avoid it on high risk groups: Morbidly Obese, Sleep Apnea, Elderly to name a few. That said, the use of IT MSo4 is perfectly fine for many patients and 0.1 mg IT combined with 15-20 ug of Fentanyl IT would be a nice adjunct to the blocks/LIA.
- Joined
- Apr 22, 2007
- Messages
- 22,997
- Reaction score
- 10,020
- Points
- 9,821
- Location
- Southeast
- Attending Physician
Eur Rev Med Pharmacol Sci. 2010 Jul;14(7):589-96.
Post-operative analgesia following total knee arthroplasty: comparison of low-dose intrathecal morphine and single-shot ultrasound-guided femoral nerve block: a randomized, single blinded, controlled study.
Frassanito L1, Vergari A, Zanghi F, Messina A, Bitondo M, Antonelli M.
Author information
Abstract
BACKGROUND AND OBJECTIVES:
Total knee arthroplasty often results in marked postoperative pain. A recent meta-analysis supports the use of femoral nerve block or alternatively spinal injection of morphine plus local anaesthetic for post-operative analgesia. On the other hand, the use of intrathecal morphine may be associated with a large number of distressing side effects (itching, urinary retention, nausea and vomiting, delayed respiratory depression). The aim of this study was to compare the effectiveness of femoral nerve block and low dose intrathecal morphine in post-operative analgesia after primary unilateral total knee arthroplasty.
MATERIAL AND METHODS:
Fifty-two consecutive patients scheduled for primary unilateral total knee arthroplasty were allocated to the intrathecal morphine group (ITM group) or to the femoral nerve block group (FNB group). In ITM group a subarachnoid puncture was performed at the L3-L4 inter-vertebral space with hyperbaric bupivacaine 15 mg plus 100 mcg of preservative-free morphine. Patients allocated to the FNB group received a single-injection ultrasound-assisted femoral nerve block with ropivacaine 0.75% 25 ml before the spinal injection of hyperbaric bupivacaine 15 mg. All patients received postoperative patient-controlled-analgesia (PCA) morphine, using a 1-mg bolus and a 5-minute lockout period. Data were analyzed using Student t test or two-way analysis of variance (ANOVA) for repeated measures with time and treatment as the 2 factors. Post hoc comparisons were performed by Bonferroni test. Statistical significance for all test was a p value < 0.05.
RESULTS:
Patient characteristics were similar between the 2 groups. We found a statistically significant differences in postoperative pain between the two groups: ITM group had the lower visual analogic pain score (VAS) values. Morphine consumption was lower in the ITM group: average consumption within the first 6 hours was 0.9 mg in IT group compared to 3.1 mg in FNB group; at 12 h 4.2 mg vs 6.3 mg; at 24 h 6.9 mg vs 10.3 mg; at 48 h 9.7 mg vs 13.6 mg. However, the difference in the opiate consumption was not statistically different (p value = 0.06). Thirteen patients in ITM group experienced itching, only 5 in FNB group. We did not find any difference in the two treatment groups in the use of antiemetic and antipruritic medication. No cases of respiratory depression was recorded.
CONCLUSIONS:
Our results show that low dose of intrathecal morphine may be safe and more efficient than single-shot femoral nerve block for post-operative analgesia after total knee arthroplasty.
Post-operative analgesia following total knee arthroplasty: comparison of low-dose intrathecal morphine and single-shot ultrasound-guided femoral nerve block: a randomized, single blinded, controlled study.
Frassanito L1, Vergari A, Zanghi F, Messina A, Bitondo M, Antonelli M.
Author information
Abstract
BACKGROUND AND OBJECTIVES:
Total knee arthroplasty often results in marked postoperative pain. A recent meta-analysis supports the use of femoral nerve block or alternatively spinal injection of morphine plus local anaesthetic for post-operative analgesia. On the other hand, the use of intrathecal morphine may be associated with a large number of distressing side effects (itching, urinary retention, nausea and vomiting, delayed respiratory depression). The aim of this study was to compare the effectiveness of femoral nerve block and low dose intrathecal morphine in post-operative analgesia after primary unilateral total knee arthroplasty.
