You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
The proposed CMS alternative payment model has arrived
- Thread starter OTN
- Start date
- Joined
- Jun 28, 2005
- Messages
- 571
- Reaction score
- 406
Site Neutral? It's like Christmas in July folks. Send back the caskets, the specialty might not be dead yet!
- Joined
- Oct 10, 2011
- Messages
- 8,599
- Reaction score
- 10,639
Let's see how much of it holds through an ASTRO challenge.
- Joined
- Oct 6, 2011
- Messages
- 85
- Reaction score
- 88
It means you are getting bundled payments for medicare pts half up front and half at 90 days if you are in one of the randomly selected geographic areas covered by the pilot. Astro and others I'm sure will put out bullet points probably by close of business tomorrow. practically, again if you are in one of the geographic areas, this will be the reality not for 1 - 2 years but for 5 years assuming they don't kill it early due to some issue or another. Other mandatory APMs in past (not in oncology) have been abandoned even before close of pilot period.
- Joined
- Sep 20, 2004
- Messages
- 11,705
- Reaction score
- 11,782
"with modifications"... That stood out to me.
"This afternoon, the Centers for Medicare and Medicaid Services (CMS) released a proposed advanced radiation oncology alternative payment model (RO Model) that intends to allow radiation oncologists to participate in value-based cancer care.
In response to this announcement, ASTRO Chair Paul Harari, MD, FASTRO, released the following statement.
"The Radiation Oncology (RO) Model announced today by the Center for Medicare and Medicaid Innovation (the Innovation Center) is a step forward in allowing the nation's 4,500 radiation oncologists to participate in the transition to value-based care that improves outcomes for cancer patients. We believe that once implemented with modifications, the model will incentivize higher quality, more convenient radiation treatments for patients and support their journey toward a cure.
We look forward to providing comments on the specifics of the model, including requirements for certain radiation oncology groups to participate. In our comments to CMS, ASTRO will prioritize recommendations that achieve our longstanding payment reform goals, including stable and fair payments accompanied by incentives for higher quality care and lower costs. In addition, ASTRO will look closely for opportunities to ensure the model is consistent with the Administration's initiative to reduce physician burden and paperwork.
ASTRO has worked for many years to craft a viable payment model that would stabilize payments, drive adherence to nationally-recognized clinical guidelines and improve patient care. We appreciate the Administration's focus and commitment to ensuring radiation oncologists' ability to participate in an advanced APM."
ASTRO staff will continue to review the potential implications from the proposed RO-APM and will notify members of its findings in the next few days. For more details, view CMS's Fact Sheet. View the proposed rule."
"This afternoon, the Centers for Medicare and Medicaid Services (CMS) released a proposed advanced radiation oncology alternative payment model (RO Model) that intends to allow radiation oncologists to participate in value-based cancer care.
In response to this announcement, ASTRO Chair Paul Harari, MD, FASTRO, released the following statement.
"The Radiation Oncology (RO) Model announced today by the Center for Medicare and Medicaid Innovation (the Innovation Center) is a step forward in allowing the nation's 4,500 radiation oncologists to participate in the transition to value-based care that improves outcomes for cancer patients. We believe that once implemented with modifications, the model will incentivize higher quality, more convenient radiation treatments for patients and support their journey toward a cure.
We look forward to providing comments on the specifics of the model, including requirements for certain radiation oncology groups to participate. In our comments to CMS, ASTRO will prioritize recommendations that achieve our longstanding payment reform goals, including stable and fair payments accompanied by incentives for higher quality care and lower costs. In addition, ASTRO will look closely for opportunities to ensure the model is consistent with the Administration's initiative to reduce physician burden and paperwork.
ASTRO has worked for many years to craft a viable payment model that would stabilize payments, drive adherence to nationally-recognized clinical guidelines and improve patient care. We appreciate the Administration's focus and commitment to ensuring radiation oncologists' ability to participate in an advanced APM."
ASTRO staff will continue to review the potential implications from the proposed RO-APM and will notify members of its findings in the next few days. For more details, view CMS's Fact Sheet. View the proposed rule."
- Joined
- Mar 20, 2013
- Messages
- 1,902
- Reaction score
- 3,480
I haven't looked deeply, but there are some weird exemptions (Vermont and Maryland excluded).
I also see that of course the PPS-exempt hospitals keep their exemptions.
If you're a proton center treating prostates and you're in included in this roll out that's going to really really hurt I'd imagine, as I *think* from reading this the baseline formula for what they're going to pay is largely based upon a national average....
Looking forward to seeing people smarter than I evaluate this and find the interesting tidbits in there. Will be nice to see ASTRO take and takes from others out there.
I also see that of course the PPS-exempt hospitals keep their exemptions.
If you're a proton center treating prostates and you're in included in this roll out that's going to really really hurt I'd imagine, as I *think* from reading this the baseline formula for what they're going to pay is largely based upon a national average....
