- Joined
- Jun 20, 2005
- Messages
- 8,022
- Reaction score
- 2,816
- Points
- 5,251
- Attending Physician
BMI 48 don't got notchPosterior cord infraclav + suprascapular in the notch.
Not what you think. But I haven’t been present on this forum for a few months, so I thought I would post a case.
69yo morbidly obese ( BMI 48) female with severe COPD for a shoulder surgery, RCR.
A little more history reveals chronic paroxysmal A fib with PSVT/RVR yada yada yada
PFT’s show <10% improvement with bronchodilators and nothing that stands out.
Pulm med note states, pt requires 3LMP O2 continuous. Requires up to 6lpm with minimal activity. Crank the canister wide open if she even looks at a treadmill or flight of stairs. She will be evaluated for lung reduction surgery after shoulder surgery. Significant dead space and B upper lobe disfunction ( can’t remember the act terminology now but basically scarred tissue not functioning whatsoever in gas exchange). BMP ShowsCO2=28.
Plan: Extensive debridement and RCR In beachchair position in outpt setting connected to hospital.
Anrsthesia plan?

P word!
Posterior cord infraclav + suprascapular in the notch.
Exactly how I would have done it!Well I did the usual KISS method. Everyone in the group that reviewed the case weighed in and the suggestions were all across the board just as in this thread. None of them right or wrong just a personal preference. We discussed. Bipap over night, ICU bed on standby, Ketafol infusion, block vs no block, and monitoring.
I did a low ISB with 10cc0.5% ropiv with decadron and targeted the C7 root. I watched the spread and tried to keep it from spreading up and anterior to the C5&6 roots (trunks). Due to COVID staffing we have some pretty long turnover times and I was able to watch her for about 30 before surgery. She showed no respiratory compromise at this time. And total block to the digits.
In the OR she desaturated while moving over to the OR table (into the low 80’s). She was unable to lie flat so I sat her up 45 deg to see if she improved. She did and we continued. I then gently induced her with neosynhrone, propofol, and lidocaine. I gave her two or three breaths by mask which was easy and slipped in a #4 LMA. Then we positioned her for surgery. While prepping her shoulder she had that uncorrdinated belly breathing pattern. So I gave a little fentanyl to slow her down a bit and added a little pressure support. She was now easily pulling 500cc TV and maintaining ETCO2 of 35-37. I turned on some SEVO and that was about all I had to do for the case. She woke up supper easy on the table in the beachchair position and moved to the gurney. Off to PACU FOR ABOUT 10 min then phase 2 and home. I’ll admit I’m surprised she did so well. I also couldn’t get the BP cuff to work on her upper arm and had to move it to the forearm so I added neo infusion to keep her forearm cuff pressure at 120/70ish, her baseline was 100/60.
The pt was super excited and the surgeon was as well. He was not stocked to do the case by the way. But said if anesthesia will do it then I will Or something like that. Good surgeon and the case took a little over an hour. The shoulder was totally Crap inside and it was the right thing to do for her in hind sight. It would have been the wrong thing to do if we had hurt her. But the plan was to proceed cautiously and to have support if needed (ie: ICU ETC).
Well I did the usual KISS method. Everyone in the group that reviewed the case weighed in and the suggestions were all across the board just as in this thread. None of them right or wrong just a personal preference. We discussed. Bipap over night, ICU bed on standby, Ketafol infusion, block vs no block, and monitoring.
I did a low ISB with 10cc0.5% ropiv with decadron and targeted the C7 root. I watched the spread and tried to keep it from spreading up and anterior to the C5&6 roots (trunks). Due to COVID staffing we have some pretty long turnover times and I was able to watch her for about 30 before surgery. She showed no respiratory compromise at this time. And total block to the digits.