MATERIAL AND METHODS:
Fifty-two consecutive patients scheduled for primary unilateral total knee arthroplasty were allocated to the intrathecal morphine group (ITM group) or to the femoral nerve block group (FNB group). In ITM group a subarachnoid puncture was performed at the L3-L4 inter-vertebral space with hyperbaric bupivacaine 15 mg plus 100 mcg of preservative-free morphine. Patients allocated to the FNB group received a single-injection ultrasound-assisted femoral nerve block with ropivacaine 0.75% 25 ml before the spinal injection of hyperbaric bupivacaine 15 mg. All patients received postoperative patient-controlled-analgesia (PCA) morphine, using a 1-mg bolus and a 5-minute lockout period. Data were analyzed using Student t test or two-way analysis of variance (ANOVA) for repeated measures with time and treatment as the 2 factors. Post hoc comparisons were performed by Bonferroni test. Statistical significance for all test was a p value < 0.05.
RESULTS:
Patient characteristics were similar between the 2 groups. We found a statistically significant differences in postoperative pain between the two groups: ITM group had the lower visual analogic pain score (VAS) values. Morphine consumption was lower in the ITM group: average consumption within the first 6 hours was 0.9 mg in IT group compared to 3.1 mg in FNB group; at 12 h 4.2 mg vs 6.3 mg; at 24 h 6.9 mg vs 10.3 mg; at 48 h 9.7 mg vs 13.6 mg. However, the difference in the opiate consumption was not statistically different (p value = 0.06). Thirteen patients in ITM group experienced itching, only 5 in FNB group. We did not find any difference in the two treatment groups in the use of antiemetic and antipruritic medication. No cases of respiratory depression was recorded.
CONCLUSIONS:
Our results show that low dose of intrathecal morphine may be safe and more efficient than single-shot femoral nerve block for post-operative analgesia after total knee arthroplasty.
- Joined
- Apr 22, 2007
- Messages
- 22,997
- Reaction score
- 10,020
- Points
- 9,821
- Location
- Southeast
- Attending Physician
Rostral spread within the CSF may produce respiratory depression, although this complication is extremely rare with the 100–200 µg doses that are used in current clinical practice. The timing of this complication is as early as 20–30 min after administration of lipophilic agents but as late as 24 h following intrathecal administration of morphine. It is crucial that appropriate monitoring for signs of respiratory depression be continued for at least 24 h post-operatively. The best early indicator of respiratory depression is increasing sedation; therefore, ward staff must be trained to monitor patients appropriately. A protocol should be in place for the management of delayed respiratory depression should this very rare complication arise.
http://ceaccp.oxfordjournals.org/content/8/2/56.full
http://ceaccp.oxfordjournals.org/content/8/2/56.full
- Joined
- Apr 22, 2007
- Messages
- 22,997
- Reaction score
- 10,020
- Points
- 9,821
- Location
- Southeast
- Attending Physician
- Joined
- Apr 22, 2007
- Messages
- 22,997
- Reaction score
- 10,020
- Points
- 9,821
- Location
- Southeast
- Attending Physician
REVIEW ARTICLE Risks and side-effects of intrathecal morphine combined with spinal anaesthesia: a meta-analysis
M. Gehling1 and M. Tryba2 1 Consultant Anaesthetist and 2 Head of Department, Department of Anaesthesiology, Intensive Care Medicine and Pain Therapy, Klinikum Kassel, Kassel, Germany
Summary: Intrathecal morphine is often used for postoperative analgesia after surgery. We performed a meta-analysis to obtain more detailed information on the frequency of side-effects in patients receiving intrathecal morphine in combination with spinal anaesthesia compared with placebo treated patients. We clustered the analysis to patients receiving placebo, less than morphine 0.3 mg (M < 0.3), or equal to or more than morphine 0.3 mg (M ‡ 0.3) and calculated the risk ratios of morphine vs placebo. Twenty-eight studies investigating 46 morphine groups vs placebo were included. A total of 790 patients with intrathecal morphine and 524 patients who received placebo were analysed. Compared with placebo the lower dose of morphine resulted in an increase of nausea (RR 1.4, 95% CI 1.1–1.7), vomiting (RR 3.1, 95% CI 1.5–6.4) and pruritus (RR 1.8, 95% CI 1.4–2.2). The higher dose resulted in an increased risk ratio for pruritus (RR 5.0, 95% CI 2.9–8.6), but not nausea (RR 1.2, 95% CI 0.9–1.6) or vomiting (RR 1.3, 95% CI 0.9–1.9). Overall, intrathecal morphine did not increase respiratory depression. However, the higher dose of intrathecal morphine was associated with more episodes of respiratory depression (7 ⁄ 80) compared with the lower dose (2 ⁄ 247). Intrathecal morphine is associated with a mild increase in side-effects. With a dose < 0.3 mg we found there were no more episodes of respiratory depression than in placebo patients who received systemic opioid analgesia.