Looking forward to seeing people smarter than I evaluate this and find the interesting tidbits in there. Will be nice to see ASTRO take and takes from others out there.
- Joined
- Jun 18, 2015
- Messages
- 577
- Reaction score
- 679
First thing I saw as well. I'm sure there will be fierce pushback against it, but if it gets though, that's huge.
Those of us who support site neutral payments should contact ASTRO ASAP to let them know we want that provision to stay in the APM. You know the hospitals will be doing it so we need to combat that
More to come and so glad this is now finally ready for review. Interestingly, the national base rates are based on the hospital outpatient payment system (HOPPS APCs) as they found the freestanding rates to be more costly per episode than the HOPPS due to high fractionation use and less stable across the episodes. Lots for us to read and analyze here.
Interested to see how the physician presence requirement will be impacted by bundled payments...Right now, you can get dinged on a per claim basis, but how would that work with what essentially appears to be a case rate??
- Joined
- Feb 28, 2018
- Messages
- 82
- Reaction score
- 113
I had the same question! And wonder how it affects documentation/standard billing requirements. "RO participants would be required to submit encounter data (no-pay) claims that include all RT services identified on the RO Model Bundled HCPCS list (Table 2) as services are furnished and would otherwise be billed under the Medicare FFS system"...but could you not do a weekly status check the first week for a patient getting 6-8 weeks of prostate radiation? Could you not document each SBRT fraction? Could you just write a 1 line simulation note (instead of having to document each treatment device you used) and all the other stuff that doesn't clinically make a difference?Interested to see how the physician presence requirement will be impacted by bundled payments...Right now, you can get dinged on a per claim basis, but how would that work with what essentially appears to be a case rate??
Attachments
- Joined
- Dec 18, 2015
- Messages
- 3,216
- Reaction score
- 4,930
Interested to see how the physician presence requirement will be impacted by bundled payments...Right now, you can get dinged on a per claim basis, but how would that work with what essentially appears to be a case rate??
Me too. I believe it would eliminate the silly kabuki theatre of "stand here... sign here... document here" at least. Chemo, which is way more dangerous/unsafe/lethal than radiotherapy even w/ SRS or SBRT at & during the moment of delivery, can be supervised by just an NP or PA in freestanding. Many big companies have been pushing for freestanding RT NP/PA supervision for a while. I also foresee the rise of, and allowance by CMS for, the rad onc "Virtualist." As we all know the rad onc has zero at-the-moment-of-delivery interaction/oversight of routine radiotherapy fractions... consults could be virtual, planning virtual, film checks virtual, even SRS/SBRT virtual. If just one of these three happen (less supervision/documentation requirements with APM, or NP supervision, or the "virtualist") there'd be need for ~1/3 less rad oncs perhaps (in the US; many other countries do not have the supervision requirement). (I expect and am fully not joking that after we have sufficiently de-fractionated there'll be randomized trials testing the elimination of weekly treatment management and its impact on outcomes. This would provide further cost savings with no impact clinically, I'm sure of it.)I had the same question! And wonder how it affects documentation/standard billing requirements. "RO participants would be required to submit encounter data (no-pay) claims that include all RT services identified on the RO Model Bundled HCPCS list (Table 2) as services are furnished and would otherwise be billed under the Medicare FFS system"...but could you not do a weekly status check the first week for a patient getting 6-8 weeks of prostate radiation? Could you not document each SBRT fraction? Could you just write a 1 line simulation note* (instead of having to document each treatment device you used) and all the other stuff that doesn't clinically make a difference?
*technically in the vast majority of situations one should not be billing for a simulation... ever... so I have already dropped the documentation burden for this quite a bit. Also, when making tx devices, it's been my understanding only one should be billed no matter how many used; documentation shouldn't be overburdensome there either.
Last edited:
- Joined
- Mar 20, 2013
- Messages
- 1,902
- Reaction score
- 3,480
Is staging taken into account at all or is this based on ICD-10 codes?
For instance, for a stage I lung SBRT or a stage III IMRT/VMAT case they both often have the same ICD 10 codes, but payment/treatment here can vary wildly.
Or a stage I right sided breast may be treated with 15 fraction 3D plan, but with a locally advanced stage III you may be looking at 33 fraction breath hold 3D (or IMRT). Both may have the same ICD 10 code. Costs vary wildly. I guess it'll all wash out in theory and you'd get paid "more" on the stage I cases but less on the stage III cases based on current billing standards.
Any thoughts here?
For instance, for a stage I lung SBRT or a stage III IMRT/VMAT case they both often have the same ICD 10 codes, but payment/treatment here can vary wildly.
Or a stage I right sided breast may be treated with 15 fraction 3D plan, but with a locally advanced stage III you may be looking at 33 fraction breath hold 3D (or IMRT). Both may have the same ICD 10 code. Costs vary wildly. I guess it'll all wash out in theory and you'd get paid "more" on the stage I cases but less on the stage III cases based on current billing standards.
