You are using an out of date browser. It may not display this or other websites correctly.
You should upgrade or use an alternative browser.
You should upgrade or use an alternative browser.
Tips and Tricks
Started by OB1🤙
How about OB tips?
Difficult epidural?
Best spinal cocktails?
Rescuing patchy epidural during C-section?
Difficult epidural?
Best spinal cocktails?
Rescuing patchy epidural during C-section?
A tip that I learned while doing a nasal intubation with the glidescope is that you can use the glidescope stylet with a regular oral endotracheal tube. You will be able to aim the tube pretty much right into the glottis with the stylet, no need to pull out the magills. The only caveat is that the tube will pretty much be at the hub into the nostril and you will have to secure it carefully.
Advertisement - Members don't see this ad
I like using a FOB and a glidescope together. The glidescope moves soft tissues out if the way and provides a great view while you maneuver the bronchoscope. It's not needed most if the time, but can make a difficult scope much easier.
Is this a two person technique? I've heard about this but never tried it. How exactly do you do it?I like using a FOB and a glidescope together. The glidescope moves soft tissues out if the way and provides a great view while you maneuver the bronchoscope. It's not needed most if the time, but can make a difficult scope much easier.
Place glidescope. Let go. Manipulate your bronchoscope aka navigable stylet.
D
deleted9493
For labor epidurals (especially the obese or those with contorted anatomy), communicate with the patient regarding where they are feeling the tip of your tuohy...to the left or right or not sure. If they aren't sure, you're probably midline. If they are, re-direct accordingly.
I can't find the study that speaks to the increased ease of placement with this simple method but there is data somewhere that speaks to its efficacy.
I can't find the study that speaks to the increased ease of placement with this simple method but there is data somewhere that speaks to its efficacy.
D
deleted162650
For those OB pts with either strage anatomy, or those ones that are in that special range of obesity where you can't feel any landmarks yet they aren't quite soo fat where the rolls drape of the midline, learn to use U/S for epidurals. Use the same U/S machine/probe (large curvilinear) that is on every OB unit in the country. You can find not only an open space/level, but you can also find the depth of the epidural space. Make a couple marks, put away the U/S machine, and proceed as usual. It takes maybe 2 min and saves you 10-15 mins of fishing around with the tuohy.
For those pts with mushburger ligaments/tissues where the LOR isn't very crisp or reassuring, go ahead pass a 26 Gertie Marx or similar through the tuohy like you're doing a CSE when you think you've got LOR.
Get CSF? Awesome, your Tuohy is in the epidural space, proceed as usual (spinal dose optional)
No CSF? False loss, keep going with that Tuohy and try again.
For those pts with mushburger ligaments/tissues where the LOR isn't very crisp or reassuring, go ahead pass a 26 Gertie Marx or similar through the tuohy like you're doing a CSE when you think you've got LOR.
Get CSF? Awesome, your Tuohy is in the epidural space, proceed as usual (spinal dose optional)
No CSF? False loss, keep going with that Tuohy and try again.
Advertisement - Members don't see this ad
A tip that I learned while doing a nasal intubation with the glidescope is that you can use the glidescope stylet with a regular oral endotracheal tube. You will be able to aim the tube pretty much right into the glottis with the stylet, no need to pull out the magills. The only caveat is that the tube will pretty much be at the hub into the nostril and you will have to secure it carefully.
The few occasions I've utilized a Glidescope for a nasal intubation (i.e: changing out an in-the-field orally inserted ETT, for nasal, in a mandible/maxilla fracture patient in c-collar to proceed with OR case), I've used a regular nasal RAE and found that the curvature of the tube itself and feeding from the nasopharynx pretty much directs it straight in (maybe with a little cricoid manipulation) without requiring a stylet.
Honest to god, I don't know how you manage feeding a tube with a J-shaped rigid stylet through the nasopharynx. 😵
On a side note, if one ever encounters a severely anterior glottis while utilizing a Glidescope and find no success with downward displacement via cricoid manipulation, utilizing a malleable stylet bent into a "candy-cane" vs the j-shaped rigid stylet, may get you just enough anterior placement, to then pull the stylet and maneuver the ETT in.