http://www.researchgate.net/profile...a-analysis/links/543fa38e0cf27832ae8badc9.pdf
M. Gehling1 and M. Tryba2 1 Consultant Anaesthetist and 2 Head of Department, Department of Anaesthesiology, Intensive Care Medicine and Pain Therapy, Klinikum Kassel, Kassel, Germany
Summary: Intrathecal morphine is often used for postoperative analgesia after surgery. We performed a meta-analysis to obtain more detailed information on the frequency of side-effects in patients receiving intrathecal morphine in combination with spinal anaesthesia compared with placebo treated patients. We clustered the analysis to patients receiving placebo, less than morphine 0.3 mg (M < 0.3), or equal to or more than morphine 0.3 mg (M ‡ 0.3) and calculated the risk ratios of morphine vs placebo. Twenty-eight studies investigating 46 morphine groups vs placebo were included. A total of 790 patients with intrathecal morphine and 524 patients who received placebo were analysed. Compared with placebo the lower dose of morphine resulted in an increase of nausea (RR 1.4, 95% CI 1.1–1.7), vomiting (RR 3.1, 95% CI 1.5–6.4) and pruritus (RR 1.8, 95% CI 1.4–2.2). The higher dose resulted in an increased risk ratio for pruritus (RR 5.0, 95% CI 2.9–8.6), but not nausea (RR 1.2, 95% CI 0.9–1.6) or vomiting (RR 1.3, 95% CI 0.9–1.9). Overall, intrathecal morphine did not increase respiratory depression. However, the higher dose of intrathecal morphine was associated with more episodes of respiratory depression (7 ⁄ 80) compared with the lower dose (2 ⁄ 247). Intrathecal morphine is associated with a mild increase in side-effects. With a dose < 0.3 mg we found there were no more episodes of respiratory depression than in placebo patients who received systemic opioid analgesia.
http://www.researchgate.net/profile...a-analysis/links/543fa38e0cf27832ae8badc9.pdf
- Joined
- Feb 19, 2009
- Messages
- 614
- Reaction score
- 228
- Points
- 5,181
- Attending Physician
Most of our surgeons perform an intraop local injection of what is called a "Lombardi" cocktail, which includes ropivacaine, ketorolac, dexamethasone, and perhaps a few other things.
We used to do all of these with general anesthesia. 2 surgeons now want spinals (but we don't do the intrathecal morphine).
Another surgeon now wants general, the Lombardi cocktail, and an adductor canal block. We are currently working out the details so we don't give a toxic dose of ropivacaine.
No one here has used exparel, however, you can make your own version by adding preservative free dexamethasone to your local.
We used to do all of these with general anesthesia. 2 surgeons now want spinals (but we don't do the intrathecal morphine).
Another surgeon now wants general, the Lombardi cocktail, and an adductor canal block. We are currently working out the details so we don't give a toxic dose of ropivacaine.
No one here has used exparel, however, you can make your own version by adding preservative free dexamethasone to your local.
- Joined
- Apr 22, 2007
- Messages
- 22,997
- Reaction score
- 10,020
- Points
- 9,821
- Location
- Southeast
- Attending Physician
Br J Anaesth. 2013 Nov;111(5):793-9. doi: 10.1093/bja/aet248. Epub 2013 Jul 19.