Any thoughts here?
- Joined
- Jun 28, 2005
- Messages
- 571
- Reaction score
- 406
If you're a proton center treating prostates and you're in included in this roll out that's going to really really hurt I'd imagine, as I *think* from reading this the baseline formula for what they're going to pay is largely based upon a national average....
My assumption is proton centers will be exempt...
- Joined
- Dec 18, 2015
- Messages
- 3,216
- Reaction score
- 4,930
Well the breast and lung wouldn't have same ICD codes. You mean CPTs? For that, in general, re: payment, 30 fraction IG-IMRT> 30 fraction 3d-IGRT > 15 fx IMRT (which could be used for 100% of early breast, see UK-IMPORT LOW and Evicore guidelines) >15 fx 3d-IGRT > SBRT. I'd predict, but who knows, there's going to be relative equality per clinical scenario. But what it may do is lead to hypofractionating Stage III lung e.g. (why not 2.1 Gy per day guys?) and treating all Stage I breast with five fractions. Maybe suddenly a big single electron dose to the tumor cavity looks appealing. IMHO. All would pay same: 33 fx, or 15 fx, or IMRT, or 3D, or partial breast. And another thing it will do: vastly decrease the number of on-beam patients in all depts across the United States.Is staging taken into account at all or is this based on ICD-10 codes?
For instance, for a stage I lung SBRT or a stage III IMRT/VMAT case they both often have the same ICD 10 codes, but payment/treatment here can vary wildly.
Or a stage I right sided breast may be treated with 15 fraction 3D plan, but with a locally advanced stage III you may be looking at 33 fraction breath hold 3D (or IMRT). Both may have the same ICD 10 code. Costs vary wildly. I guess it'll all wash out in theory and you'd get paid "more" on the stage I cases but less on the stage III cases based on current billing standards.
Any thoughts here?
- Joined
- Mar 20, 2013
- Messages
- 1,902
- Reaction score
- 3,480
Well the breast and lung wouldn't have same ICD codes. You mean CPTs? For that, in general, re: payment, 30 fraction IG-IMRT> 30 fraction 3d-IGRT > 15 fx IMRT (which could be used for 100% of early breast, see UK-IMPORT LOW and Evicore guidelines) >15 fx 3d-IGRT > SBRT. I'd predict, but who knows, there's going to be relative equality per clinical scenario. But what it may do is lead to hypofractionating Stage III lung e.g. (why not 2.1 Gy per day guys?) and treating all Stage I breast with five fractions. Maybe suddenly a big single electron dose to the tumor cavity looks appealing. IMHO. All would pay same: 33 fx, or 15 fx, or IMRT, or 3D, or partial breast. And another thing it will do: vastly decrease the number of on-beam patients in all depts across the United States.
I now see the base formula rates are buried in the proposal. They make no distinction for stage. It literally just says Breast - professional fee $X.
Plus, correct me if I"m wrong, but if you have RUL lung tumor stage I, but a RUL lung tumor with mediastinal nodes, the ICD 10 code is still c34.11, no?
- Joined
- Jun 18, 2015
- Messages
- 577
- Reaction score
- 679
My assumption is proton centers will be exempt...
Why do you say that?
- Joined
- Sep 20, 2004
- Messages
- 11,705
- Reaction score
- 11,782
That will probably be one of ASTROs proposed "modifications" to the planMy assumption is proton centers will be exempt...
- Joined
- Dec 18, 2015
- Messages
- 3,216
- Reaction score
- 4,930
i think so; last time I checked, no way to code for stageI now see the base formula rates are buried in the proposal. They make no distinction for stage. It literally just says Breast - professional fee $X.
Plus, correct me if I"m wrong, but if you have RUL lung tumor stage I, but a RUL lung tumor with mediastinal nodes, the ICD 10 code is still c34.11, no?
- Joined
- Sep 20, 2004
- Messages
- 11,705
- Reaction score
- 11,782
Could use overlapping lung code for locally advanced patientsI now see the base formula rates are buried in the proposal. They make no distinction for stage. It literally just says Breast - professional fee $X.
Plus, correct me if I"m wrong, but if you have RUL lung tumor stage I, but a RUL lung tumor with mediastinal nodes, the ICD 10 code is still c34.11, no?
- Joined
- Mar 20, 2013
- Messages
- 1,902
- Reaction score
- 3,480
That will probably be one of ASTROs proposed "modifications" to the plan
This is what I think may happen too. Though some chunk of the proton centers will be exempt from all of this anyway
- Joined
- Jun 28, 2005
- Messages
- 571
- Reaction score
- 406
Why do you say that?
There was discussion of it when the proposals were being drafted.
- Joined
- Dec 18, 2015
- Messages
- 3,216
- Reaction score
- 4,930
This is what I think may happen too. Though some chunk of the proton centers will be exempt from all of this anyway
If ASTRO pushes for proton centers to be exempt, well then it should be fairly obvious to all that the emperor truly has no clothes.
