Winners and Losers
Daniel Merenstein, MD
JAMA. 2004;291(1):15-16. doi:10.1001/jama.291.1.15
There are many losers in this story: the man with incurable prostate cancer, me, my family, family practice residency programs, national guidelines, the shared decision-making model, and anyone who believes in evidence-based medicine (EBM). There were also a few winners: the man with prostate cancer's lawyer, to some extent his family, and anyone who wants to continue to practice outdated medicine or doesn't believe in continuing medical education.
The date was July 19, 1999, when as a third-year resident I saw a highly educated 53-year-old patient. In June 2002, my residency and I were served with court papers. June 2003, the trial.
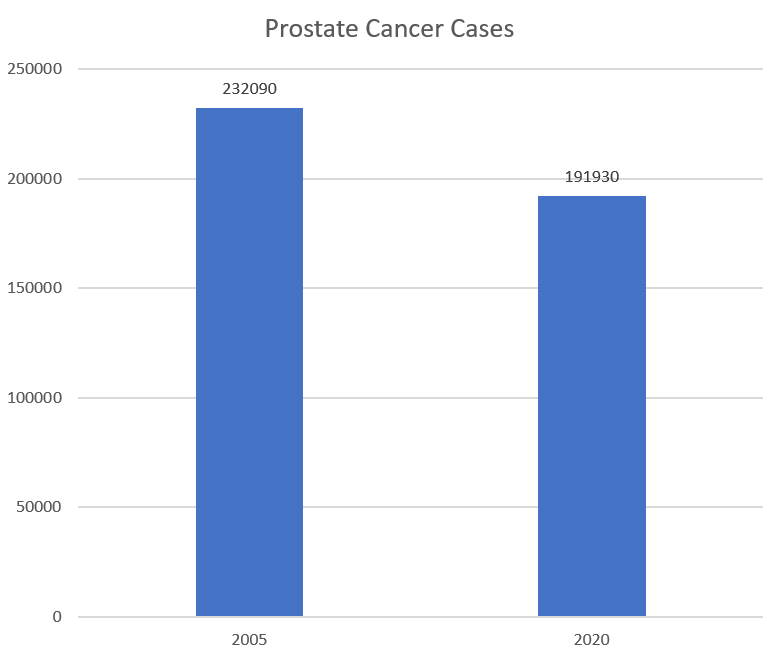
On that day in July 1999 I saw the 53-year-old man for a physical examination. I discussed with him, and documented in his chart, the importance of colon cancer screening, seat belts, dental care, exercise, improved diet, and sunscreen use. I also presented the risks and benefits of screening for prostate cancer and documented the discussion. I never saw the patient again, and after I graduated, he went to another office. His new doctor ordered prostate-specific antigen (PSA) testing without discussing the risks and benefits of screening with him. Unfortunately for the patient, his PSA level was very high and he was subsequently diagnosed with incurable advanced prostate cancer. This patient lost on many accounts. For starters, he had a horrible cancer (Gleason 8), a cancer that is very difficult to treat in any stage and even harder to find early in its course. The literature does not support that early detection would have changed his outcome, although society and many physicians do believe so, thus making the patient live with the false belief that if something had been done differently, he would have survived longer. Clearly, this patient lost the most in this story.
When the trial started on June 23, 2003, I was nervous but confident. I realized that the patient was going to say we had never discussed prostate cancer screening but since I always do and had documented it, I didn't think this would be a very strong plaintiff argument. What I didn't anticipate was that the plaintiff's attorney was going to argue that I should have never discussed the risks and benefits and should have just ordered the PSA. But he did. In fact, a major part of his argument was that there is little risk involved in performing a PSA and that the standard of care is to order the test. Although we had the recommendations from every nationally recognized group supporting my approach and the literature is clear that screening for prostate cancer is controversial, the plaintiff's attorney argued otherwise.