Postoperative pain relief after total hip arthroplasty: a randomized, double-blind comparison between intrathecal morphine and local infiltration analgesia.
Kuchálik J1, Granath B, Ljunggren A, Magnuson A, Lundin A, Gupta A.
Author information
Abstract
BACKGROUND:
Postoperative pain after total hip arthroplasty (THA) can delay mobilization. This was assessed after intrathecal morphine (ITM) compared with local infiltration analgesia (LIA) using a non-inferiority design.
METHODS:
Eighty patients were recruited in this randomized, double-blind study. ITM 0.1 mg (Group ITM) or periarticular local anaesthetic (ropivacaine 300 mg)+ketorolac 30 mg+ epinephrine 0.5 mg (total volume 151.5 ml) (Group LIA) were compared. After 24 h, 22 ml of saline (Group ITM) or ropivacaine (150 mg)+ketorolac (30 mg)+epinephrine (0.1 mg) (Group LIA) were injected via a catheter. After operation, rescue analgesic consumption, pain intensity, and home-readiness were measured.
RESULTS:
Morphine consumption was equivalent, median difference 0 mg (95% confidence interval -4 to 4.5) between the groups at 0-24 h. During 24-48 h, it was lower in Group LIA (3 mg, 0-60 mg, median, range) compared with Group ITM (10 mg, 0-81 mg) (P=0.01). Lower pain scores were recorded at rest at 8 h in Group ITM (P<0.01), but in Group LIA on standing and mobilization, at 24-48 h (P<0.01). Paracetamol and tramadol consumption was lower in Group LIA (P=0.05 and 0.05, respectively) as was pruritus, nausea, and vomiting (P<0.05).
CONCLUSION:
Lower pain intensity was recorded early after surgery in ITM group but later, analgesic consumption, pain intensity on mobilization, and side-effects were lower in patients receiving LIA. LIA is a good alternative to ITM in patients undergoing THA.
Postoperative pain relief after total hip arthroplasty: a randomized, double-blind comparison between intrathecal morphine and local infiltration analgesia.
Kuchálik J1, Granath B, Ljunggren A, Magnuson A, Lundin A, Gupta A.
Author information
Abstract
BACKGROUND:
Postoperative pain after total hip arthroplasty (THA) can delay mobilization. This was assessed after intrathecal morphine (ITM) compared with local infiltration analgesia (LIA) using a non-inferiority design.
METHODS:
Eighty patients were recruited in this randomized, double-blind study. ITM 0.1 mg (Group ITM) or periarticular local anaesthetic (ropivacaine 300 mg)+ketorolac 30 mg+ epinephrine 0.5 mg (total volume 151.5 ml) (Group LIA) were compared. After 24 h, 22 ml of saline (Group ITM) or ropivacaine (150 mg)+ketorolac (30 mg)+epinephrine (0.1 mg) (Group LIA) were injected via a catheter. After operation, rescue analgesic consumption, pain intensity, and home-readiness were measured.
RESULTS:
Morphine consumption was equivalent, median difference 0 mg (95% confidence interval -4 to 4.5) between the groups at 0-24 h. During 24-48 h, it was lower in Group LIA (3 mg, 0-60 mg, median, range) compared with Group ITM (10 mg, 0-81 mg) (P=0.01). Lower pain scores were recorded at rest at 8 h in Group ITM (P<0.01), but in Group LIA on standing and mobilization, at 24-48 h (P<0.01). Paracetamol and tramadol consumption was lower in Group LIA (P=0.05 and 0.05, respectively) as was pruritus, nausea, and vomiting (P<0.05).
CONCLUSION:
Lower pain intensity was recorded early after surgery in ITM group but later, analgesic consumption, pain intensity on mobilization, and side-effects were lower in patients receiving LIA. LIA is a good alternative to ITM in patients undergoing THA.
- Joined
- Mar 13, 2003
- Messages
- 2,205
- Reaction score
- 1,254
- Points
- 5,226
- Attending Physician
For those wanting hyperbaric bupi: why?