Site Neutrality: Under Medicare Fee-For-Service (FFS), RT services furnished in a freestanding radiation therapy center are paid under the Medicare Physician Fee Schedule (PFS) at the non-facility rate including payment for the professional and technical aspects of the services. For RT services furnished in an outpatient department of a hospital, the facility services are paid under the Hospital Outpatient Prospective Payment System (OPPS) and the professional services are paid under the PFS. These payment systems determine payment rates for the same services in different ways, which creates site-of-service payment differentials. This difference in payment rate may incentivize Medicare providers and suppliers to deliver RT services in one setting over another, even though the actual treatment and care received by Medicare beneficiaries for a given modality is the same in both settings.
It will be a far bigger bully batting away at this proposal than ASTRO. Hospital lobbyists (which would represent academic centers too obv) will not let "facility fee" incentivization go away without a fight. At this point I can't tell if ASTRO is altruistic, greedy, or just plain dumb, so it's tough to predict on which side of this they'll come down.
- Joined
- May 7, 2014
- Messages
- 1,651
- Reaction score
- 3,461
Quoting verbatim-
"Our analysis also showed that, on average, freestanding radiation therapy centers furnished (and billed for) a higher volume of RT services within such episodes than did HOPDs. Based on our analysis of Medicare FFS claims data from that time period, episodes of care in which RT was furnished at a freestanding radiation therapy center were, on average, paid approximately $1,800 (or 11 percent) more by Medicare than those episodes of care where RT was furnished at a HOPD. We are not aware of any clinical rationale that explains for these differences, which persisted after controlling for diagnosis, patient case mix (to the extent possible using data available in claims), geography, and other factors. These differences also persist even though Medicare payments are lower per unit in freestanding radiation therapy centers than in HOPDs. Upon further analysis, we observed that freestanding radiation therapy centers use more IMRT, a type of RT associated with higher Medicare payments, and perform more fractions (that is, more RT treatments) than HOPDs."
"Our analysis also showed that, on average, freestanding radiation therapy centers furnished (and billed for) a higher volume of RT services within such episodes than did HOPDs. Based on our analysis of Medicare FFS claims data from that time period, episodes of care in which RT was furnished at a freestanding radiation therapy center were, on average, paid approximately $1,800 (or 11 percent) more by Medicare than those episodes of care where RT was furnished at a HOPD. We are not aware of any clinical rationale that explains for these differences, which persisted after controlling for diagnosis, patient case mix (to the extent possible using data available in claims), geography, and other factors. These differences also persist even though Medicare payments are lower per unit in freestanding radiation therapy centers than in HOPDs. Upon further analysis, we observed that freestanding radiation therapy centers use more IMRT, a type of RT associated with higher Medicare payments, and perform more fractions (that is, more RT treatments) than HOPDs."
- Joined
- Sep 20, 2004
- Messages
- 11,705
- Reaction score
- 11,782
Those of us following data and guidelines welcome CMS's push to curtail 40/20 to bone mets and 60/33 to 70+ y/o early stage breast caQuoting verbatim-
"Our analysis also showed that, on average, freestanding radiation therapy centers furnished (and billed for) a higher volume of RT services within such episodes than did HOPDs. Based on our analysis of Medicare FFS claims data from that time period, episodes of care in which RT was furnished at a freestanding radiation therapy center were, on average, paid approximately $1,800 (or 11 percent) more by Medicare than those episodes of care where RT was furnished at a HOPD. We are not aware of any clinical rationale that explains for these differences, which persisted after controlling for diagnosis, patient case mix (to the extent possible using data available in claims), geography, and other factors. These differences also persist even though Medicare payments are lower per unit in freestanding radiation therapy centers than in HOPDs. Upon further analysis, we observed that freestanding radiation therapy centers use more IMRT, a type of RT associated with higher Medicare payments, and perform more fractions (that is, more RT treatments) than HOPDs."
- Joined
- Mar 4, 2019
- Messages
- 55
- Reaction score
- 133
I haven't looked deeply, but there are some weird exemptions (Vermont and Maryland excluded).
I believe these states already have alternative payment models.
- Joined
- Oct 6, 2011
- Messages
- 85
- Reaction score
- 88
Your belief regarding VT and MD is in fact correct. Also for those scoring at home, proton therapy is included in the standard bundle as detailed in the released/proposed rule. Where it ends up at the end of the comment period, nobody knows.
If you’ve been treating appropriately in freestanding centers, site parity via HOPPS will be great. I hypofractionate nearly all my intact breast patients, very, very rarely go above 30 in 10 for mets, and see almost no prostate patients (thanks urorads), so this has real potential to be good for my practice.
