- Joined
- May 3, 2004
- Messages
- 3,441
- Reaction score
- 4,074
Anyone else using these ALTO guidelines for non opioid pain management in your ED? We have a non opioid pain policy with big banners in the ED informing patients and although physicians are technically free to order whatever they think is appropriate, we get emails with the names of physicians who are the biggest offenders with ordering narcotics in the ER so there is definitely pressure to not order them if you can help it. FMD is 100% behind the push for no opioids. At first, I was really excited about the policy and it has definitely made it easier to refuse drugs to the pill heads but incessant pressure to "never order them" has gotten to me recently. I always get rubbed the wrong way when I feel intense pressure to practice a certain way. Sometimes, I feel we're getting so obsessed with non narcotics that it's bordering on lunacy. I mean, check out the ALTO stuff for example:
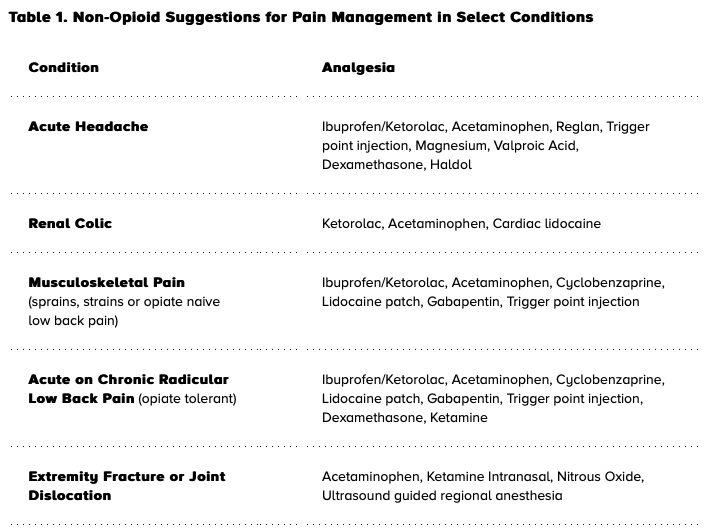
Headache guidelines? Ok, not so bad, though I don't think Haldol would be my first choice to cure someone's headache. How about extremity fracture or joint dislocation. Let's take a femur fracture for instance... Ketamine intranasal? Nitrous?! Are you serious? For the femur fracture and the pt writhing around in the bed in pain, why on earth would I have two techs grab his head and hold him still while I make him snort ketamine? And nitrous?! I can just see myself... "For God's sake, hold him still while I get this Nitrous set up!" For real? Man, give that guy some morphine dammit. I guess my point is that there are still plenty of times where I feel it's completely appropriate to give IV narcotics. Kidney stone? Oh c'mon, add some morphine with that toradol instead of bolusing him with IV lidocaine.
Sometimes, I feel like we've gone so far out into left field with the opioid crisis that we've lost sight of the forest for the trees. IV narcotics are still some of the best ways to manage pain. I'm talking true pain, not the supratentorial BS. I have this one doc who is obsessed with IV ketamine for anyone with pain over 2/10 and I keep thinking to myself...is IV ketamine becoming our "morphine 4mg IV push" of the future? If so, is this really a good idea? I mean...it's ketamine people. For starters, I really hate the dissociative jazz that these pt's go through as soon as you bolus them an "analgesic" dose. I've got patients that will start swaying, yelling, screaming, talking to dead relatives, it's all very annoying with the nurse looking at me nervously.
And what does everyone do with the SCPC? If you try 100% non-narcotic therapy, they will either sign out AMA and call the hospital complaint line or get admitted for pain control. Every time. Good luck getting them pain controlled and out the door without narcotics. What's more....I can't find any official recommendations for non narcotic therapy in SCD. All guidelines recommend IV narcotics. I also feel like such a dumb ass when I phone up medicine for a SCPC admission who hasn't received any narcotics at all because that's the first thing that gets ordered for them by the hospitalist and hematology. Don't get me wrong, I hate giving these guys IV narcs because we have such a huge population of SCD that has been turned into drug seekers but I still haven't found a great way to manage them in the ED in this "non narcotic world" we seem to have found ourselves in these days.
End rant.
Headache guidelines? Ok, not so bad, though I don't think Haldol would be my first choice to cure someone's headache. How about extremity fracture or joint dislocation. Let's take a femur fracture for instance... Ketamine intranasal? Nitrous?! Are you serious? For the femur fracture and the pt writhing around in the bed in pain, why on earth would I have two techs grab his head and hold him still while I make him snort ketamine? And nitrous?! I can just see myself... "For God's sake, hold him still while I get this Nitrous set up!" For real? Man, give that guy some morphine dammit. I guess my point is that there are still plenty of times where I feel it's completely appropriate to give IV narcotics. Kidney stone? Oh c'mon, add some morphine with that toradol instead of bolusing him with IV lidocaine.
Sometimes, I feel like we've gone so far out into left field with the opioid crisis that we've lost sight of the forest for the trees. IV narcotics are still some of the best ways to manage pain. I'm talking true pain, not the supratentorial BS. I have this one doc who is obsessed with IV ketamine for anyone with pain over 2/10 and I keep thinking to myself...is IV ketamine becoming our "morphine 4mg IV push" of the future? If so, is this really a good idea? I mean...it's ketamine people. For starters, I really hate the dissociative jazz that these pt's go through as soon as you bolus them an "analgesic" dose. I've got patients that will start swaying, yelling, screaming, talking to dead relatives, it's all very annoying with the nurse looking at me nervously.
And what does everyone do with the SCPC? If you try 100% non-narcotic therapy, they will either sign out AMA and call the hospital complaint line or get admitted for pain control. Every time. Good luck getting them pain controlled and out the door without narcotics. What's more....I can't find any official recommendations for non narcotic therapy in SCD. All guidelines recommend IV narcotics. I also feel like such a dumb ass when I phone up medicine for a SCPC admission who hasn't received any narcotics at all because that's the first thing that gets ordered for them by the hospitalist and hematology. Don't get me wrong, I hate giving these guys IV narcs because we have such a huge population of SCD that has been turned into drug seekers but I still haven't found a great way to manage them in the ED in this "non narcotic world" we seem to have found ourselves in these days.
End rant.
Last edited: