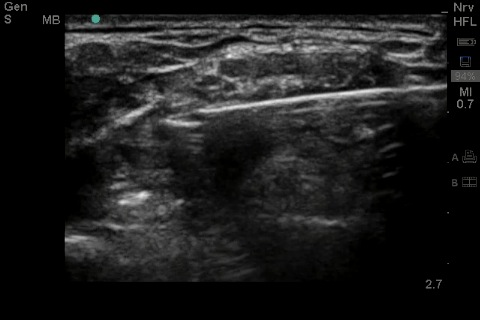
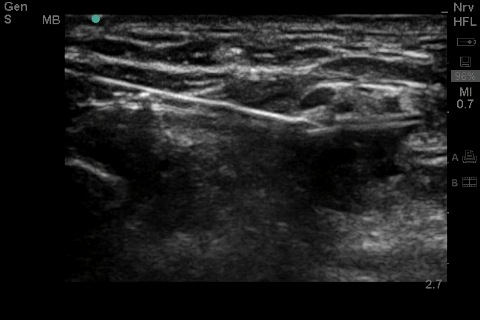
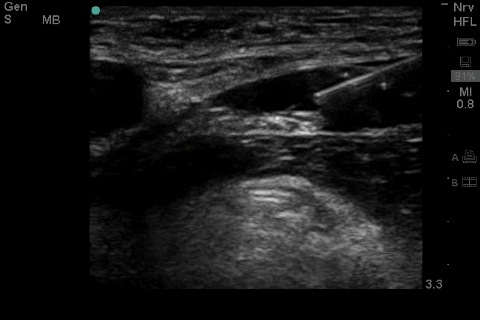
I am going to reawaken this thread as I need some help trouble shooting my central lines. I am an R1 and have done about 15 central lines- mix of IJ, subclavian, femoral. I have gotten to the point that I am pretty good at hitting the vein on my first attempt, but then I run into some problems. My problem is usually threading the wire. Sometimes it will thread about 5-6cm and then meet resistance. At that point I try twist the wire and advance. When that does not work I end up taking out the wire and putting syringe back on and make sure I'm still in vessel. Then repeat with wire. Still wont advance. At that point need to come out with needle and start again. I am not sure what I am doing wrong. Unfortunately we dont have US at my hospital so we are doing the lines based on anatomy. Please help! The residents that I am working with are not experienced enough to help me trouble shoot and sometimes they just take over.
Next time you open a kit in your institution, feed the wire into the needle while you're holding it up and see at what distance the J hook exits the tip of the needle. If your wire gets stuck at 5-6cm, as others have pointed out the tip of the needle may have moved. If you're into the vessel, beyond the tip of the needle and get hung up at 5-6cm it could be due to the direction of your needle bevel placement or the direction your J hook is taking.
If you're right handed and controlling the needle with your left hand, in order to feed the J-hook in the direction that you'd like the catheter to take, you may have to cross your right hand over your left (depending on site), in order to point the J-hook "down" the proper way. The J-hook usually follows the curls of the plastic wire holder for easy reference in most kits I've seen.
Some other issues are:
- Tightening the needle too hard onto the slip tip syringe which requires then additional force when you're trying to detach the needle. This results in you displacing the tip of the needle inadvertently. I always detach and reattach the needle myself so I know exactly how much force I applied. This also enables me to standardize where my bevel is positioned in relation to the numbers on the syringe. I also break the "bond" of the rubber plunger to the plastic sides of the syringe as I do this in order not have any resistance when I'm actually aspirating.
- Pushing the needle further in as you're advancing the wire. I've seen this commonly occur in the excitement of the moment as you push the plastic hub of the wire holder that straightens out the J hook into the opening of the needle and displace your tip as a result.
- Using a bent wire. If you've managed to bend the wire on the last attempt, commonly just after the J-hook, it will thread to a point, then stop. It essentially behaves like central venous obstruction although I find that if I get a fresh wire, I can then pass the wire without a problem.
- Moving the needle as you reach for the wire. I avoid putting any equipment on the patient except for some 4x4s as I've had enough things fall on the floor as people move around. The wire should be relatively accessible. I find that if you grasp the needle with your thumb and index finger this allows you to gently rest your pinky on the patient's skin which will then stabilize your control of the needle. This is particularly important for small vessels.
- Collapsing vessel. Under US you can see a volume depleted person's IJ go from plump to non-existent in the span of a breath. This can result in a scenario where you get stuck at the end of the needle, but not due to movement of the needle, rather due to movement of the vessel. Those people I'll put into Trendelenburg to optimize my chances of success.
- True central obstruction. Rarer, but it does exist and if you're beyond the tip of the wire, have tried a couple/multiple ways at that site, it may be best to convert to the other site on the same side. I usually give myself the opportunity to simply go from the SC to IJ without having to re-prep or re-drape to save time.
See if your institution will invest in an ultrasound. For non-emergent lines it really should be standard of care, particularly for inexperienced operators.