- Joined
- Oct 6, 2011
- Messages
- 85
- Reaction score
- 88
from ASTRO summary of RO APM that if not already released publicly to membership will be imminently:
"Included Modalities
CMS proposes to include all modalities of treatment, including external beam therapy: threedimensional
conformal radiotherapy, intensity-modulated radiotherapy, stereotactic radiosurgery,
stereotactic body radiotherapy, and proton beam therapy; intraoperative radiotherapy; image guided
radiation therapy; and brachytherapy.
CMS is considering excluding proton beam therapy from the included modalities in instances where a
beneficiary is participating in a federally funded, multi-institutional, randomized control clinical trial for
proton beam therapy so that further clinical evidence assessing its health benefit comparable to other
modalities can be gathered.
Site Neutral Test
The RO Model proposal includes a “site neutral test” that would establish a common payment amount
for services regardless of where they are furnished. The Agency believes this would offer RO
participants more certainty regarding the pricing of radiation therapy services and remove incentives to
promote the provision of radiation therapy services at one site over another. Since the HHS Secretary
does not have the authority to adjust payments outside of the established MPFS and HOPPS payment
methodologies, this test would only be applicable to RO Model participants."
"Included Modalities
CMS proposes to include all modalities of treatment, including external beam therapy: threedimensional
conformal radiotherapy, intensity-modulated radiotherapy, stereotactic radiosurgery,
stereotactic body radiotherapy, and proton beam therapy; intraoperative radiotherapy; image guided
radiation therapy; and brachytherapy.
CMS is considering excluding proton beam therapy from the included modalities in instances where a
beneficiary is participating in a federally funded, multi-institutional, randomized control clinical trial for
proton beam therapy so that further clinical evidence assessing its health benefit comparable to other
modalities can be gathered.
Site Neutral Test
The RO Model proposal includes a “site neutral test” that would establish a common payment amount
for services regardless of where they are furnished. The Agency believes this would offer RO
participants more certainty regarding the pricing of radiation therapy services and remove incentives to
promote the provision of radiation therapy services at one site over another. Since the HHS Secretary
does not have the authority to adjust payments outside of the established MPFS and HOPPS payment
methodologies, this test would only be applicable to RO Model participants."
- Joined
- Feb 8, 2008
- Messages
- 311
- Reaction score
- 447
Agree entirely. For those of us who have adopted hypofractionation and treat reasonably, this could well represent a pay bump. Not as good of news for those that are treating bone mets with 1.8's...If you’ve been treating appropriately in freestanding centers, site parity via HOPPS will be great. I hypofractionate nearly all my intact breast patients, very, very rarely go above 30 in 10 for mets, and see almost no prostate patients (thanks urorads), so this has real potential to be good for my practice.
- Joined
- Mar 20, 2013
- Messages
- 1,902
- Reaction score
- 3,480
If I'm reading this correctly, the APM is "triggered" at CT sim. So presumably things like prostate/liver/pancreas fiducials or spaceOAR would not bundle into the treatment?
- Joined
- Dec 18, 2015
- Messages
- 3,216
- Reaction score
- 4,930
Random thoughts...
Dr. Harari thinks there are 4500 radiation oncologists in the U.S.:
But in ~2015, ASTRO said there were 5000 radiation oncologists in the U.S... (which personally I think is the right number for ~2014-15, and I feel there are easily 5200-5500 today...)

And there were 186 residency slots ~4 years ago...
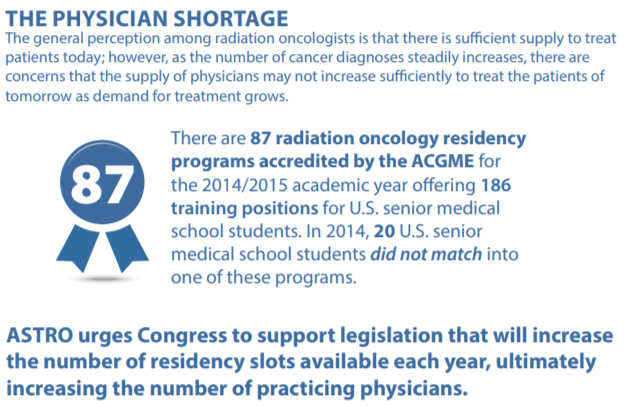
But there are ~211 slots now. Dr. Harari, how did the number of radiation oncologists in the U.S. go down by 500 in 4 years as we are producing ~10% more residents per year, and about 200 residents per year
I blame in some ways ASTRO for all the government attention given to rad onc. They're whiners; they concentrated on this one minor issue because they were butthurt that private practices were doing IMRT for prostate (and the academic centers weren't). Graphics like the below are silly and inflammatory and dog-bites-man in their essence. "Oh goodness someone did something a little questionable; heaven forfend." They shoulda just laid (lied?) low like a two dollar bill like @CarbonIonAngle. Supposedly America's hallowed rad onc residencies were producing radiation oncologists that were going to work in these situations that ASTRO was against (I wasn't one of them, but ASTRO was attacking a lot of its membership when it was attacking Urorads). Rad onc is costing Medicare just a few billion a year. Keytruda itself is costing CMS more than all of rad onc does. Perspective is important.