In the OR she desaturated while moving over to the OR table (into the low 80’s). She was unable to lie flat so I sat her up 45 deg to see if she improved. She did and we continued. I then gently induced her with neosynhrone, propofol, and lidocaine. I gave her two or three breaths by mask which was easy and slipped in a #4 LMA. Then we positioned her for surgery. While prepping her shoulder she had that uncorrdinated belly breathing pattern. So I gave a little fentanyl to slow her down a bit and added a little pressure support. She was now easily pulling 500cc TV and maintaining ETCO2 of 35-37. I turned on some SEVO and that was about all I had to do for the case. She woke up supper easy on the table in the beachchair position and moved to the gurney. Off to PACU FOR ABOUT 10 min then phase 2 and home. I’ll admit I’m surprised she did so well. I also couldn’t get the BP cuff to work on her upper arm and had to move it to the forearm so I added neo infusion to keep her forearm cuff pressure at 120/70ish, her baseline was 100/60.
The pt was super excited and the surgeon was as well. He was not stocked to do the case by the way. But said if anesthesia will do it then I will Or something like that. Good surgeon and the case took a little over an hour. The shoulder was totally Crap inside and it was the right thing to do for her in hind sight. It would have been the wrong thing to do if we had hurt her. But the plan was to proceed cautiously and to have support if needed (ie: ICU ETC).
How often do you ask surgeons to consult palliative rather than proceed with surgery? Haven’t done it before, so wondering how receptive surgeons are to that convo...Hey @Noyac, good to see you posting. Good, challenging case. My thoughts are as follows:
1) she has about a 0% 5 year survival rate. She'll likely never have any sort of quality of life again.
2) She's better suited for a palliative care consult than ortho or thoracic surgery. BMI 48, O2 6LPM with minimal activity? Someone is considering lung reduction surgery? BWahahahhaha
3) my thoughts these days are pulm and cards notes are irrelevant with regard to suitability for surgery/anesthesia. They're signing off on the fact that nothing needs to be done to her heart or lungs right now (though the pulm note is suspicious...).
4) if you're doing her at your ASC geez man, what patients are you taking care of in the big house? Since she can't get out of bed without a flood of oxygen to her face she goes directly to the big house where I am.
5) The plan for pain control is no different than it would be for anyone else. You either block, they have little to no pain, and you don't worry about whatever O2 exchange capacity you've knocked out because you've bargained they can handle it. Or you dont' block, they have pain and get a fair amount of opioids, and you don't worry about whatever O2 exchange capacity you've knocked out because you've bargained they can handle it.
6) In short, I push the surgeon not to do the surgery and have a frank discussion with the patient. I realize most COPDers do fine with GETA, but most of them aren't BMI 48 with O2 flood to face every time they have a bowel movement. I'm pushing for palliative involvement here.
If someone holds a gun to my head we do the following:
1) low volume supraclav (10cc)
2) intubate
3) aline if BP cuff isn't reliable
4) plan to extubate to CPAP or BiPAP but tell patient it's likely she goes to ICU intubated
5) even if she surprises us and flies through she stays overnight in case the block wears off and she requires opioid and more CPAP/BiPAP
Now, tell us you did it with block, nothing else, she was discharged 30 min post op, and climbed Mt Everest later that week. 🙂
Well I did the usual KISS method. Everyone in the group that reviewed the case weighed in and the suggestions were all across the board just as in this thread. None of them right or wrong just a personal preference. We discussed. Bipap over night, ICU bed on standby, Ketafol infusion, block vs no block, and monitoring.
I did a low ISB with 10cc0.5% ropiv with decadron and targeted the C7 root. I watched the spread and tried to keep it from spreading up and anterior to the C5&6 roots (trunks). Due to COVID staffing we have some pretty long turnover times and I was able to watch her for about 30 before surgery. She showed no respiratory compromise at this time. And total block to the digits.