Advertisement - Members don't see this ad
- Joined
- May 21, 2010
- Messages
- 475
- Reaction score
- 315
- Points
- 5,241
- Attending Physician
I completely agree with the effectiveness and low risk for respiratory depression for IT morphine. But I'm just wondering if anyone does it without continuous pulse ox. Our hospital would not be able to handle the monitoring requirements for the volume we do. Not to mention that many of the total joints are going home the same day.REVIEW ARTICLE Risks and side-effects of intrathecal morphine combined with spinal anaesthesia: a meta-analysis
M. Gehling1 and M. Tryba2 1 Consultant Anaesthetist and 2 Head of Department, Department of Anaesthesiology, Intensive Care Medicine and Pain Therapy, Klinikum Kassel, Kassel, Germany
Summary: Intrathecal morphine is often used for postoperative analgesia after surgery. We performed a meta-analysis to obtain more detailed information on the frequency of side-effects in patients receiving intrathecal morphine in combination with spinal anaesthesia compared with placebo treated patients. We clustered the analysis to patients receiving placebo, less than morphine 0.3 mg (M < 0.3), or equal to or more than morphine 0.3 mg (M ‡ 0.3) and calculated the risk ratios of morphine vs placebo. Twenty-eight studies investigating 46 morphine groups vs placebo were included. A total of 790 patients with intrathecal morphine and 524 patients who received placebo were analysed. Compared with placebo the lower dose of morphine resulted in an increase of nausea (RR 1.4, 95% CI 1.1–1.7), vomiting (RR 3.1, 95% CI 1.5–6.4) and pruritus (RR 1.8, 95% CI 1.4–2.2). The higher dose resulted in an increased risk ratio for pruritus (RR 5.0, 95% CI 2.9–8.6), but not nausea (RR 1.2, 95% CI 0.9–1.6) or vomiting (RR 1.3, 95% CI 0.9–1.9). Overall, intrathecal morphine did not increase respiratory depression. However, the higher dose of intrathecal morphine was associated with more episodes of respiratory depression (7 ⁄ 80) compared with the lower dose (2 ⁄ 247). Intrathecal morphine is associated with a mild increase in side-effects. With a dose < 0.3 mg we found there were no more episodes of respiratory depression than in placebo patients who received systemic opioid analgesia.
http://www.researchgate.net/profile...a-analysis/links/543fa38e0cf27832ae8badc9.pdf
- Joined
- Sep 8, 2008
- Messages
- 120
- Reaction score
- 168
- Points
- 4,886
- Attending Physician
For those wanting hyperbaric bupi: why?
It's what's in the kit[emoji4]
- Joined
- Nov 12, 2002
- Messages
- 249
- Reaction score
- 34
- Points
- 4,631
- Attending Physician
1. SAB
2. Single shot ACB or Femoral (surgeon preference)
3. If Painful in PACU then rescue popliteal/sciatic block (single shot)
Sorry if this is a stupid question, but how do you get around the dressing to do a rescue popliteal block on a TKA?
- Joined
- Apr 22, 2007
- Messages
- 22,997
- Reaction score
- 10,020
- Points
- 9,821
- Location
- Southeast
- Attending Physician
Sorry if this is a stupid question, but how do you get around the dressing to do a rescue popliteal block on a TKA?
I can usually pull the dressing down enough to find the popliteal nerve. If the patient is obese or I can't find the popliteal nerve then I do a gluteal or subgluteal sciatic nerve block.
- Joined
- Nov 2, 2006
- Messages
- 7,248
- Reaction score
- 3,089
- Points
- 5,481
- Location
- The South
- Attending Physician
Is there a newly discovered nerve called the popliteal nerve??? 😵
- Joined
- Jun 20, 2005
- Messages
- 8,022
- Reaction score
- 2,816
- Points
- 5,251
- Attending Physician
We do a number of different approaches.
My favorite has been SS FNB (0.5% Ropiv)/Anterior sciatic (1.5% Mepivicaine) and spinal without MS. I felt the duramorph wasn't needed since the FNB out lasted the MS. Also, we stopped placeing foleys in these pts with some surgeons if we didn't use IT MS.