Dr. Harari thinks there are 4500 radiation oncologists in the U.S.:
"The Radiation Oncology (RO) Model announced today by the Center for Medicare and Medicaid Innovation (Innovation Center) is a step forward in allowing the nation’s 4,500 radiation oncologists to participate in the transition to value-based care that improves outcomes for cancer patients."
But in ~2015, ASTRO said there were 5000 radiation oncologists in the U.S... (which personally I think is the right number for ~2014-15, and I feel there are easily 5200-5500 today...)

And there were 186 residency slots ~4 years ago...

But there are ~211 slots now. Dr. Harari, how did the number of radiation oncologists in the U.S. go down by 500 in 4 years as we are producing ~10% more residents per year, and about 200 residents per year
I blame in some ways ASTRO for all the government attention given to rad onc. They're whiners; they concentrated on this one minor issue because they were butthurt that private practices were doing IMRT for prostate (and the academic centers weren't). Graphics like the below are silly and inflammatory and dog-bites-man in their essence. "Oh goodness someone did something a little questionable; heaven forfend." They shoulda just laid (lied?) low like a two dollar bill like @CarbonIonAngle. Supposedly America's hallowed rad onc residencies were producing radiation oncologists that were going to work in these situations that ASTRO was against (I wasn't one of them, but ASTRO was attacking a lot of its membership when it was attacking Urorads). Rad onc is costing Medicare just a few billion a year. Keytruda itself is costing CMS more than all of rad onc does. Perspective is important.

- Joined
- Oct 5, 2013
- Messages
- 812
- Reaction score
- 547
I mean - if you think ASTRO is wrong in 2019 about how many rad oncs there are, then why wouldn't they have also possibly been wrong in 2015 to begin with? Maybe the 4500 number now is more accurate? Would want to see real data on this and not what you or anyone else 'feels' seems right
Also - CMS was ALWAYS going to pay more attention to all fields of medicine as medicine began to cost more and there were easier (digital) ways to track everything - whether or not there was ever a concern about self-referral
Also - CMS was ALWAYS going to pay more attention to all fields of medicine as medicine began to cost more and there were easier (digital) ways to track everything - whether or not there was ever a concern about self-referral
- Joined
- Dec 18, 2015
- Messages
- 3,216
- Reaction score
- 4,930
Choose one, search your feelings: 1) there are less rad oncs today than ~2015, 2) no one can really say if there are more or less rad oncs today than ~2015, or 3) there are more rad oncs today than ~2015. It wasn't the raw number(s) per se; it's the suggestion (unintentional I'm sure) by Harari/ASTRO that there are 10% less rad oncs today than 4 years ago. And if ASTRO can't consistently be on top of the workforce numbers in this day and age, so that they're not a mystery, that's inexcusable. I've tried to get real data before.I mean - if you think ASTRO is wrong in 2019 about how many rad oncs there are, then why wouldn't they have also possibly been wrong in 2015 to begin with? Maybe the 4500 number now is more accurate? Would want to see real data on this and not what you or anyone else 'feels' seems right
Nah, it's not digital tracking. Rad onc's cost to CMS is small. The amount of govt attention it gets is out of proportion to its size in CMS' budget. Public perception and attention matters. R. Kelly went years with no legal problems; once Lifetime did a documentary on him though he now seems destined for a reckoning. A very superficial look at the long view, in my view, would show a rad onc reimbursement explosion ~2000-2010 from IMRT. This got everybody's attention, including, like from this publication, from this guy (who's also this guy), who "tracked" IMRT spending for prostate. There was similar attention in other disease sites. All reasons for the rise in IMRT use were almost always ascribed to avarice; ASTRO's part in that was not zero. Since ~2010, CMS spending for rad onc has been on a downward trend; personally my CMS billing is down ~20% 2019 vs 2013 for about the same patient numbers (many things reimburse less, somethings you don't even get reimbursed at all for anymore, and hypofractionation; the billing/treating landscape is FAR different, and less lucrative, today than just ~6 years ago). At the same time, however, certain entities (large academic centers) are charging multiples of what some other entities are charging for RT (you bet that's tracked). ASTRO is lamenting self-referral and saying "don't do IMRT for breast," but ASTRO gets indignant when proton non-reimbursement is suggested e.g. It's all a stew. I can't point to one thing, and wouldn't. But ASTRO hasn't been a staunch and consistent helper to all its members due to its actions and inactions. I linked this above, but from 7 years ago Dr. Zeitman was saying:Also - CMS was ALWAYS going to pay more attention to all fields of medicine as medicine began to cost more and there were easier (digital) ways to track everything - whether or not there was ever a concern about self-referral
"Dr. Zietman stressed that our current payment system is a larger part of the problem. 'In the United States we currently have what I call ‘code-driven’ clinical practice. In other words, the practice follows the most lucrative reimbursement codes. It’s simply human nature. So our coding structure is certainly one area in which we could save money and, in some instances, deliver more appropriate care.'"*
Unthinking virtue signalling is also human nature, as is a tendency to try and fix things which aren't broken. I don't think (could be wrong) many other specialties are currently publicly angling, or have been actively publicly angling, for reimbursement-reducing coding sea changes along with essentially saying many of its members (those who work in urology practices e.g.) are behaving unethically.