In the medical world it is well accepted that screening for prostate cancer is a risky proposition, in which there is the potential for more harm than good. Nearly all of the national guidelines—including those of the American Academy of Family Physicians, the American Urological Association, and the American Cancer Society—recommend nearly identical approaches a physician should take when it comes to prostate cancer screening. This approach is discussing with the patient the risks and benefits, providing thorough informed consent, and coming to a shared decision. Family medicine has begun to stress the shared decision-making model because of the uncertainty in the literature with regard to such practices as hormone therapy, screening mammography, and many other medical procedures. The shared decision-making model and national guidelines are both losers in this story.
As the trial progressed we presented national experts who discussed the controversy surrounding prostate cancer screening and explained some of the potential dangers of PSA. We discussed such things as false positives, indolent vs aggressive cancers, sensitivity and specificity. Our experts explained that because of the questionable benefit vs associated risks of PSA screening, a shared decision by the physician and the patient was recommended by all of the national health associations. The science was clearly in our favor.
As a family physician I have reveled in keeping up-to-date and providing my patients with the best possible medicine. I have discussed with both patients and colleagues that simply ordering more tests because we have them is not always the best medicine. We have discussed false positives and their implications. The active practitioners who keep up-to-date and stay informed are the losers in this story. During that year before the trial, my patients became possible plaintiffs to me and I no longer discussed the risks and benefits of prostate cancer screening. I ordered more laboratory and radiological tests and simply referred more. My patients and I were the losers.
A major part of the plaintiff's case was that I did not practice the standard of care in the Commonwealth of Virginia. Four physicians testified that when they see male patients older than 50 years, they have no discussion with the patient about prostate cancer screening: they simply do the test. This was a very cogent argument, since in all likelihood more than 50% of physicians do practice this way. One may have argued that we were practicing above the standard of care, but there is no legal precedent for such an argument.
As is well documented in the literature, physicians take quite a long time to change their patients' protocols. Thus, we know that many practicing physicians are not using well-proven interventions or implementing well-publicized national guidelines. The legal definition of standard of care protects these physicians and encourages them to change slowly, if at all. It is often claimed that malpractice is a mechanism for holding physicians accountable and improving the quality of care. This case illustrates quite the opposite: punishing the translation of evidence into practice, impeding improvements to care, and ensconcing practices that hurt patients. In our legal system, the physicians who are slow to change are the winners.
During closing arguments the plaintiff's lawyer put evidence-based medicine on trial. He threw EBM around like a dirty word and named the residency and me as believers in EBM, and our experts as the founders of EBM. He defined EBM as a cost-saving method and stated his belief that the few lives saved were not worth the money. He urged the jury to return a verdict to teach residencies not to send any more residents on the street believing in EBM.
Before this case, I believed that following the current literature and evidence-based medicine was well accepted in medicine and throughout the country. Neither my lawyers nor the judge ever questioned if the plaintiff's attorney could argue against EBM or the national guidelines; the argument was clearly admissible. Sackett and colleagues have generally been given credit for reviving the idea of EBM, which is generally defined as the "conscientious, explicit, and judicious use of current best evidence in making clinical decisions about the care of individual patients."
1 Evidence-based medicine was a loser.
On June 30, 7 days after the trial started, I was exonerated. My residency was found liable for $1 million.
The plaintiff's lawyer was convincing. The jury sent a message to the residency that they didn't believe in evidence-based medicine. They also sent a message that they didn't believe in the national guidelines and they didn't trust the shared decision-making model. The plaintiff's lawyer won.
As I see it, the only way to practice medicine is to keep up with the best available evidence and bring it to my patients.
As I see it, the only way to see patients is by using the shared decision-making model. As I see it, the only way to step into an examination room is to look at a patient as a whole person, not as a potential plaintiff. As I see it, I'm not sure I'll ever want to practice medicine again.
 www.uspreventiveservicestaskforce.org
www.uspreventiveservicestaskforce.org