Last edited:
http://tinyurl.com/lwgaft7
Glad u like this technique, I reported it back in 2007 and continue to use it regularly.
One trick I came up with, haven't seen reported, is to verify proper tracheal tube placement without using positive pressure ventilation and risking (over) inflating the stomach: Place tube, connect circuit with pop off fully open, and apply quick sternal compression. If tube in trachea, prompt detectable ETCO2. Works best on kids with flexible chests, not so well on elderly with stiff chest walls. May seem silly but the are lots of reports of overinflated stomach and mucosal tears that have required laparotomy to fix.
Glad u like this technique, I reported it back in 2007 and continue to use it regularly.
One trick I came up with, haven't seen reported, is to verify proper tracheal tube placement without using positive pressure ventilation and risking (over) inflating the stomach: Place tube, connect circuit with pop off fully open, and apply quick sternal compression. If tube in trachea, prompt detectable ETCO2. Works best on kids with flexible chests, not so well on elderly with stiff chest walls. May seem silly but the are lots of reports of overinflated stomach and mucosal tears that have required laparotomy to fix.
Definitely not vital in any way to patient management like these other posts, but if you take one of the pre-filled 10cc NS syringes and pull the plunger backwards, it breaks the seal so you don't have to worry about shooting out part of the contents of the syringe.
Definitely not vital in any way to patient management like these other posts, but if you take one of the pre-filled 10cc NS syringes and pull the plunger backwards, it breaks the seal so you don't have to worry about shooting out part of the contents of the syringe.
This becomes vital when you watch a resident that doesn't know this tip shoot a syringe of saline straight up into the air trying to break the seal, and then subsequently watch said saline hit a video screen/light and drip back down onto their central line tray...
I stand corrected.This becomes vital when you watch a resident that doesn't know this tip shoot a syringe of saline straight up into the air trying to break the seal, and then subsequently watch said saline hit a video screen/light and drip back down onto their central line tray...
D
deleted171991
I pull the seal towards the plunger with my both hands, while holding the tip against my chest or belly. Takes just one second, no spray.
Last edited by a moderator:
This becomes vital when you watch a resident that doesn't know this tip shoot a syringe of saline straight up into the air trying to break the seal, and then subsequently watch said saline hit a video screen/light and drip back down onto their central line tray...
I always get saline from some source while setting up my tray during central line placement but have always wondered if this step is really necessary...if you aspirate blood through all the ports and put a cap on them it shouldn't take more than a couple minutes from that point to dressing the line and then being able to grab saline from an IV (or whatever) and flushing the lines after you have broken sterility. Will the blood really clot up in a couple of minutes assuming they don't have some strange thrombophilia?
The few occasions I've utilized a Glidescope for a nasal intubation (i.e: changing out an in-the-field orally inserted ETT, for nasal, in a mandible/maxilla fracture patient in c-collar to proceed with OR case), I've used a regular nasal RAE and found that the curvature of the tube itself and feeding from the nasopharynx pretty much directs it straight in (maybe with a little cricoid manipulation) without requiring a stylet.
Honest to god, I don't know how you manage feeding a tube with a J-shaped rigid stylet through the nasopharynx. 😵
On a side note, if one ever encounters a severely anterior glottis while utilizing a Glidescope and find no success with downward displacement via cricoid manipulation, utilizing a malleable stylet bent into a "candy-cane" vs the j-shaped rigid stylet, may get you just enough anterior placement, to then pull the stylet and maneuver the ETT in.
I've done a lot of nasal raes, not all of them goes directly through the glottis without outside help like magills, especially head/neck cancer radiation cases or c spine cases.
I wouldn't have mentioned this tip if I thought it was obvious. I say give it a careful try, it may surprise you how easy it is to manipulate a rigid stylet through the nasopharynx after typical dilation/vasoconstrictor/lube.
Advertisement - Members don't see this ad
I always get saline from some source while setting up my tray during central line placement but have always wondered if this step is really necessary...if you aspirate blood through all the ports and put a cap on them it shouldn't take more than a couple minutes from that point to dressing the line and then being able to grab saline from an IV (or whatever) and flushing the lines after you have broken sterility. Will the blood really clot up in a couple of minutes assuming they don't have some strange thrombophilia?