*EDIT: If a code represents the work by the physician, another way to paraphrase this is:
"Dr. Zietman stressed that our current payment system is a larger part of the problem. 'In the United States we currently have what I call [work-driven] clinical practice. In other words, the practice follows [work that gets paid for]. It’s simply human nature. So our coding structure is certainly one area in which we could [pay less for certain work and thereby force] more appropriate care.'"
Last edited:
- Joined
- Jun 18, 2015
- Messages
- 577
- Reaction score
- 679
Good editorial by Brian Kavanagh explaining the reason ASTRO has pushed for an APM, the basic fundamentals, and the importance of unified advocacy to make the APM as favorable as possible to us. We should all be calling ASTRO to express our preferences, and then when ASTRO comes up with an official response to CMS, we should be calling our Congresspeople to advocate as well on our behalf.
https://www.redjournal.org/article/S0360-3016(19)33448-0/pdf
https://www.redjournal.org/article/S0360-3016(19)33448-0/pdf
Quoting verbatim-
"Our analysis also showed that, on average, freestanding radiation therapy centers furnished (and billed for) a higher volume of RT services within such episodes than did HOPDs. Based on our analysis of Medicare FFS claims data from that time period, episodes of care in which RT was furnished at a freestanding radiation therapy center were, on average, paid approximately $1,800 (or 11 percent) more by Medicare than those episodes of care where RT was furnished at a HOPD. We are not aware of any clinical rationale that explains for these differences, which persisted after controlling for diagnosis, patient case mix (to the extent possible using data available in claims), geography, and other factors. These differences also persist even though Medicare payments are lower per unit in freestanding radiation therapy centers than in HOPDs. Upon further analysis, we observed that freestanding radiation therapy centers use more IMRT, a type of RT associated with higher Medicare payments, and perform more fractions (that is, more RT treatments) than HOPDs."
[/QUOTE]
When Medicare takes away financial incentives for overutilization, this is hard data that the job market, propped up by overutilization in freestanding centers,will be further harmed,not that we didn’t know that.
"Our analysis also showed that, on average, freestanding radiation therapy centers furnished (and billed for) a higher volume of RT services within such episodes than did HOPDs. Based on our analysis of Medicare FFS claims data from that time period, episodes of care in which RT was furnished at a freestanding radiation therapy center were, on average, paid approximately $1,800 (or 11 percent) more by Medicare than those episodes of care where RT was furnished at a HOPD. We are not aware of any clinical rationale that explains for these differences, which persisted after controlling for diagnosis, patient case mix (to the extent possible using data available in claims), geography, and other factors. These differences also persist even though Medicare payments are lower per unit in freestanding radiation therapy centers than in HOPDs. Upon further analysis, we observed that freestanding radiation therapy centers use more IMRT, a type of RT associated with higher Medicare payments, and perform more fractions (that is, more RT treatments) than HOPDs."
[/QUOTE]
When Medicare takes away financial incentives for overutilization, this is hard data that the job market, propped up by overutilization in freestanding centers,will be further harmed,not that we didn’t know that.
Last edited:
- Joined
- Dec 18, 2015
- Messages
- 3,216
- Reaction score
- 4,930
The biggest job growth market, by far, in rad onc the last ~15 years has been in academic positions (~2.2-fold increase). This has outmatched the percent growth in resident slots (~1.6-fold increase). And this has outmatched the growth in private practice jobs (~1.3 fold increase). So freestanding/private practice has been doing all the overbilling, but academics has been able to afford a >200% increase in jobs? C'mon CMS. Everyone should easily see where the real money's been flowing (facility fees? special treatment?). The freestanding centers will either close (small ones especially) or simply not hire to increase ranks for a very long time. The latter has been happening for a while. So I predict, just by looking at the trends, the real job market contraction will be in academics. This will put a major monkeywrench in future job seekers' plans as this, "academics" (academic satellites etc.), has been the "absorber" of all the new rad oncs. Recent ASTRO workforce data back this supposition up: academic jobs growing at the expense of private practice.When Medicare takes away financial incentives for overutilization, this is hard data that the job market, propped up by overutilization in freestanding centers,will be further harmed,not that we didn’t know that.
Last edited:
Moderator note: the post previously referenced here was removed for trolling.
What kind of person goes on to a radiation oncology board to directly talk trash about the specialty?
