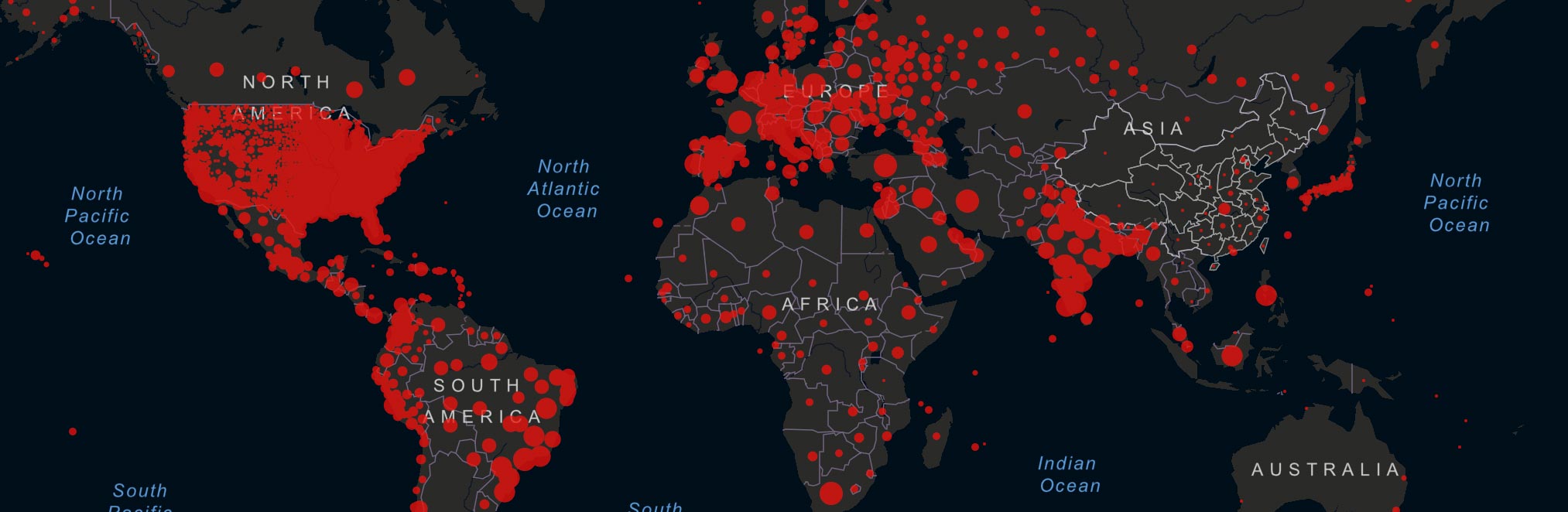
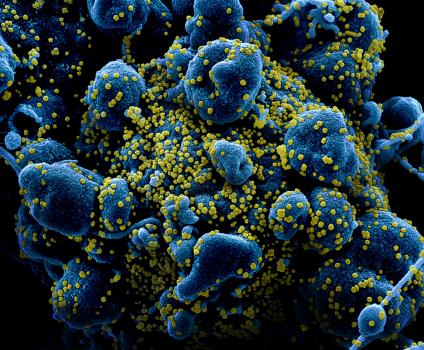
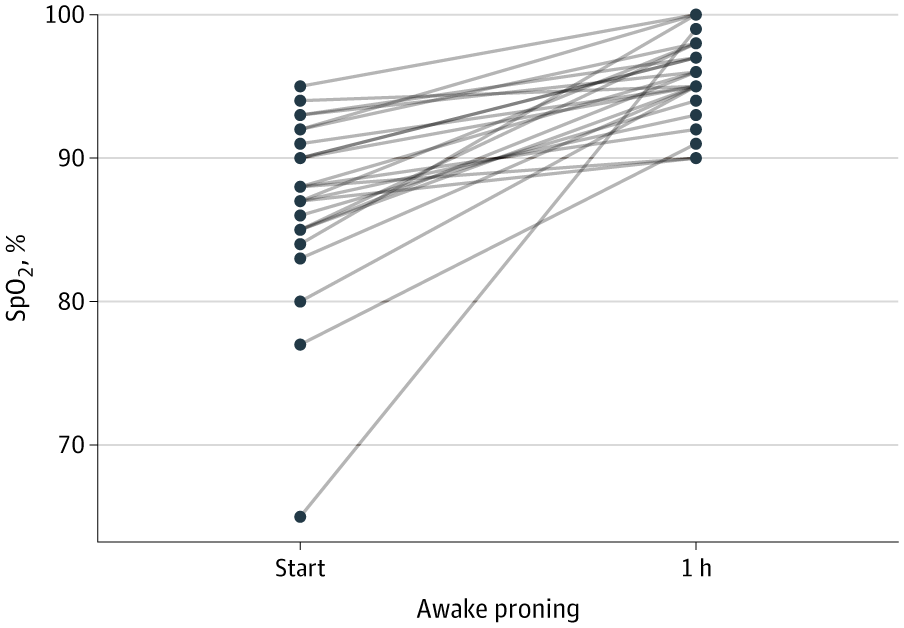
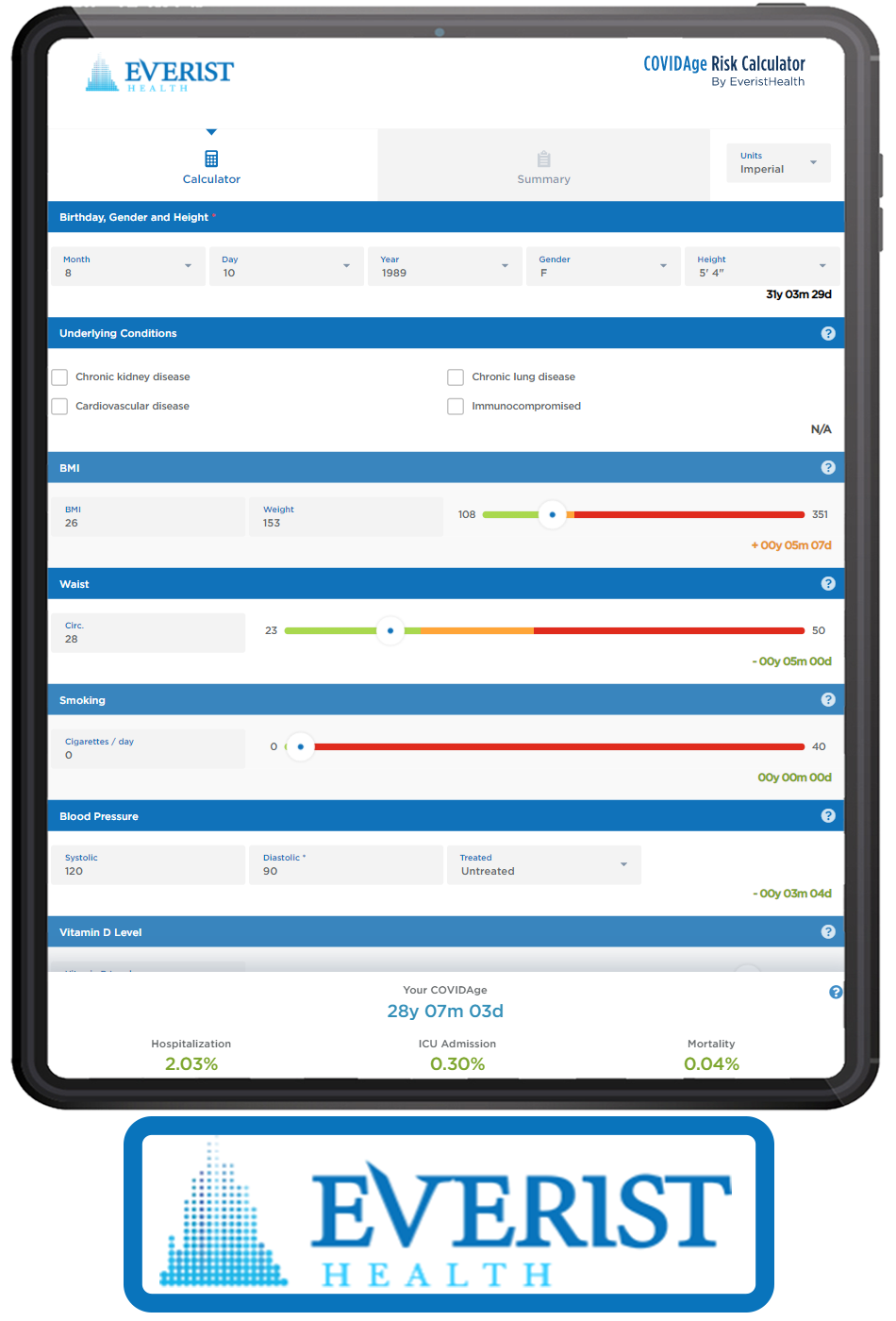
the battle between the ivory tower academics vs. the rogue cowboys An internecine war is brewing about the treatment of COVID-19. You can hardly
emcrit.org
This article makes some fine points about research infrastructure. I would also add that that money is a main factor in creating this divide.
1) Big Pharma profiting from an expensive new drug is a big motivator for protracted research. Whereas, more expeditious clinical research done on the front lines to learn what existing and cheaper modalities may help the patient do not bring windfalls. Look at the amount of time and money being put into the development of a vaccine, the mother-lode of all profiteering.
2) Today's medical education and practice is evidence-based in nature. Academia, medical organizations, and societies have fallen more on the side of "Let's wait and see." There is little willingness for systems of medicine (academia, hospitals) to break with this mentality. Throughout this crisis, I've observed the tendency of our facility (who is admittedly struggling to gather, discern, and apply all of the various pieces of data and research) to defer to 'the expert' recommendations as gospel. There is a large homogenization in today's medicine, for better or worse. This leads to less clinical sites being willing to step out of line and do something different, like a small, but possibly meaningful, study. I think we see more of a propensity to try 'unproven' modalities from outpatient practitioners because they are more distanced from hospital bureaucratic mentality (more autonomy), payment for modalities is the choice of patient, a patient with minor symptoms or early illness is potentially most helped by these modalities. We have a dichotomy of large, organized inpatient medicine (let's wait and see) and independent outpatient practitioners (benefit>risk).
3) In addition to the lack of RCT data, I also wonder if money and supply chain has played a role in the unwillingness of hospitals to trial other/existing modalities. For example, at my hospital, when I asked the ID pharmacist about why our treatment regime did not include an older, cheaper modality which had shown some evidence of usefulness with Covid, the answer I personally received was non-conclusive evidence of efficacy and the concern over supply chain issues (whether our facility would be able to adequately stock the volume of drug necessary for the recommendation.) I couldn't help but think about the waffling recommendations for public mask wearing, which went from 'no need' to 'highly recommended' based on PPE availability. I also wonder if inventory costs (relative cheap drug but in high volume) and lack of reimbursement were the nails in the coffin for this even being available for use at my hospital. In other words, did money play a role in treatment options? Of course it did. It always does. Why would this be any different?