In the OR she desaturated while moving over to the OR table (into the low 80’s). She was unable to lie flat so I sat her up 45 deg to see if she improved. She did and we continued. I then gently induced her with neosynhrone, propofol, and lidocaine. I gave her two or three breaths by mask which was easy and slipped in a #4 LMA. Then we positioned her for surgery. While prepping her shoulder she had that uncorrdinated belly breathing pattern. So I gave a little fentanyl to slow her down a bit and added a little pressure support. She was now easily pulling 500cc TV and maintaining ETCO2 of 35-37. I turned on some SEVO and that was about all I had to do for the case. She woke up supper easy on the table in the beachchair position and moved to the gurney. Off to PACU FOR ABOUT 10 min then phase 2 and home. I’ll admit I’m surprised she did so well. I also couldn’t get the BP cuff to work on her upper arm and had to move it to the forearm so I added neo infusion to keep her forearm cuff pressure at 120/70ish, her baseline was 100/60.
The pt was super excited and the surgeon was as well. He was not stocked to do the case by the way. But said if anesthesia will do it then I will Or something like that. Good surgeon and the case took a little over an hour. The shoulder was totally Crap inside and it was the right thing to do for her in hind sight. It would have been the wrong thing to do if we had hurt her. But the plan was to proceed cautiously and to have support if needed (ie: ICU ETC).
Good oral boards case.
First of all, she will need a detailed preop, including a proper H&P. Btw, what were her baseline O2 sats?
Regional is out given the severe COPD.
She needs a preop echo to possibly catch some serious RV dysfunction/PHTN. I will assume she has both, given the hypoxia. I will also assume the hypoxia is optimized (as in this is not some misdiagnosed CHF). That bicarb is unimpressive for a COPD-er, but it suggests chronic respiratory acidosis. Glad that the scarring is not at the base of the lungs.
She will need an ETT to control her ventilation (to avoid hypoxia/hypercarbia), plus to recruit whatever lung she has left, if needed. Good intraop pain control is also essential (pain also raises the PAP).
She will probably need a preinduction A-line, both because of size and because of PHTN/RV failure. She may need some inodilators/epi for the RV during the case.
IV access may be fun too, especially since she will need one for bolusing and one for pressors.
As rapid induction as her heart can tolerate (easy to say), because she will desat like a rock. Prop, sux, tube. Maintenance with sevoflurane, non-opiate analgesia as much as possible if extubation planned (see below), otherwise usual opiates. Have the surgeon inject local in the joint at the end, ideally exparel.
Definitely not an outpatient surgicenter case. Besides the possible difficult extubation due to her COPD, she will have serious pain control issues (unless exparel). It may be needed to leave her intubated for 2-3 days, less if arthroscopic, unless non-opiates (tylenol, toradol, lidocaine gtt, magnesium, ketamine gtt) are enough for her analgesia. Some opiates may be titrated, too, reversed with Narcan in the RR/sats drop too much.
Probably missed some stuff. Definitely the kind of case worth playing mental ping-pong about with colleagues.
Now tell us how you did it under regional. 😀
I'm curious to know how the consent process went? Like did you advise her that she has a fairly good likelihood of death or that you may end up intubating with a prolonged ICU stay and possibly never getting the tube out? That's something that is kinda glossed over in residency and we don't much training on it, so I'd like to hear how you consent for something like this.
Never in a million years would I put a LMA in this patient. Tube, local from surgeon, some adjuncts, light on the opioids.
How often do you ask surgeons to consult palliative rather than proceed with surgery? Haven’t done it before, so wondering how receptive surgeons are to that convo...
I say if you can isolate the posterior cord without hitting the phrenic then you can probably block the whole plexus without hitting the phrenic, you can block suprascapular with US and infiltrate around the suprascacular artery
We should talk about that. Why I like them for this and why others don’t.Nice job. I am not brave enough to do an LMA though.
I agree but I have done thus for 15 yrs and never had to convert.I'm glad it worked out but wooo boy, this line made me nervous: " I gave her two or three breaths by mask which was easy and slipped in a #4 LMA. Then we positioned her for surgery. While prepping her shoulder she had that uncorrdinated belly breathing pattern. "
Now say the case got started and this belly breathing pattern didn't improve with narcotics, you increase the PSV and now PIP are getting close to 20 cmH2O, TV remains bad, LMA starts leaking, CO2 starts climbing up, PAPs go up, RV starts disliking it and her BP baseline is only 100/60....we are in a world of badness. I really don't like not having my backup plan of putting her on protected airway controlled mechanical ventilation + paralysis.