With all that being said, we have one surgeon using exparel so the jury is out on that one. We on,y do spinals on these pts.
I haven't done a GA on a joint in a long time.
My favorite has been SS FNB (0.5% Ropiv)/Anterior sciatic (1.5% Mepivicaine) and spinal without MS. I felt the duramorph wasn't needed since the FNB out lasted the MS. Also, we stopped placeing foleys in these pts with some surgeons if we didn't use IT MS.
With all that being said, we have one surgeon using exparel so the jury is out on that one. We on,y do spinals on these pts.
I haven't done a GA on a joint in a long time.
- Joined
- Nov 2, 2006
- Messages
- 7,248
- Reaction score
- 3,089
- Points
- 5,481
- Location
- The South
- Attending Physician
This is what I did at my previous job, fast paced busy ortho group.We do a number of different approaches.
My favorite has been SS FNB (0.5% Ropiv)/Anterior sciatic (1.5% Mepivicaine) and spinal without MS. I felt the duramorph wasn't needed since the FNB out lasted the MS. Also, we stopped placeing foleys in these pts with some surgeons if we didn't use IT MS.
With all that being said, we have one surgeon using exparel so the jury is out on that one. We on,y do spinals on these pts.
I haven't done a GA on a joint in a long time.
Now I do a femoral and distal sciatic blocks + LMA, usually no intra-op opiates, and patients are pain free for at least 36 hours.
Our patients don't walk the first 24 hours which makes my approach possible.
D
deleted126335
Is there a newly discovered nerve called the popliteal nerve??? 😵
Cute. Snarky. Maybe petty. But cute.
- Joined
- Apr 22, 2007
- Messages
- 22,997
- Reaction score
- 10,020
- Points
- 9,821
- Location
- Southeast
- Attending Physician
Ultrasound-guided popliteal nerve block
- Joined
- Nov 2, 2006
- Messages
- 7,248
- Reaction score
- 3,089
- Points
- 5,481
- Location
- The South
- Attending Physician
Ultrasound-guided popliteal nerve block
The nerve block of the distal sciatic nerve is called popliteal block because of the location but it's not the "popliteal nerve" that is being blocked!!!
Now go search google to find some studies proving that there is a nerve called the popliteal nerve and its best blocked using Exparel!!!
Advertisement - Members don't see this ad
- Joined
- Apr 22, 2007
- Messages
- 22,997
- Reaction score
- 10,020
- Points
- 9,821
- Location
- Southeast
- Attending Physician
The nerve block of the distal sciatic nerve is called popliteal block because of the location but it's not the "popliteal nerve" that is being blocked!!!
Now go search google to find some studies proving that there is a nerve called the popliteal nerve and its best blocked using Exparel!!!
You are ridiculous. It's a Popliteal Sciatic Block which is shortened to Popliteal block for convenience. My previous post was "proof" that others are using the same nomenclature as I was doing in my post. As usual, you find it necessary to post inflammatory or derogatory comments rather than ones which provide any useful information.
- Joined
- Nov 2, 2006
- Messages
- 7,248
- Reaction score
- 3,089
- Points
- 5,481
- Location
- The South
- Attending Physician
You are ridiculous. It's a Popliteal Sciatic Block which is shortened to Popliteal block for convenience. My previous post was "proof" that others are using the same nomenclature as I was doing in my post. As usual, you find it necessary to post inflammatory or derogatory comments rather than ones which provide any useful information.
You said:
I can usually pull the dressing down enough to find the popliteal nerve. If the patient is obese or I can't find the popliteal nerve then I do a gluteal or subgluteal sciatic nerve block.
Is it inflammatory and derogatory if I corrected your obvious ignorance of anatomy?
People say popliteal nerve block because of the anatomical location but no one other than you invented a new nerve called the popliteal nerve professor!
