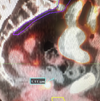
Everyone discussing like it’s a prostate ca recurrence, only. Why so sure. “High grade urothelial ca throughout the bladder,” and a (Gleason 10) prostate cancer. The PSA rose 0.4 over a two year period… this doesn’t match great with a 1.5cm gross pelvic recurrence and an external iliac node does it? What if you bx the node and it’s not prostate cancer? Is that possible even with PSMA positivity?
Gleason 9 and 10 prostate cancers are more likely to be PSA non-producing, or minimally producing, compared to less aggressive histologies. I've seen plenty of low-PSA, high-grade recurrences. PSMA positive certainly can be falsely positive, and has been reported in a variety of cancers, but the most common ones are RCC, lung, and lymphoma. Haven't seen anything about urothelial carcinoma as a false positive on PSMA.
No, I think in the setting of an undetectable PSA after cystoprostatectomy which is now detectable and rising, and hot on PSMA PET, this is prostate cancer until proven otherwise. The PSA / disease volume mismatch is not that surprising given the Gleason 10 histology. I'd be more suspicious about that mismatch it it were a Gleason 7.
If you think you've got a surgeon who can confidently put some kind of spacer in there, then it's a reasonable consideration. I've had conversations like this with various surgeons before and have never gotten anyone to bite, however. YMMV. That loop of bowel is probably adhesed, not surprised prone positioning didn't move the bowel out of the pelvis.
Lacking surgical separation, I would stick a fiducial or two in that nodule for targeting alignment and would be as aggressive as possible with my margins and dosing. I'd also do conventional fractionation to maximize how much dose you can give to the bowel, probably on the order of max dose <57-60 Gy and have a conversation about risk of bowel perforation vs risk of an ugly pelvic recurrence if the disease isn't controlled. And I'd SIB/dose paint as much dose into the GTV as possible while meeting bowel tolerance.
As for the nodes, I'd treat 'em. I'd use 50.4 for the nodal chain and SIB the PET positive node as best as possible. The hardest part is how to define a "prostatectomy bed" since there's no bladder anymore. I'd probably fuse pre-op imaging and draw a prostatectomy bed that covers the original prostate location. Can't go to 70.2 Gy with all the small bowel, so I'd probably limit it to 45 - 50.4 Gy. You're gonna treat a lot of small bowel, there's no way around it. The small bowel DVH will look farily similar to an adjuvant cystectomy plan, if you've ever done one of those. But if he recurs again in the prostatectomy bed after you've done all this radiation he's basically screwed, there is no functional salvage option at that point. So I think the risk reward is in favor of at least covering the prostatectomy bed to a microscopic dose.
Definitely would do dual ADT with a goal of 18 - 24 months. Worth pointing out that SPPORT excluded gleason 10 pts, so in the absence of data supporting stopping at 6 months I'd push for longer. Tough case, good luck!