At my shop we routinely place central lines/introducers without priming them with saline and I've never had an issue. Place the line, bleed it back, and then hand off a sterile extension to an assistant who hooks it up to the fluid source and flushes toward you so you can hook it up and flush the blood out of the line. If you're paranoid about the line getting yanked you can suture it in before doing this if you're not too slow with the suturing. You can't dawdle with it because it really does only take a couple minutes for the blood to start clotting, especially if you're putting in a line with smaller diameter ports like a triple lumen.
Last edited:
I always get saline from some source while setting up my tray during central line placement but have always wondered if this step is really necessary...if you aspirate blood through all the ports and put a cap on them it shouldn't take more than a couple minutes from that point to dressing the line and then being able to grab saline from an IV (or whatever) and flushing the lines after you have broken sterility. Will the blood really clot up in a couple of minutes assuming they don't have some strange thrombophilia?
I have one attending who thinks flushing double and triple lumen central lines is silly in the first place.
If you are placing the line with the neck below the level of the heart, I don't see the point of pre-flushing the ports at all.I have one attending who thinks flushing double and triple lumen central lines is silly in the first place.
http://tinyurl.com/lwgaft7
Glad u like this technique, I reported it back in 2007 and continue to use it regularly.
One trick I came up with, haven't seen reported, is to verify proper tracheal tube placement without using positive pressure ventilation and risking (over) inflating the stomach: Place tube, connect circuit with pop off fully open, and apply quick sternal compression. If tube in trachea, prompt detectable ETCO2. Works best on kids with flexible chests, not so well on elderly with stiff chest walls. May seem silly but the are lots of reports of overinflated stomach and mucosal tears that have required laparotomy to fix.
I'm not an anesthesiologist, haven't even started MD school, but I can offer one that I learned while working with experimental pigs:
To determine correct et tube placement, don't inflate the cuff as soon as the tube is placed. Bag patient for 2-3 breaths. If etCO2 shows up, you're good. If not, pull it out and try again.
By not inflating the cuff asap, you prevent over-inflating the stomach. (This is rather important when working with animals where the esophogeal intubation rate is ~50%) Also, if you have to pull the tube multiple times, not inflating the cuff until proper placement is assured will save a bit of time.
I'm not an anesthesiologist, haven't even started MD school, but I can offer one that I learned while working with experimental pigs:
To determine correct et tube placement, don't inflate the cuff as soon as the tube is placed. Bag patient for 2-3 breaths. If etCO2 shows up, you're good. If not, pull it out and try again.
By not inflating the cuff asap, you prevent over-inflating the stomach. (This is rather important when working with animals where the esophogeal intubation rate is ~50%) Also, if you have to pull the tube multiple times, not inflating the cuff until proper placement is assured will save a bit of time.
You can get 2-3 breaths of etco2 from the stomach though. Once you start intubating homo-sapiens and homo-superiors you'll see it's pretty rare that you don't witness it go through the cords...then you're just checking to make sure you didn't mainstem it.
I prefer to intubate with the cuff up because passing it through the cords will help to dilate them...and after extubation they will breath better...resistance is inversely related to r^4.
I always get saline from some source while setting up my tray during central line placement but have always wondered if this step is really necessary...if you aspirate blood through all the ports and put a cap on them it shouldn't take more than a couple minutes from that point to dressing the line and then being able to grab saline from an IV (or whatever) and flushing the lines after you have broken sterility. Will the blood really clot up in a couple of minutes assuming they don't have some strange thrombophilia?
I don't think you have to pre-flush but if you bleed back I always like to flush to prevent it from clotting. You could even use the little vial of lido that comes in the kit to flush if you want, no extraneous flush material required.
I prefer to intubate with the cuff up because passing it through the cords will help to dilate them...and after extubation they will breath better...resistance is inversely related to r^4.
Wait what? <Not sure if serious>
You can get 2-3 breaths of etco2 from the stomach though.
Eh...it appeared 100% accurate when working with Sus domesticus at least.
(Yes, you could get etCO2 from the stomach, but it was always significantly lower than what you 'should' see.)
Advertisement - Members don't see this ad
Eh...it appeared 100% accurate when working with Sus domesticus at least.