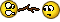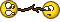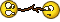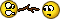
Last edited:
- Joined
- Dec 26, 2006
- Messages
- 7,313
- Reaction score
- 20,116
- Points
- 9,596
- Attending Physician
TKA's get single shot IPACK (http://www.anesthesiologynews.com/ViewArticle.aspx?d=PRN&d_id=21&i=December+2012&i_id=915&a_id=22234) with 20cc 0.25% rop, single shot AC with 15cc 0.25% rop, and AC catheter is placed preop and infusion started in PACU. Intraop is mepiv spinal or mepiv CSE if it's a slow surgeon.
- Joined
- May 28, 2008
- Messages
- 2,524
- Reaction score
- 3,135
- Points
- 5,281
- Location
- Neither here nor there
- Attending Physician
Amidst all the bickering, it's time to take a break and listen to a song from TKA:
- Joined
- Feb 26, 2011
- Messages
- 10
- Reaction score
- 9
- Points
- 4,531
- Attending Physician
for the guys using iso bupi, is it for faster onset?
I found this article that talks about it a bit: http://link.springer.com/article/10.1007/BF03020730
(have to copy/paste the link)
where I trained, the only drug used for SAB was hyperbaric bupi (big academic center, very little total joints and no SAB/epidurals for them, so only SAB for c/s and cerclage and occasional 30 min lower ext I/D).
just curious what dose are you guys using?
we still don't do total joints (other than reverse total shoulders and trauma hemi-arthroplasty hips) here as the guy doing them was a huge douche and everyone was thrilled when he left (no anesth residents allowed in his room but ok for ortho residents to scrub his cases ).
).
I found this article that talks about it a bit: http://link.springer.com/article/10.1007/BF03020730
(have to copy/paste the link)
where I trained, the only drug used for SAB was hyperbaric bupi (big academic center, very little total joints and no SAB/epidurals for them, so only SAB for c/s and cerclage and occasional 30 min lower ext I/D).
just curious what dose are you guys using?
we still don't do total joints (other than reverse total shoulders and trauma hemi-arthroplasty hips) here as the guy doing them was a huge douche and everyone was thrilled when he left (no anesth residents allowed in his room but ok for ortho residents to scrub his cases
 ).
).
D
deleted162650
I use iso bupi because I don't need a thoracic level for a hip or knee. With iso, the dose stays where I put it (lumbar) so a) it's a more HD stable anesthetic and b) it's not nearly as position sensitive (I'll let you think about why heavy bupi is a poor choice for a lateral hip).
I use 10mg iso bupi w/ 15-20mcg fent. The fent is there to ease the transition as the bupi wears off in PACU, and it lets you decrease the bupi dose a little. Most of my pts are moving their legs when I drop them off in PACU and are still totally pain free. The need very little narc in PACU. The fent doesn't add much if anything for the surgery itself and it wouldn't break my heart if I couldn't add it (unlike a C/S where I think it definitely helps intra-op). I also don't notice much of any itching in the joint pts with IT fent unlike the C/S crowd where it's pretty standard (granted they also get Duramorph).
I use 10mg iso bupi w/ 15-20mcg fent. The fent is there to ease the transition as the bupi wears off in PACU, and it lets you decrease the bupi dose a little. Most of my pts are moving their legs when I drop them off in PACU and are still totally pain free. The need very little narc in PACU. The fent doesn't add much if anything for the surgery itself and it wouldn't break my heart if I couldn't add it (unlike a C/S where I think it definitely helps intra-op). I also don't notice much of any itching in the joint pts with IT fent unlike the C/S crowd where it's pretty standard (granted they also get Duramorph).
- Joined
- Jun 20, 2005
- Messages
- 8,022
- Reaction score
- 2,816
- Points
- 5,251
- Attending Physician
Whats the onset and duration of IT fentanyl?I use iso bupi because I don't need a thoracic level for a hip or knee. With iso, the dose stays where I put it (lumbar) so a) it's a more HD stable anesthetic and b) it's not nearly as position sensitive (I'll let you think about why heavy bupi is a poor choice for a lateral hip).