Last edited by a moderator:
- Joined
- Oct 5, 2013
- Messages
- 812
- Reaction score
- 547
A known troll? He and one other poster that doesn’t need to be named are known trolls. You engage at your own risk.
- Joined
- Oct 5, 2013
- Messages
- 812
- Reaction score
- 547
The biggest job growth market, by far, in rad onc the last ~15 years has been in academic positions (~2.2-fold increase). This has outmatched the percent growth in resident slots (~1.6-fold increase). And this has outmatched the growth in private practice jobs (~1.3 fold increase). So freestanding/private practice has been doing all the overbilling, but academics has been able to afford a >200% increase in jobs? C'mon CMS. Everyone should easily see where the real money's been flowing (facility fees? special treatment?). The freestanding centers will either close (small ones especially) or simply not hire to increase ranks for a very long time. The latter has been happening for a while. So I predict, just by looking at the trends, the real job market contraction will be in academics. This will put a major monkeywrench in future job seekers' plans as this, "academics" (academic satellites etc.), has been the "absorber" of all the new rad oncs. Recent ASTRO workforce data back this supposition up: academic jobs growing at the expense of private practice.
Yes - as has been stated over and over again this is not a rad onc thing but a medicine thing. Hospitals have become corporations and are buying out everything. By definition that makes more ‘academic center’ jobs. Rad onc is not immune nor is Urology, Optho, etc etc etc
- Joined
- Oct 19, 2004
- Messages
- 536
- Reaction score
- 833
Send back the caskets, the specialty might not be dead yet!
PREACH!
D
deleted941485
The biggest job growth market, by far, in rad onc the last ~15 years has been in academic positions (~2.2-fold increase). This has outmatched the percent growth in resident slots (~1.6-fold increase). And this has outmatched the growth in private practice jobs (~1.3 fold increase). So freestanding/private practice has been doing all the overbilling, but academics has been able to afford a >200% increase in jobs? C'mon CMS. Everyone should easily see where the real money's been flowing (facility fees? special treatment?). The freestanding centers will either close (small ones especially) or simply not hire to increase ranks for a very long time. The latter has been happening for a while. So I predict, just by looking at the trends, the real job market contraction will be in academics. This will put a major monkeywrench in future job seekers' plans as this, "academics" (academic satellites etc.), has been the "absorber" of all the new rad oncs. Recent ASTRO workforce data back this supposition up: academic jobs growing at the expense of private practice.
Academic practices especially the ones that have proton facilities are pretty much lining up to shut down any discussion of bundling proton for Medicare patients. Its a joke. That is literally all they care about. It’s helping to prop up a lot of depts. and helps free up their attendings for “academic” work and generate money for the hospital.
A lot of depts are working overtime in building efficiency in their EMR workflow. Automated contouring, Departmental pathway algorithms, etc. it adds up to really less hiring and crappy contracts for the new attendings. And just a crappy job altogether.
In 5 years it’s gonna be basically you literally will click a diagnosis code stage them and the computer will spit out a treatment. If you don’t follow it then you’ll just fill out more paperwork. Which overtime no one will do because it just adds unnecessary time. They will slowly just stop caring.
APMs are gonna end up being just another Paycut to your Dept and ultimately to you. they’re just gonna make their existing workforce pick up the slack and give them the tools to do it.
Your clinical gestalt and experience becomes irrelevant.
- Joined
- Sep 20, 2004
- Messages
- 11,705
- Reaction score
- 11,782
.
APMs are gonna end up being just another Paycut to your Dept and ultimately to you.
Only to those ill prepared for it. Lean, mean, evidence based practice machines will be fine.
There is no reason for different sites of service to be reimbursed differently. A linac is a linac, regardless of location
D
deleted941485
Only to those ill prepared for it. Lean, mean, evidence based practice machines will be fine
Nope...just lean.
- Joined
- Sep 20, 2004
- Messages
- 11,705
- Reaction score
- 11,782
So you think hospitals should get paid more fraction? If so, why?Nope...just lean.
D
deleted941485
So you think hospitals should get paid more fraction? If so, why?
Huh? Did I suggest that?
D
deleted941485
Only to those ill prepared for it. Lean, mean, evidence based practice machines will be fine.
There is no reason for different sites of service to be reimbursed differently. A linac is a linac, regardless of location
Lean practices hire less. Getting leaner makes that worse. APMs will make that even worse. Site neutrality, APM, and proton cuts will literally turn academic centers into just another treatment center. It’s the trifecta of death. I’m not a fan of academic or big hospital Corp but these beasts are pretty much the only ones hiring.
- Joined
- Sep 20, 2004
- Messages
- 11,705
- Reaction score
- 11,782
No but that's what APM is trying to do. It will probably be more of a pay cut if you:Huh? Did I suggest that?
1). Prescribe too many fractions unnecessarily
And/or
2) practice at an expensive site of service.
Not sure how either of those is a "bad" pay cut