(Yes, you could get etCO2 from the stomach, but it was always significantly lower than what you 'should' see.)
Last soda intake..part of pre-op interview.
Some of the gastric ruptures were in kids where uncuffed tubes are usedI'm not an anesthesiologist, haven't even started MD school, but I can offer one that I learned while working with experimental pigs:
To determine correct et tube placement, don't inflate the cuff as soon as the tube is placed. Bag patient for 2-3 breaths. If etCO2 shows up, you're good. If not, pull it out and try again.
By not inflating the cuff asap, you prevent over-inflating the stomach. (This is rather important when working with animals where the esophogeal intubation rate is ~50%) Also, if you have to pull the tube multiple times, not inflating the cuff until proper placement is assured will save a bit of time.
Re: epidurals. Not a trick but a tip for residents. Once you go continuous technique, you won't look back. Easier, faster, slicker, and IMO safer than the "advance, tap tap" technique. Insert needle to some appropriate depth. Attach saline filled syringe WITHOUT any air bubbles. Apply pressure on the syringe plunger to advance. You will get a better tactile feel as you engage ligament, then once you enter epidural space, the saline will be injected epidural and the needle tip will not advance further.
Re: flushing central lines. I never flush before or during line placement, it's a complete waste of time. Just make sure your hubs are on tight and neither blood nor air will go where it shouldn't. Flush after the line is in and skip this unnecessary step.
Re: flushing central lines. I never flush before or during line placement, it's a complete waste of time. Just make sure your hubs are on tight and neither blood nor air will go where it shouldn't. Flush after the line is in and skip this unnecessary step.
Last edited:
Some of the gastric ruptures were in kids where uncuffed tubes are used
Ok.
I can't tell if you're agreeing, disagreeing, or simply tying to add to the discussion, so I will insert this smilie in leeway of actual discussion:

D
deleted87051
This becomes vital when you watch a resident that doesn't know this tip shoot a syringe of saline straight up into the air trying to break the seal, and then subsequently watch said saline hit a video screen/light and drip back down onto their central line tray...
Haha!
When I need flush for a line, I just pull it from the flush port of the transducer that is invariably nearby. I use a 30 ml syringe and squirt it into the tray. No prefilled saline syringes needed.
You can also pull it from the injection port of the patient's IV line. All that fluid ends up in the same place.
This makes no sense.I prefer to intubate with the cuff up because passing it through the cords will help to dilate them...and after extubation they will breath better...resistance is inversely related to r^4.
Please do not do this.
If this were true then why would we deflate the cuff before extubating pts?
Advertisement - Members don't see this ad
This makes no sense.
Please do not do this.
If this were true then why would we deflate the cuff before extubating pts?
Thank you, you've changed my whole outlook on anesthesia.
I a
I should have said, I disagree with this. And would you please explain how this is supposed to work?
I apologize.Thank you, you've changed my whole outlook on anesthesia.
I should have said, I disagree with this. And would you please explain how this is supposed to work?
I a
I apologize.
I should have said, I disagree with this. And would you please explain how this is supposed to work?
I was just messing around. Your reaction was similar to the response I'd get on my pager when i used to suggest we run a mac on .25mg of versed and a sux drip
Or when i'd label my carrier fluid "naloxone" on tiva cases because remi was too strong
Sometimes the only one who finds me funny is...me 🙂
Last edited:
If you hit the goose, LEAVE THE ORIGINAL TUBE IN.
Now you have a conduit for gastric contents to escape without causing aspiration. As a bonus, you know where to NOT put the tube the second time 🙂
Now you have a conduit for gastric contents to escape without causing aspiration. As a bonus, you know where to NOT put the tube the second time 🙂
A tip for facilitating advancement of the ETT in a very anterior glottis (usually with Glidescope). Use a standard satin-slip malleable stylet and bend to the appropriate J-curve (roughly approximating the Glidescope stylet or even more acute angle as required) with the difference being that you 'reverse load.' That is, use the stylet to bend the ETT against the grain of its natural curvature. This way when you get the tip to the glottis and advance ETT/remove stylet you won't have the problem of getting stuck on the anterior commissure or against anterior tracheal wall because the ETT will tend to move posteriorly rather than anteriorly. The other trick of counter-clockwise turns can also help but this can be challenging on a still-styletted ETT.