That’s the academic approach in my opinion.So did the group decide that block with potential for knocking out phrenic nerve is better vs no block and using opiates is better for obese COPDers? I was taught that COPD with home O2 use is kind of a contraindication to interscalene maybe even supraclav block, but like so many things from residency, may not be so black and white...
One person's brave is the next person's foolish.Nice job. I am not brave enough to do an LMA though.
0% chance you bag the phrenic on an ISB.
Could you elaborate. The board answer is there is a 100% chance of phrenology nerve block for interacalene.0% chance you bag the phrenic on an ISB. You could hit all 3 cords, but it won’t add anything for a shoulder. Hitting the suprascap in the notch with U/S is necessary with this approach unless you have a surgeon who is really good about getting it in the field. Used to work with a guy like that.
Could you elaborate on this as well? I don’t understand what advantage an LMA gives you over an ETT, just more risk.We should talk about that. Why I like them for this and why others don’t.

Could you elaborate on this as well? I don’t understand what advantage an LMA gives you over an ETT, just more risk.
The theoretical benefit is the lack of glottic/tracheal instrumentation, aka not poking the beast in someone with reactive airway disease. But as I said earlier you can avoid that by pretreatment with neb, methylpred, touch of opioid. Then achieve nice plane of hemodynamically stable anesthesia masking with volatile, D/L, Ropi LTA (+- lido jelly on cuff etc), then smooth sailing.
Effect of topical ropivacaine on the response to endotracheal tube during emergence from general anesthesia: a prospective randomized double-blind controlled study - PMC
The airway reflex such as cough is common accompanied with severe fluctuations of hemodynamics during emergence. This prospective double-blind randomized controlled trial tested the hypothesis that topical ropivacaine may reduce extubation response ...www.ncbi.nlm.nih.gov
Btw @Noyac when did you start targetting roots with your neurostimulator?
I agree but I have done thus for 15 yrs and never had to convert.
I made sure everything was good before westarted the case. You can always reprep.


There is an ENTIRE thread about that subject. Just search the forum.Could you elaborate on this as well? I don’t understand what advantage an LMA gives you over an ETT, just more risk.
How often do you ask surgeons to consult palliative rather than proceed with surgery? Haven’t done it before, so wondering how receptive surgeons are to that convo...
NEVER lie to your patient. That's dereliction of duty. You have the choice of how you package it, but try to tell her the truth, the whole truth, and nothing but the truth, anytime there is a difficult decision to make. Why? Because you need to manage expectations (beyond the duty to your patient). The best policy is always to be honest. I will use malpractice lawsuits as a proxy for profound patient unhappiness, to illustrate my point.I'm curious to know how the consent process went? Like did you advise her that she has a fairly good likelihood of death or that you may end up intubating with a prolonged ICU stay and possibly never getting the tube out? That's something that is kinda glossed over in residency and we don't much training on it, so I'd like to hear how you consent for something like this.
I would have intubated this patient likely with a glidescope
Why?
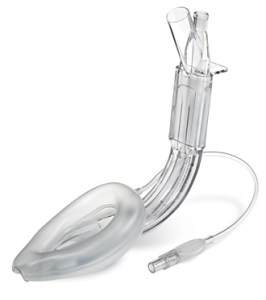
See post number 2 by FFP. I would be willing to try a Supreme LMA size 4 but once I saw the belly breathing the LMA would have likely been changed to an ETT.
Good discussion.
Of note... even if you aim at C6-C7 or lower you can possibly get rostral spread.
This is a block I did today. 20cc’s during a single pass with the needle tip aimed @ C6. Spread is caudal, rostral, anterior and posterior. Doesn’t always spread this way, but it can if it’s a tight sheath with the right hydro dynamics.
View attachment 309889
I sense some concerns. 😵glad it worked out