I use 10mg iso bupi w/ 15-20mcg fent. The fent is there to ease the transition as the bupi wears off in PACU, and it lets you decrease the bupi dose a little. Most of my pts are moving their legs when I drop them off in PACU and are still totally pain free. The need very little narc in PACU. The fent doesn't add much if anything for the surgery itself and it wouldn't break my heart if I couldn't add it (unlike a C/S where I think it definitely helps intra-op). I also don't notice much of any itching in the joint pts with IT fent unlike the C/S crowd where it's pretty standard (granted they also get Duramorph).
- Joined
- Jun 20, 2005
- Messages
- 8,022
- Reaction score
- 2,816
- Points
- 5,251
- Attending Physician
Sublimaze,
I use isobaric from time to time. Just as Saltydog described except I use a larger dose, around 15mg. In training I had an attending at the VA who used 25mg and it worked very well. It also lasted damn long. But I never saw an issue from this dose.
I don't believe the onset is faster, actually I think it's slower. Sometimes you will be worried that it's not working well enough for the surgery but it always does.
I use isobaric from time to time. Just as Saltydog described except I use a larger dose, around 15mg. In training I had an attending at the VA who used 25mg and it worked very well. It also lasted damn long. But I never saw an issue from this dose.
I don't believe the onset is faster, actually I think it's slower. Sometimes you will be worried that it's not working well enough for the surgery but it always does.
D
deleted162650
Whats the onset and duration of IT fentanyl?
Onset is 10ish minutes with a duration of 2-4 hours depending on which article you read which works out just about perfect for what I'm hoping to get out of it. I think it also lets me use a lower bupi dose which cuts down on motor block and therefore PACU times. One of our orthopods does anterior total hips and routinely takes 3-3.5 hours and my approach keeps pts comfy for the duration even though I know the Bupi is wearing off by the end.
Like I said though, its non-essential and I could easily do without, but I like the results I get and my PACU nurses like it too. Your mileage may vary.
Advertisement - Members don't see this ad
D
deleted87051
1. Is it legit to bill IT opioids (62311) for IT fentanyl?
2. Does it cause clinically significant urinary retention?
2. Does it cause clinically significant urinary retention?
D
deleted162650
1. Is it legit to bill IT opioids (62311) for IT fentanyl?
2. Does it cause clinically significant urinary retention?
1. Technically I don't know, but I'm almost positive the answer is No. I don't bill for it since I'm not writing post-op pain orders and doing a formal POD#1 check like for a Duramorph pt. The post op pain consult is really what your billing for with IT morph
2. The vast majority of our joints still get Foley'ed so it's a non-issue. I have still done it for one our younger orthopods who doesn't foley everyone and I haven't run into issues yet.
- Joined
- Jun 20, 2005
- Messages
- 8,022
- Reaction score
- 2,816
- Points
- 5,251
- Attending Physician
Fair enough. But as you probably already know, when I ask a question I'm usually just trying to get your POV. If I don't know the answer then I look it up.Onset is 10ish minutes with a duration of 2-4 hours depending on which article you read which works out just about perfect for what I'm hoping to get out of it. I think it also lets me use a lower bupi dose which cuts down on motor block and therefore PACU times. One of our orthopods does anterior total hips and routinely takes 3-3.5 hours and my approach keeps pts comfy for the duration even though I know the Bupi is wearing off by the end.
Like I said though, its non-essential and I could easily do without, but I like the results I get and my PACU nurses like it too. Your mileage may vary.
In this case, I only use fentanyl in spinals for c/s when there is was an epidural in place and I pulled it for a spinal. I add it in this case because, as you pointed out, I can cut down the local dose. But I don't like how they start to itch at about 30 min. I also doubt the 2-4 hr duration but admittedly don't monitor it for that long.
The 10min onset of the isobaric bupiv is exactly what I see which means that the onset is slower than hyperbaric.
- Joined
- May 19, 2008
- Messages
- 349
- Reaction score
- 112
- Points
- 4,691
- Location
- Houston, TX
- Website
- rk.md
- Attending Physician
Spinal vs CSE (~10 mg intrathecal hyperbaric Marcaine with 100 mcg of Duramorph) followed by a continuous adductor canal peripheral nerve block (0.2% ropi plain)