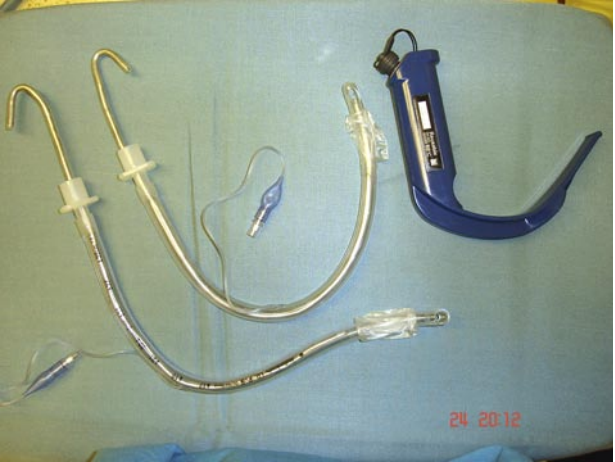
Source: Dow&Parsons, CJA 54:2 2007
Source: Dow&Parsons, CJA 54:2 2007
Last edited:
Sometimes a poorly fitting face mask works better turned upside down.
If the surgeon is likely to use the patients face as an arm rest, put the tube tree under the patients head, not under the mattress. Put it on the surgeons side, almost touching the ear/jaw. It is pokey enough to remind them not to lean on someone's face.
Advertisement - Members don't see this ad
2 liters in the foley bag? Hook the drain nozzle up to your suction and bag is empty in 15 seconds.Everyone has their own little semi-secret tricks. Let's hear what yours are. Maybe this thread will suck, and maybe it'll be great. We'll see.
I'll throw 2 out there.
1) Your pt has very crappy veins, and you need a reasonable IV? Got an ultrasound, found a nice juicy target but it's pretty deep?
The Arrow a-line kit is your friend. You can enter the vein at a pretty steep angle, thread the built-in wire, and voila, 20g IV. Because it's kink-resistant, it'll stay good despite the angle.
2) Have trouble masking, and don't have qualified help? Set your machine to pressure control ventilation, dial the pressure to something reasonable (I use 15), rate about 10. Turn vent on. Now use both hands to hold the mask, and the machine does the "bagging" for you.
Bonus: If the reason you're having trouble is a bushy beard, pop a big Tegaderm over the beard and cut a hole over the mouth. Seal will be much, much better.
Let's hear some more.
When you are doing a nasal intubation, if it is difficult to get the tube through the cords and you need to bmv or reassess (particularly in kids who desat quicker)....
Just leave the tube in, go up on the cuff, connect circuit, pinch the non-tubed nostril and mouth shut (easy w/ 1 hand) and use the tube like an LMA to bag patient back up.
Works better than a mask anyways and you don't have to subject patient to any more ett through the nose trauma.
Just leave the tube in, go up on the cuff, connect circuit, pinch the non-tubed nostril and mouth shut (easy w/ 1 hand) and use the tube like an LMA to bag patient back up.
Works better than a mask anyways and you don't have to subject patient to any more ett through the nose trauma.
When you are doing a nasal intubation, if it is difficult to get the tube through the cords and you need to bmv or reassess (particularly in kids who desat quicker)....
Just leave the tube in, go up on the cuff, connect circuit, pinch the non-tubed nostril and mouth shut (easy w/ 1 hand) and use the tube like an LMA to bag patient back up.
Works better than a mask anyways and you don't have to subject patient to any more ett through the nose trauma.
The only can't ventilate situation I've ever been in was mitigated by that technique. It worked for a few breaths and allowed time to use a bronchoscope to place the ett.
And if it's a difficult airway it won't get any easier with a tube in the mouth... don't like this technique eitherIf you have determined that you intubated the goose, wouldn't you likely need to bag before attempting another DL? I would think leaving the original tube in place would make mask ventilation difficult
The only can't ventilate situation I've ever been in was mitigated by that technique. It worked for a few breaths and allowed time to use a bronchoscope to place the ett.
👍
That's a heck of a save right there.
Along the same lines, sometimes if you are having difficulty (dang thing always gets caught on arytenoids for me), get right in front of the arytenoids, have someone pump 10cc into the cuff, and see if it elevates/centers it to slide the tip past the cords before going down on the cuff and sliding right in. Not 100% successful like the one above but sure looks slick and feels good when you do it.
D
deleted171991
While intubating a difficult airway, use a nasal cannula at high flow for apneic oxygenation.
When your OB asks for hemabate or methergine during a c/s under spinal, give it under the drapes in the thigh. The pt won't feel it and it works faster (theoretically).
I just found out that I'm the only one in my group that does this. I thought everyone did it this way.
I just found out that I'm the only one in my group that does this. I thought everyone did it this way.
D
deleted162650
When your OB asks for hemabate or methergine during a c/s under spinal, give it under the drapes in the thigh.
This is how we do at my place except the circulator actually does the injection.
Advertisement - Members don't see this ad
This thread is one of the reasons I love this job. Keep 'em coming!
One thing I've been coming to love recently is bolusing 100 mcg Fentanyl with my 15-20 mL of 0.125% bupi for initial labor epidural placement. They seem to get comfortable faster than plain 0.125%. Usually give 5-7 ml through the Touhy, thread the catheter, then give the rest in divided doses between taping/repositioning/starting infusion. Some folks here refuse to use Fentanyl as a bolus, citing that will mask a bad catheter. I'm not sure I buy that argument but my N is about 30 using this technique so time will tell.
Need a couple of clarifications:
1. Regarding the tegaderm-over-beard trick, how big are you cutting the mouth hole?
2. I've heard about the 14 gauge angio cath+stopcock+ETT connector trick for crics before, but I'm still unclear as to WHAT TO DO WITH IT. So you have a catheter in the trachea... what do I do? Hook up the circuit to the ETT connector and hand ventilate? Hook it up to the jet ventilator stopcock/Luer lock? How do you move air (i.e. remove CO2) through such a small orifice?
One thing I've been coming to love recently is bolusing 100 mcg Fentanyl with my 15-20 mL of 0.125% bupi for initial labor epidural placement. They seem to get comfortable faster than plain 0.125%. Usually give 5-7 ml through the Touhy, thread the catheter, then give the rest in divided doses between taping/repositioning/starting infusion. Some folks here refuse to use Fentanyl as a bolus, citing that will mask a bad catheter. I'm not sure I buy that argument but my N is about 30 using this technique so time will tell.
Need a couple of clarifications:
1. Regarding the tegaderm-over-beard trick, how big are you cutting the mouth hole?
2. I've heard about the 14 gauge angio cath+stopcock+ETT connector trick for crics before, but I'm still unclear as to WHAT TO DO WITH IT. So you have a catheter in the trachea... what do I do? Hook up the circuit to the ETT connector and hand ventilate? Hook it up to the jet ventilator stopcock/Luer lock? How do you move air (i.e. remove CO2) through such a small orifice?
Jet ventilator. You can't get enough pressure/flow with an ambubag or the machine circuit. Exhalation is passive, once you get the lungs inflated, even if you can't intubate/ventilate from above, a full pair of lungs will still exhale passively through the upper airway. But the extremely low pressure/flow you get with the ambubag/circuit through an angiocath won't get much into the lungs since the low resistance path is up and out. You need to use the jet ventilator. IMO the whole angiocath + 3cc syringe + ETT connector is mystic MacGyverish lore dogma and should die. If you ever get a chance to do a cadaver lab try it both ways. Low pressure/flow through an angiocath Doesn't Work.2. I've heard about the 14 gauge angio cath+stopcock+ETT connector trick for crics before, but I'm still unclear as to WHAT TO DO WITH IT. So you have a catheter in the trachea... what do I do? Hook up the circuit to the ETT connector and hand ventilate? Hook it up to the jet ventilator stopcock/Luer lock? How do you move air (i.e. remove CO2) through such a small orifice?
I suppose if you sealed the mouth/nose while ambubaging an angiocath you might get a tiny amount of O2 into the lungs and that's better than nothing, but you're far better off just using the jet ventilator on the machine.

